[Updated December 3, 2018]
When I watch our dog, Pokey, nose his way over the prairie and through the woods around our homestead, I sometimes try to imagine what he is smelling. It’s an impossible assignment. The canine sense of smell and his repertoire of scents is, after all, at least hundreds of times and perhaps more than a million times more acute and more expansive than mine.
I watch as he trots ahead, nose just above the grasses, head ever on the swivel, left to right and up to down – air-sniffing, selecting scents, veering to wherever the pleasures of his nose takes him. Suddenly he stops, noses into a clump of grass, snorts, burrows his nose deeper into some fragrance I will never know, an odor that recalls some aromatic memory, perhaps a primitive recollection from even before he was born. He digs into the memory of odor. Digs with his paws for a while, snorts, then decides it is a lingering smell no longer worthy of his work. He rises up, glances my way … and then lifts his leg and marks this location for any who might follow.

The Canine Nose
The dog’s nose consists of a bony nasal cavity that is divided into two separate chambers by a bony and cartilaginous nasal septum. Within each of the cavities are the turbinate bones (conchae) and the paranasal sinuses.
The turbinate bones form into several scrolls of moveable cartilage and bony tissue that is lined with ciliated epithelial cells. The turbinate bones are a veritable maze of structure, and locating a foreign body hidden in their depths can be an extremely frustrating undertaking – a procedure that almost always requires general anesthesia.
The nose opens to the exterior via two external “nares” or nostrils and the ethmoid bone marks the posterior aspect of the nose.
The paranasal sinuses are extensions of the nasal cavity and various diseases or tumors may impair their drainage (especially of the frontal sinuses). When the dog sniffs, there is forced inspiration and the nostrils are dilated. The inspired air is warmed and humidified as it passes through the turbinates, and the mucus layer that lines the air passages serves as a filter to trap bacteria and particulate matter.
The dog collects scents by air-scenting (sniffing volatile oils that are traveling in the air) and sniffing the ground. A dog’s nose is ideally made for sniffing – the outer nares are mobile and allow for expansion on inspiration and contraction to prevent the entry of unwanted objects. When a dog sniffs, he inhales the scented chemicals into his nasal cavities, where they are trapped in mucus and processed by the sensory cells. Expiration forces air out the side of the nares so that its exit doesn’t interfere with odors still in the air or on the ground.
Several cilia extend from each of the sensory cells into the nasal cavity, and each of these cilia contains many scent receptors. After the cell receptors trap the smells, each cell has several (10 to 100) axons that deliver their messages back through the ethmoid bone directly to the olfactory bulb of the brain.
Once in the olfactory bulb, scents are transported to the frontal cortex for recognition as well as to other regions of the brain that include the brain’s centers for emotions, memory, and pleasure. There are many interconnections between all these centers, with the result that a simple smell, detected by a dog, likely has an entire set of meanings, memories, and emotional ties that only that dog can know and interpret.
Much of the deeper work of trying to understand the sense of smell has been done on humans; how do you ask a dog what he feels or remembers when he smells a certain odor? But we do know that dogs have much more surface area within their nasal cavities, and this area is well supplied with sensory cells – estimates of the total number of these cells vary and depend on the breed, but they have been cited as somewhere between 125 million and several times that. (This compares with estimates of human numbers that are in the 5- to 10-million-cell range.)
In addition, the dog has devoted a tremendous amount of his brain tissue to olfactory cells. (Some estimates allocate one-third of the dog’s brain to the chore of scenting.) All this adds up to a canine scenter that has thousands to millions of times the ability of his human counterpart.
We also know that we can use the dog’s incredible sense of smell to benefit mankind in ways we are only beginning to imagine. Today’s working scent dogs are involved in search and rescue (some dogs can follow a trail that is more than a week old), finding cadavers (dogs have even detected drowned people in a depth of 80+ feet of water), detecting explosives, firearms, and drugs, and even scenting tumors in human patients. Early work has begun to use dogs to test the breath of humans – to help diagnose internal diseases before they become evident with other methods.
Jacobson’s Organ
Inside the nasal cavity and opening into the upper part of the mouth is the final piece of the dog’s scent-related puzzle, the remarkable Jacobson’s Organ. Jacobson’s Organ is a “sense of smell” receptor that is actually not receptive to ordinary odors. Rather, the scenting nerve cells of the organ are quite different from those in normal olfactory tissue in that they respond to a range of substances that have large molecules, but often no detectable odor.
The sensory cells of Jacobson’s Organ (which anatomists claim are unlike any other nerve cells) communicate not with the olfactory bulbs and cortex, but with the accessory bulbs and the part of the brain that coordinates mating and other basic emotions. In fact, recent evidence suggests that the two separate but parallel systems of odor detection cooperate in surprising ways to produce novel sensibilities not achievable by either of them on their own.
The primary function of the Organ is to detect pheromones, which then provides both sexes with information as to the availability of the opposite sex for breeding. Additionally the Organ is apparently able to detect other, normally undetectable, odors – odors that may enhance the newborn’s ability to find its own dam, for example. Search and rescue dog handlers notice that many of their dogs lick the air, as if to give additional input into their “scents-ability.”
Animals enhance the sex-detection ability of the Organ with what is called the “flehmen” reaction or “flared face.” When exposed to the urine of an animal in heat, a male will typically throw back his head and raise or curl his upper lip – both of these help to open the entry slits into Jacobson’s Organ.
Horses, deer, and goats are the masters of this reaction, and many dogs can produce a rather pronounced flehmen when the time is right. Interestingly, although just a few years ago it was thought that Jacobson’s Organ did not exist in humans, a recent anatomical study of 400 human subjects confirmed both its presence and the fact that its nervous connections are capable of sending functional messages to the brain. Apparently, as much as some folks would like to deny it, we humans are indeed sexual animals, just like the rest of nature.
For Animals, Smelling is More Than Just Scent
The nose and the sense of smell are vastly expanded by Jacobson’s Organ, but an animal’s ability to smell extends into many other realms as well. Since smelling is hooked into the most primitive areas of an animal’s brain, there is reason to believe that smell is also linked to sensations created long before the animal was actually born.
We know, for example, that animals (and humans) prefer to mingle with the scent of members within their own pack or herd (or, in the case of humans, in their own culture), and horses and dogs can detect the human scent of fear. Also, shortly after birth, mothers are able to pick out their own offspring by smell, and puppies quickly learn the smell of their mother’s milk . . . and before long, the smell of a preferred teat.
We know that certain scents may be linked with memories of past events, and even with positive or negative emotions. The fragrance of cookies baking, for ex-ample, may remind us of the good times we had at grandma’s house, many years ago. Throughout our lifetime, then, the smell of fresh-baked cookies may evoke a positive feeling. It’s not easy to correlate long-lasting emotions to past events in dogs, but it is certainly something to consider when we are dealing with a behavior problem that we can’t explain physically; could it be related to some household odor that was associated with a bad experience in the dog’s past?
In traditional Chinese medicine, the nose – along with the throat and vocal cords – are all considered to be intimately connected to the function of the Lungs. Many nose and throat disorders are therefore treated through the Lung Meridian.
Nose Nutrition
In addition to the normally recommended wholesome diet for dogs, a few nutrients may be especially beneficial for the nose and its ability to smell. Vitamin A seems to be directly involved in the sensory cells’ ability to receive and activate the energy of odorant molecules. Glutamate has been proposed as the olfactory cell neurotransmitter (at least in turtles, toads, and rats). While these may prove to be helpful for smelling (especially in the older dog), no definitive studies have yet been done to ascertain proper dosages (or definite benefits) for dogs.
Remember that, as an animal ages, he loses some or all of his ability to smell. Older animals may need to be tempted to eat, and some seem to find spicy foods more palatable. Try several culinary herbs to see if your dog prefers any of them – most of the culinary herbs are high in nutrients and antioxidant, anti-aging activity.

In my opinion, the best “nutrition” we can give to a dog’s nose is a daily dose of natural odorants, generated from the fields and woodlands out of doors – the perfect way to build up the reserve of sensory cells and brain connections related to smelling.
Disease Etiologies
Viral infection is the most common cause of acute rhinitis or sinusitis in dogs, with canine distemper, adenovirus types 1 and 2, and parainfluenza the most frequently incriminated.
While primary bacterial sinusitis or rhinitis (inflammation of the mucus membranes of the nose – from the Greek “rhis,” meaning nose) is extremely rare in dogs, secondary bacterial infections are a frequent complication of viral infections.
Allergic sinusitis or rhinitis may occur seasonally in association with pollen production, or it may be the result of household and environmental irritants such as cigarette smoke, housedust, mold, irritant gasses, excess or abnormal odors (perfumes and perfumed air fresheners, for example), and exposure to toxic chemicals such as pesticides and herbicides.
If rhinitis becomes chronic, consider a persistent secondary bacterial infection after a viral infection, trauma, or presence of a foreign body, or the possibility of a tumor or fungal infection. Rhinitis or sinusitis may also result when a tooth root abscess extends into the maxillary region.
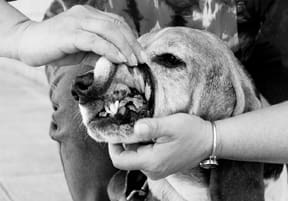
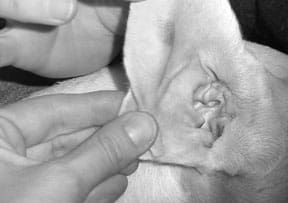
In the course of a normal smelling adventure, a dog will inhale a variety of foreign bodies, most of which are too small to worry about or are immediately sneezed out. Occasionally a dog may, however, inhale a splinter or a plant awn or some other small particle that remains lodged in the nasal cavity, causing local irritation and infection. Finally, both fungal and neoplastic disease may center in the nasal cavities, generally producing chronic symptoms.
Clinical Signs of Rhinitis
Acute rhinitis is characterized by one or more of the following: nasal discharge, sneezing, pawing at the face, respiratory stertor (snoring or sonorous breathing), open-mouthed breathing, or other signs of inspiratory difficulty. Tearing (lacrimation) and red eyes (conjunctivitis) often accompany upper respiratory inflammation.
There is often a nasal discharge that may be serous (resembling serum or watery in appearance), catarrhal (discharge created by the inflammation of a mucus membrane), purulent (containing pus or white blood cells), or hemorrhagic (bloody), depending on the degree of mucosal damage and on the increased amount of normal (or abnormal) secretions. The amount of discharge may also reflect decreased “grooming” of the nostrils with the tongue when the dog is ill.
Sneezing, in an attempt to clear the upper airways of discharge, is seen most frequently in acute rhinitis; as the disease progresses to a more chronic form, the sneezing becomes intermittent. The presence of a foreign body is suggested by frantic sneezing; an acute, one-sided nasal discharge (especially if it is bloody or tinged with blood); and possibly accompanied by pawing at the face or rubbing one side of the face against the ground. Neoplastic or fungal disease is suggested by a chronic nasal discharge that was initially unilateral but becomes bilateral or that changes in character over time (say, from serous to blood-tinged).
Pure sinusitis is not very common in dogs; sinus infections are generally associated with diseases of the nasal cavity. Epistaxis (bloody nose) is a rare occurrence in dogs and may be the result of recent trauma or the presence of a nasal foreign body or tumor.
Conventional Treatment for Nose Problems in Dogs
Since the primary etiologies of rhinitis and sinusitis are viral, supportive therapy may be the only conventional treatment available … and to be fair, most cases of rhinitis and sinusitis will resolve themselves with nothing more than supportive care.
Make sure your dog continues to eat and drink when he’s suffering from any sort of nasal problem; remember that most of a dog’s ability to “taste” food resides in her nose, and if she can’t smell the food, she may not want to eat it. Furthermore, even a mild fever will quickly dehydrate a sick animal, and if you can’t get her to drink at home, consider a trip to the vet for fluids.
Foreign bodies will need to be removed, most often under general anesthetic. Tumors of the nasal cavities can be nasty and will require the full concentration of a holistic veterinarian.
Alternative Therapies
Acupuncture treatments will most often be aimed at enhancing the immune function, and since the nose is connected through the Lungs, will often include treating the Lungs.
The Lung Meridian begins at the forward point of the shoulder and proceeds downward around the upper arm, extending along the medial aspect of the foreleg to end at the medial aspect of the first (inner) phalanx.
To help alleviate conditions involving the nose, massaging both forelegs from the shoulder down to the toes will stimulate all the Lung points and important immune-balancing points (LI-4 and LI-11). In addition, a massage of the neck and upper back, from the base of the head (at the occipital bone) back to the shoulder blades, will stimulate points along the Bladder Meridian that are correlated to the Lungs (Bl-13, at the third intercostal space, is the Lung association point, and Bl-9 at the base of the occipital bone, indicated for headache, neck pain, and nasal congestion).
LI-20, located just lateral to and slightly below the nasal ala (the fleshy part of the nostril), is specific for rhinitis, epistaxis, and facial paralysis. Sometimes stimulation of this point will cause an intense outflow of gunk from the nasal cavities, much like an artificial “nose-blowing.” Most dogs seem to tolerate needles in this point, but I’ve not had much luck trying to stimulate it with a finger (acupressure).
Everyone should learn one particular nose-related acupuncture point, GV-26, the point located on the lip at the center of the nose, just below the fleshy part of the nose. GV-26 is the most important point for acute emergencies such as shock, collapse, heatstroke, cardiac arrest, coma, severe bronchitis, or acute epileptic attacks. If a newborn puppy is not breathing properly or a dog is not recovering from anesthesia, this is the point to stimulate.
If you don’t have acupuncture needles, use whatever sharp object is at hand – a safety pin, knitting needle, your fingernail, whatever is available. For emergencies use strong stimulation – the “hen pecking” technique is appropriate here, rapidly jabbing the sharp object straight into the acu-point, about ¼ to ½ inch into the skin – much like a hen would peck at grain on the ground.
Homeopathic remedies can often be very useful, especially for the acute sinusitis or rhinitis, and the analysis of nasal symptoms can sometimes lead to a remedy that offers a cure for the totality of the patient’s symptoms. The problem is that nasal symptoms can also be extremely confusing in the initial case-taking.
To get some perspective on the magnitude of remedies listed for the nose, using the classical repertory, Kent’s Repertorium Generale, edited by J. Kunzli, there are 24 pages of remedies dealing with the nose alone. If we were to use nasal “discharges” as our key symptom, we would need to wade through almost four pages of remedies, each one applied to one of the 56 descriptive terms used to describe a specific type of discharge.
Additionally, when an animal is being treated with homeopathic remedies, external symptoms may be the last ones to clear up. Nasal symptoms are thus not the most reliable to monitor when you’re trying to decide which direction the case is taking.

Given all this, I still rely heavily on Aconite (30c, three times, the doses given 12 hours apart) when treating almost any acute nasal infection. My approach is to give the aconite at the first signs of rhinitis or sinusitis (or actually, almost any acute disease), wait a few days to monitor results, then (if any more treatment is needed) decide on which remedy to follow up with, depending on the specific signs seen.
Homeopathic remedies have shown some success when treating nasal tumors, and if a tumor is diagnosed in your dog, it is certainly worthwhile to consult with a holistic veterinarian who has experience treating them homeopathically.
Herbal Medicines for Nasal Health in Dogs
Herbs that may be helpful for treating rhinitis and/or sinusitis include a mixture of two or more of the following:
• Elder flower (Sambucus nigra). Has anti-catarrhal effects and is tonifying to mucus membranes
• Goldenseal (Hydrastis canadensis) or Oregon grape root (Berberis aquifolium). Antibacterial and antiviral
• Goldenrod (Solidago virgauria). Anti-inflammatory and anti-catarrhal
• Peppermint (Mentha piperita). Decongestant
• Yarrow (Achillea millefolium). Especially beneficial if the disease has become chronic and is accompanied by fever
• Echinacea (Echinacea spp.). Aids the immune system
Mix the herbs chosen in equal amounts and brew a mild tea from the mixture. Cool and pour the tea over the dog’s food – about 1/4 cup of tea per 20 pounds of dog, one to three times daily. Alternatively, sprinkle the mixed herbs (fresh or dry) on the dog’s food – about a teaspoon of herbs per 20 pounds of dog, two to three times daily.
Aromatherapy
Aromatherapy is directly applied through the animal’s ability to sense odors that in turn are directed to various parts of the brain. The effects on the brain centers depends on the flower essence used, and an entire repertory has been developed to help the practitioner and a dog’s caretaker decide which aroma may be beneficial for the condition.
While the development of aromatherapy treatments for animals remain a work in progress, recent studies using electro-encephalograms (EEGs) confirm that at least some of the aromas do affect brain centers just as they are supposed to.
One study in particular shows that rosemary depresses alpha-activity (i.e., acts as a stimulant) and ylang ylang enhances it (providing relaxation) – just as the aromatherapy “textbooks” say they should. In aromatherapy, rosemary is used as a stimulant and ylang ylang is a soothing, relaxing aroma. In addition, one trial demonstrated that kenneled dogs bark less when they are exposed to the soothing aroma of lavender.
Flower Essences
Flower essences can help alleviate any emotional upset that may come along with problems that involve the nose, and there are some essences that may speed up the healing process. Crab apple is good for general detoxification, and cedar may be helpful whenever environmental or chemical toxicants are involved. Salvia supports an immune system under stress.
Dog Noses & Sense of Smell: Summary
The dog’s nose may be his most powerful organ and it is certainly one of the most dynamic of all animal systems, with activities that range from basic smell detection, to sensing fear, to memory, to emotions, to mate- and pack-selection, on to a genetic history carried from one generation to the next. Fortunately, disease doesn’t often waylay its functional capability, and fortunately again, most of the diseases of the nose are easily treated naturally.
What You Can Do
1. A runny nose should always warrant further inspection and monitoring. Consult your holistic veterinarian if symptoms persist.
2. If your dog comes in from a walk outside and has an acute attack of sneezing that doesn’t resolve within 20 minutes or so, take him right to your veterinarian. He probably has inhaled a foxtail or other plant awn, and will need anesthesia to remove it.
Want more cool facts about dogs’ sense of smell? Click here!
Dr. Randy Kidd earned his DVM degree from Ohio State University and his Ph.D. in Pathology/Clinical Pathology from Kansas State University. A past president of the American Holistic Veterinary Medical Association, he’s author of Dr. Kidd’s Guide to Herbal Dog Care and Dr. Kidd’s Guide to Herbal Cat Care.