There are few things as frightening as watching your dog have a seizure. Yet seizure disorders are surprisingly common in canines. A seizure is defined as uncontrolled electrical activity in the brain. Seizures can run the gamut from very minor, focal seizures (a twitching of the face or a leg) to major convulsions in which a dog loses consciousness, may vocalize loudly, has uncontrolled muscle movements, and loses bowel and/or bladder control.
Types of Dog Seizures
A seizure or “ictus” is comprised of three phases. The pre-ictal phase can begin as much as 24 hours before a seizure and is not always obvious. Your dog may act strange during this period, but this is usually only recognized in retrospect. The second phase is ictus (the seizure itself). In the third, or post-ictal period, your dog is recovering from the seizure. It can be stressful and disturbing to witness, and it varies significantly between dogs. The post-ictal stage can include a deep sleep that lasts several hours to an entire day, confusion, and abnormal behavior, including ravenous hunger or complete anorexia, dilated pupils, and in some cases, blindness that will resolve. Your dog may be disoriented for a short time, but this period is otherwise not dangerous.
In the past, seizures have been categorized as grand mal (French meaning “great sickness”) or petit mal (“small sickness”). These terms are no longer used to describe seizure activity, as they are considered too vague. The more recent classifications are tonic-clonic, clonic, and tonic. Seizures can also be described as generalized, focal, or psychomotor.
In a tonic-clonic seizure, the first, very short phase is the tonic. The dog will suddenly stiffen and collapse if standing. Next is the clonic phase, in which the muscles contract and relax rapidly. This is the type of seizure with which most people are familiar. It is often called a convulsion and represents the most common, generalized seizure type in dogs.
A tonic seizure is usually brief (less than one minute) and involves a sudden stiffening of the muscles. This is a less common manifestation of a seizure disorder. A clonic seizure is rhythmic muscle jerking that generally starts in one area of the body. It is very rare and often associated with canine distemper virus. Both a tonic seizure and a clonic seizure can be generalized or focal.
Psychomotor seizures often manifest as unusual behavior, such as “flybiting” at the air or staring into space and not responding to cues. Sometimes, they are called “absence spells,” as the pet seems unaware and unresponsive to his surroundings.
Seizures can last from seconds to hours. When a seizure doesn’t stop after a few minutes, it is called status epilepticus. In this scenario, the body temperature will start to go up due to the repeated muscle contraction, and heat stroke can result. A dog’s body temperature can elevate to as high as 110 degrees or more if the seizure is not interrupted. Prolonged hypoxia (low oxygen) to the brain due to seizures can also cause damage. Status epilepticus is always an emergency.
Medical Emergency: Status Epilepticus
Status, as it’s commonly called, occurs when a seizure persists and will not stop without medical intervention. This is always an emergency and requires veterinary attention. Benzodiazepines like Valium will be given intravenously to stop the seizure. Your dog may need to be cooled to prevent heat stroke. He may need to stay on a continuous infusion of medications like Propofol (an anesthetic) to break the seizure cycle and allow recovery. This can take two to four days in some cases. The prognosis is guarded for recovery.

Dog Seizure Causes and Diagnostics
Causes of seizures can be divided by age group:
Dogs Less Than Six Months
A dog of this age with sudden onset of seizures likely has a congenital problem, infection with parasites such as Neospora, infection with a virus such as canine distemper or rabies, or toxin exposure. Epilepsy at this age is extremely rare.
The first step of evaluation is, as always, a thorough history. Puppies are prone to ingesting toxic substances such as rat baits and gum sweetened with xylitol. As a result, if your puppy presents with seizures, your veterinarian will recommend a thorough diagnostic work-up. This will start with a complete blood count (CBC) and chemistry panel, urinalysis, and fecal examination.
Bloodwork will evaluate for metabolic causes of seizures, such as liver failure, electrolyte abnormalities, or low blood sugar. A urinalysis will help determine how the kidneys are functioning, as well as look for evidence of any inflammation or infection within the urinary tract. Your vet may also recommend specific blood tests to rule out parasites such as Neospora caninum and Toxoplasma gondii.
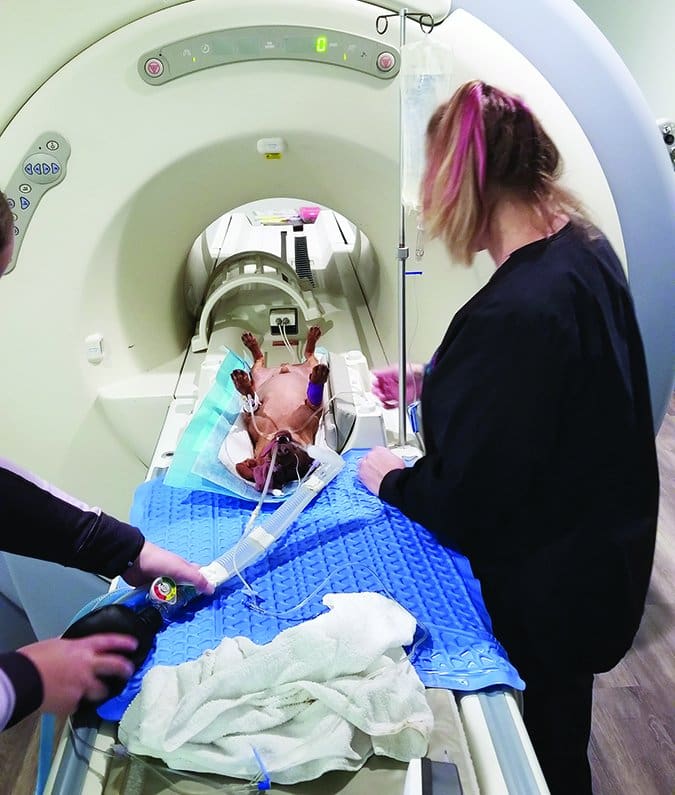
If those tests do not reveal a cause, your vet will refer you to a specialist for a cerebrospinal tap and imaging of the brain such as an MRI or CT scan. Because epilepsy is very rare in dogs this age, it is important to find the cause of the seizures. Without definitive diagnosis, the underlying condition is likely to worsen, as are the seizures.
If further testing is not financially possible, your veterinarian will start empirical treatment based on the suspected underlying cause. This may or may not be effective.
Dogs Aged Six Months to Five Years
Epilepsy becomes the most likely diagnosis in this age group when other causes are excluded. Epilepsy is not a disease per se. It is a description of seizure activity for which no underlying cause can be found.
A diagnosis of epilepsy cannot be made definitively until every other cause of seizures is ruled out. The tests needed to rule out an underlying cause can be expensive, however, so this diagnosis is often made based on breed, clinical signs, and response to treatment. Beagles, Schnauzers, Collies, Cocker Spaniels, and Basset Hounds are predisposed to epilepsy.
Your veterinarian will recommend the same set of diagnostic tests as for puppies and likely add a blood pressure measurement, thyroid levels, and x-rays of the chest and abdomen. If those are normal, the next steps are imaging of the brain as outlined above. In most cases, owners do not opt for the advanced testing and instead treat the suspected epilepsy with anti-epileptic drugs (AEDs).
Dogs Older Than Five Years
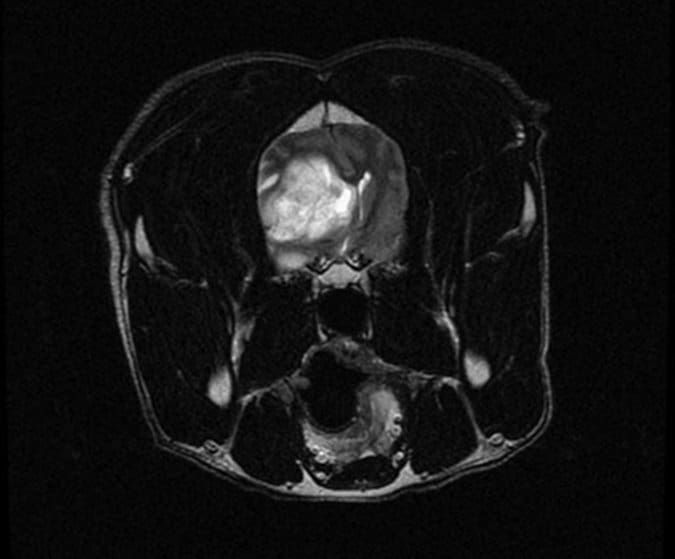
In dogs older than five, the most common cause of seizures is a brain tumor. These are generally benign tumors, such as meningiomas. Seizures can result from the tumor pressing on nearby structures as well as from swelling around the tumor.
The same diagnostic algorithm is followed as above, and again, many owners opt to merely treat the seizures without an in-depth exploration of the causes. While brain tumors are generally benign and can be removed via surgery, they are invasive and carry a guarded prognosis for recovery.
The causes of seizures are vast and varied. They can be broadly divided into extra-cranial (outside the brain) and intracranial (inside the brain).
Extra-cranial diseases include metabolic disease such as liver failure, toxin ingestion like xylitol or bromethalin rat poison, insulinoma (a tumor of the pancreas causing low blood sugar), infectious diseases like rabies and canine distemper virus, parasitic infection, and electrolyte derangements.
Intracranial causes are almost as varied and include cancer, inflammatory conditions such as necrotizing encephalomyelitis, previous head trauma leading to scar tissue formation within the brain, and vascular abnormalities like blood clots.
Dog Seizure Treatments
The first step in treatment may be nothing at all. If seizures are short and not frequent, treatment may not be necessary.
While they are difficult to witness, if the seizures are brief (under five minutes) and self-limiting, then they are not dangerous to your dog. In this case, your veterinarian may not prescribe medication but simply have you keep a “seizure journal.” This involves writing down when the seizures happen, what could have precipitated them (stress, anxiety, sleep), how long it lasted, and how long it takes your pet to recover. Your veterinarian will use this log to help dictate when to start treatment and what treatment to start.
In 2016, the American College of Veterinary Internal Medicine (ACVIM) released a consensus statement regarding when to start AED therapy. In general, if the seizures are mild and infrequent, therapy is not recommended. If they are severe and frequent, or the dog has a history of previous head trauma, or if there is an obvious lesion on CT/MRI (such as a brain tumor), AEDs should be started.
If the seizures are becoming a problem, medication is the first step. There are four commonly used AEDs in veterinary medicine, but more drugs are currently under study and are tentatively being used.
The most commonly prescribed first-line medication is phenobarbital, although this is slowly changing. “Pheno,” as it is frequently called, has long been used to treat seizures in humans and animals, so the effects and side effects are well-known, and the drug is readily available and inexpensive. It is also very effective. Unfortunately, it does have side effects such as sedation, weight gain, panting, increased appetite, and increased liver enzymes.
Phenobarbital is usually given twice a day and is a controlled substance under FDA regulations. It should not be stopped abruptly, as this can lead to more seizures. If you start administering this drug to your dog, make sure you are always prepared with refills before you run out! This will require at least a yearly examination with your veterinarian to maintain a valid client-patient relationship (VCPR).
Your veterinarian will also recommend monitoring of liver values and phenobarbital levels, likely on a bi-annual or annual schedule. This will help determine the effects that phenobarbital is having on your dog’s body. It will also assist your veterinarian in determining how much more (or less) phenobarbital your dog can receive.
About 30 percent of dogs will achieve good seizure control on phenobarbital. Greater than 75 percent will have a significant reduction in seizure frequency. About 30 percent of dogs will require an additional drug to control their seizures.
Historically, potassium bromide has been the next drug of choice. This is changing, as more and more veterinarians are becoming comfortable with and using newer AEDs. Potassium bromide also causes sedation and can be associated with pancreatitis, as well as a condition called bromism (bromide toxicity). It is being used less as newer drugs replace it.
The two newest AEDs are levetiracetam (Keppra) and zonisamide (Zonegran). Keppra has been used in humans in the U.S. for the past 10 years. It has very few known side effects and does not damage the liver. It is safe to use in patients with compromised kidney or liver function and does not generally cause drowsiness. It requires dosing every eight hours and can be expensive for larger dogs. An extended release formulation is sometimes available and can be given twice a day. It is also less cost effective. Unfortunately, there are few studies to evaluate how well it works in canines, so Keppra’s use is currently anecdotal. As time passes, there will likely be more evidence for its usage, more generics available, and a twice-daily formulation will become readily available.
Zonisamide is similar to Keppra. How it works to prevent seizures is not clear. It has possible side effects of sedation, decreased appetite, ataxia (wobbly walking), and might contribute to liver and urinary problems, though this has not been proven. It is also given twice a day.
In some cases, one drug can control seizure activity. In others, multiple seizure medications are needed.
Recently, a veterinary therapeutic diet was released by Purina that may significantly improve seizure control when given with medications. This diet uses medium chain triglycerides (MCTs) as the fat source. These MCTs have an anti-seizure effect and can improve control in conjunction with medication therapy.
Your veterinarian may send you home with an anti-seizure medication to apply into the rectum or nostrils if your dog has a seizure.
There are other, less mainstream treatment options such as vagal nerve stimulator implants. These are not commonly done and are only used in the most refractory cases.
Catherine Ashe is a 2008 graduate of the University of Tennessee College of Veterinary Medicine. After nine years in emergency medicine, she now works as a relief veterinarian in Asheville, North Carolina.






my dog (2 year old male shih-poo) had a convulsion this morning, same symptoms as a tonic seizure. he got up and started throwing up, he then fell on his side and his body became stiff. His glands then opened up and he starting defecating. I panicked and began yelling, after realized I created more stress. My mom came in the room where he showed rare signs of aggression, he than calmed down. Whole thing lasted about 2/3 minutes. What can be the cause to all of this, and what can be done naturally to prevent this from happening again. he eats homemade food, no commercial. Someone please shine light to this situation
My chi gags then whizzez alot more and more had two seizure since gaging or something’s stuck o. His throat, he gets stiff makes a god awful Howell then kinda weak but if I take him out side where it’s cold here in Oregon he seems much better but could he die from this . Like be so scared his little heart could give out??? What can I do to make him more comfortable in his life .
I am not sure if anyone reads this anymore… My yorkie that is 3 years old recently started having seizures. He has otherwise been extremely energetic with normal behavior. He has had about 5 so far (that I have personally seen) I think he might have had more while I am asleep, as a couple have been in the middle of the night and woke me up. Every single time I panic and cry because I am so worried. He is literally my everything and it is so hard to watch them go through this. He is on keppra but still getting these every two weeks. I have already spent over 2k in vet bills and now the next step is the MRI….. just under 5k here!! I love him so much and obviously will fork this out, however it is going to be really hard for me to afford. This will be 7k in just two months or less… I am really looking for any advice or tips for dogs this young with seizures. If they do not find anything in his x-rays there has to be some sort of relief when these pills are not working. As you know, seizures are so traumatizing to all involved. He is only 8lbs and it is so hard to watch this little guy endure this. It breaks my heart. If you have any tips…. diet, best pills that worked for your furbaby, etc. Would be greatly appreciated.