They are among the words you least want to hear: Your dog has cancer. But the odds are you will hear them someday, especially if you have more than one dog in your lifetime. One in four dogs get cancer; half of the dogs over 10 years of age die from or with it.
Much of what is known about canine cancer closely parallels what is known about cancer in humans. Dogs are at risk of the same types of cancer afflicting humans, and treating canine cancer successfully is dependent upon the same variables found in human cancer treatment: the type of cancer, the wisdom of the attending doctor in choosing the most effective course of treatment, the availability of advanced medical techniques, and the willingness and ability to pay for them.
There are other similarities. Statistically speaking, cancer is a disease of middle and old age. Certain cancers are largely preventable with prudent lifestyle choices. Early detection is almost always a critical factor. Cancer is hereditary, sometimes running in canine families. Variables like nutrition and toxic exposure seem to play a prominent role.
And always there is a highly individual response to disease. For some dogs, the immune system rallies, and the treatments seem magically precise. For many, if not most, treatment becomes a holding pattern, an evolving equation of modulated therapy versus quality of life. For still others, hope fades as quickly as the once-playful antics of a dog’s life.
Detecting Cancer Early is Key to Survival
Just as with humans, early detection offers by far the most realistic hope for your dog’s survival, particularly for those cancers which aggressively metastasize. Make it a regular practice to examine your dog’s body for unexplained swelling or lumps. Tumors developing in the upper layers of skin are the most common types of cancer in dogs.
Many early warning signs of cancer, however, are more subtle. While many of these signs – behavioral changes, loss of appetite, increased water consumption, persistent wheezing or coughing – are universal and require only basic observational skills on the part of the owner, other signs require a more sophisticated knowledge of your own pet.
Cancers are often traced to the site of earlier injuries, traumas, wounds, or fractures, so knowledge and examination of these injury sites can be helpful.
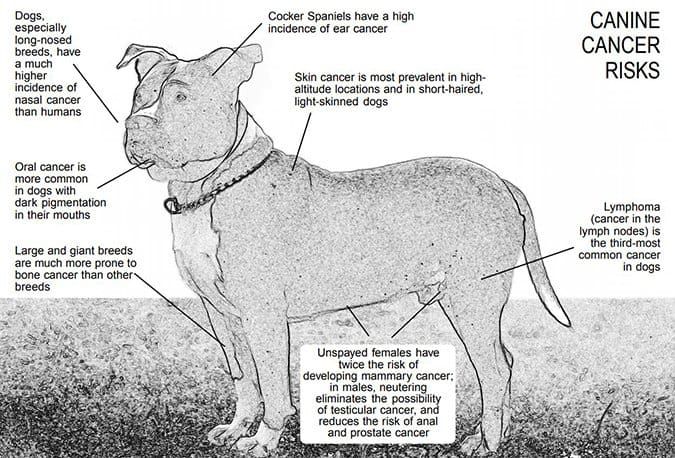
Dogs with long snouts and dogs who live on commercial farms, exposed throughout their lives to herbicides and pesticides, are more prone to nasal cancer.
However, dogs in general have a higher incidence of nasal cancer than humans. This, as they say, is a lifestyle issue; a dog keeps his nose to the ground, sniffing up whatever carcinogens happen to be present.
Oral melanoma, the fourth most common type of canine cancer, is much more common in dogs with dark pigmentation in their mouths. If you own such a dog, you need to be especially alert to unexplained oral swellings or signs of dental disease.
Mast cell tumors are common, but far more common in short-nosed breeds like boxers and Boston Terriers. Large and giant breeds are at much higher risk of developing bone cancer, particularly in the long bones of the legs. Cocker spaniels are prone to an otherwise rare type of ear cancer. Skin cancer is prevalent where ultraviolet light is strong, and particularly for short-haired, fair-skinned breeds like Boxers.
Before buying a certain type of dog, you should ask several breeders about the prevalence of cancer in that breed, and in that particular canine family. Heredity is a major determining factor in cancer; it is thought that boxers, for example, are more prone to cancer than any other bred. These statistics should not necessarily make you shy away from that breed, but inform your level of vigilance.
You should also be aware that, as in humans, there are cancer-causing genes, called oncogenes, which are more prevalent in one family than another. As dogs age, they are increasingly prone to both growths on the skin, and to fatty deposits just under it. Most often these growths are benign, but even a veterinarian can’t reliably tell just by looking. It is crucial to aspirate (withdraw cells via a thin needle) and, if necessary, biopsy (analyze the tissue sample under a microscope) these growths upon detection.
Even benign growths should be monitored closely; they have the potential to become cancerous. In addition, a dog might have a number of seemingly identical growths, of which only one is malignant.
As your dog ages, the likelihood increases that your dog will get cancer in any of one hundred different forms. Simple awareness, clearly, can go a long ways toward providing a happy outcome.
Diagnosing Cancer in Dogs
Approximately one in four dogs will get cancer; nearly half of all dogs reaching 10 years of age will die of it. Although we don’t know, in any given dog, precisely what factors caused a particular type of cancer, we do know that cancers seem to derive, over time, from an immune system stressed by toxins, injuries, poor nutrition – and probably stress itself.
If cancer is suspected, your veterinarian will order a series of tests leading to a diagnosis. These tests might include, depending on the cancer in question, aspiration, biopsy, blood tests, urine tests, x-rays, and ultrasound.
In some cases, your veterinarian might recommend exploratory surgery, or even one of the advanced, accurate, and expensive scanning technologies available to human patients.
When a cancer is present, however your veterinarian has arrived at the diagnosis, he or she should present you with a realistic prognosis. This process, called staging, identifies both the extent of the cancer’s spread (metastasis), and determines the treatment options available.
Common Canine Cancers:
Lymphoma
Lymphoma, also known as Lymphosarcoma, is a cancer of the blood cells and tissues associated with the lymphatic system. Generally afflicting middle-aged and older dogs, it is a cancer whose most common type (other forms originate in the gastrointestinal tract, chest, skin, or bone marrow) involves multiple external lymph nodes.
Frequently examine your dog’s body for abnormalities; it is of particular importance here, as lymphoma is the third most common cancer diagnosed in dogs. It is usually a simple matter to locate swollen lymph nodes at the base of the jaws, in the rear legs behind the knee, armpits, groin, and in front of the shoulder blades.
While true cures, for all practical purposes, remain out of reach, lymphoma responds exceptionally well to chemotherapy; what constitutes an acceptable quality of life, however, will sooner or later be the overriding issue for you as a dog owner.
Osteosarcoma
This aggressively malignant bone cancer most often strikes large or giant breeds, typically in the long bones of the legs. It tends to spread to the lungs very early in the course of the disease, and accounts for some 80 percent of the primary bone cancers found in dogs. The median age at diagnosis is seven years. In addition to targeting large dogs (only five percent of cases occur in dogs less than 25 pounds), osteosarcoma has also been linked to dogs with previously broken bones, and with hairline fractures occurring when bone growth was incomplete.
Initially, osteosarcoma might be labeled a mere sprain, but persistent symptoms later lead to a correct diagnosis, which is invariably grave. While new techniques are emerging, amputation is still the therapy of choice, since it removes both the primary cancer site and the primary source of pain. With amputation alone, however, only 10 percent of patients survive a year. When chemotherapy is applied, the one-year survival increases to 50 percent.
Skin Tumors
Dogs are prone to a great many classifiable lumps, cysts, growths, deposits, and tumors, the majority of which prove benign; some 20 percent are malignant or, rarely, become malignant over time. Because these growths are a normal part of the aging process, it is important to keep an eye on them, and bring them to your veterinarian’s attention.
The three most common types are called histiocytomas, or button tumors; lipomas, or fatty tumors; and mast cell tumors, which are by far the most serious.
Fatty tumors, to which breeds like the Labrador Retriever are prone, are unsightly but not dangerous in most cases. Most dogs, if they get any at all, will have more than one. Most veterinarians aren’t eager to remove them unless they inhibit the dog’s quality of life – they can reach the size of baseballs – by growing in an armpit or the crook of a knee.
Histiocytomas are referred to by what they resemble on the skin – raised, red, and often angry-looking “buttons” of rough tissue. Appearing in a spot where a dog is forced to leave them alone, they sometimes disappear without treatment. However, dog owners should never wait for the situation to resolve itself. Again, tumors cannot be safely identified by sight alone, even by experienced veterinarians.
It is the nature of mast cell tumors that they are very difficult to remove surgically, and surgery is the standard protocol. For this reason, veterinarians often recommend radiation and/or chemotherapy in conjunction with surgery, depending on the tumor’s appearance when the dog is brought in. In its early stage, this cancer is of uniform appearance (in medical terminology, “well-differentiated”), and can often be successfully excised. Otherwise, it is known for metastasizing to almost any part of the body.
Mammary Cancer
The risks of this largely preventable cancer are directly correlated with whether, and when, a female dog has been spayed. (While extremely rare, this cancer also occurs in males). For those dogs not intended to be bred, owners can virtually eliminate the risks of mammary cancer by spaying prior to the female dog’s first heat.
Mammary cancer, like most canine cancers, is closely associated with age. The average age of onset is ten years, and probably half of all cases are benign. And even for malignancies – almost alone among the serious dog cancers – this one has a significant rate of cure, but only when caught early, and the tumor is still localized. When the cancer has spread, the treatment goal hinges on quality of life issues, rather than possible cures.
Oral Melanoma
There may very well be a lifestyle link with this common and often grave cancer.
According to the most prevalent theory, carcinogens lodge on a dog’s coat, and are absorbed into oral tissues as a dog grooms. Even long-banned chemicals like DDT remain in the environment. Airborne carcinogens, in particular, settle to the ground; many of us fertilize our lawns, or spray pesticides in our gardens.
Because dogs spend their lives at toxicity’s ground zero, the potential for cell-altering damage is high. Fortunately, a major positive benefit of the growing emphasis on canine dental care is that this type of cancer can be diagnosed early.
Unless complete surgical removal is possible (and only follow-up x-rays will reveal if the cancer has metastasized), the options, once again, will be limited to a patient’s quality of life.
Preventing Cancer in Dogs
Of course, there is no magical diet, supplement, or vaccine that prevents cancer. But, as a dog owner, you can make some relatively simple choices to improve the odds.
As already mentioned, early spaying enormously reduces the risk of mammary cancer in females. Dogs spayed prior to initial estrus carry only half the risk of those spayed after the first but prior to the second heat cycle. Dogs spayed as young adults, or never spayed at all, have a risk factor increased by several hundred percent.
In male dogs, testicular cancer is common; neutering, obviously, eliminates that risk, and reduces the risk of both cancerous and non-cancerous prostate conditions, as well as anal cancer. (For show dogs and other unneutered males, fortunately, canine testicular cancer rarely spreads, and therefore has a relatively high rate of cure.)
Pale-skinned dogs have a higher risk of skin cancer. A striking example of this risk is the Dalmatian, a breed currently high in popularity. Cancer is known to surround – but not enter – a Dalmatian’s black spots. If you own a fair-skinned, short-haired breed, it would be best to limit your dog’s sun exposure, especially at the times of day when the sun’s rays are the most direct.
Moving beyond these few proven risk factors, however, takes us into the realm of nutrition and environment, where the human experience may or may not apply to our dogs as well. However, common sense – and growing clinical evidence – tells us that it does.
Environment
It isn’t any secret that the fewer environmental toxins our dogs are exposed to, the better. Long-term toxic exposure can destroy a dog’s liver, and weaken the immune system, which is the first and last line of defense against cancer.
Limiting your dog’s exposure to toxins is harder than you might think, however. After all, our dogs spend their lives on the earth’s most toxic layer, the ground, and in contact with the toxin-covered surfaces in our homes: carpets which have been cleaned with potentially harmful chemicals, floors which have been sprayed with ant and roach killer, garage floors which have absorbed all sorts of toxins.
Then there are all the chemicals we pour onto our dogs, most notably, flea-killing chemicals of every description: powders, sprays, shampoos, dips, and ointments.
The Prevention/Nutrition Link
Free radicals are active chemical substances which react with and alter our body’s cells. Those most capable of damage are associated with food additives, pesticides, air pollution, and radiation. It is thought that these damaged cells can “lose” their genetic programming, which limits and controls cell replication. Cancer, by definition, is uncontrolled cell growth. As is by now well-known, there is strong evidence that antioxidants (such as vitamins A, C, E and many other nutrients) help to neutralize free radicals absorbed from our environment. In theory, neutralizing free radicals could be a potent cancer preventative.
All of us “get cancer”; we probably have cancerous cells present in our bodies at all times. A properly functioning immune system will detect these cells and eliminate these cells before “cancer” takes hold. Cancer kills us when our immune system fails.
For dogs, and dog owners, the best possible advice suggests maintaining our immune systems at optimum levels through nutrition, weight control, and regular exercise.
Dr. R. H. Anderson, an holistic veterinarian in Dallas, Oregon, suggests a health-building and disease-preventing protocol for all his clients, and as a result, says very few of the clients who have followed the protocol end up developing cancer. “I have my clients work up to feeding their dogs at least a 50 percent natural diet. I clean up the dogs’ livers, and I make sure their immune systems are functioning normally. Every dog is different, but these three things seem to work pretty well.”
Cancer Treatments for Dogs: Traditional, Holistic, and Experimental
In the next issue of WDJ, we’ll examine the world of canine cancer treatments – conventional and unorthodox – as well as describe the most promising developments in cancer research.
Knowledge of the latest treatments is helpful, but it doesn’t alter cancer’s basic conundrum: What is the best outcome for my dog, and how do we get there?
Many holistic veterinarians believe that some conventional cancer treatments are pointless, inhumane, and often counterproductive. Many mainstream veterinarians roll their eyes at the very suggestion that alternative therapies are effective – or even more effective – than modern drug and radiation therapies.
While no one can give any definitive answers – every dog is different – in our next issue, we will tell you about the best treatment options available today, and what those options will look like in the future.
Roger Govier, a freelance writer and frequent contributor to WDJ, lives in San Francisco, California.






We have rescued a number of medium sized dogs and cats over the past 22 years and fed them Evolution Diet organic and non gmo plant protein – plant oil pet foods. The Evolution company does not use chemical preservatives or chemical mold inhibitors in any of their foods and again they make organic, non gmo pet foods. We also keep our dogs from walking on chemical sprayed lawns and we use only the very minimum rabies vaccines required to keep dogs legal: we do not use them with our indoor cats. We use no other vaccines or pesticides with our dogs or cats. We wash our floors once per week as well as vacuum our seating and pet sleeping surfaces. We spray our dogs with bottled lemon juice on the front, back, upper and lower body once or twice per week during the warm months to repel fleas, ticks and mosquitos. We comb our dogs and our cats about once per week to remove hair and dander. Our veterinary bills are almost non existent and although the Evolution Ultra Life Food or Evolution Maximum Life Foods are more expensive then store bought food we have had some of our dogs live into their late mid to late teens and 2 that exceeded 21 human years. One of those dogs was a medium sized Dachshund named Rusty and the other was an Australian Shepherd name Trina. Several of our cats have lived into their late teens and early twenties. I will not tell you that dogs or cats live any longer using Evolution pet foods than any other pet foods because this was not a study result, but it was what we have experienced.
My Beagle always had home cooked food. I fully believe his Lymphoma was caused by over vaccinations. There were times where we would be at the vet and he was due for 3 shots, and 2 more in a couple months, and they would say, do you want to just give them all to him now? I had no idea dogs only need most shots just once in their life and not get boosters year after year. Don’t let any vet do this to your dog. It’s the one common denominator among all dogs that get cancer. There are other causes, pesticides, flea and tick meds that are toxic, bad dog foods, most of which are garbage, but the most common of all is shots. I lost my boy at 8 years old even after 6 months of chemo. It only bought him a couple months of remission in the end, and I will be heart broken forever.
Another explanation for the increase in canine cancer is simply because dogs are living longer. Just like humans, our lifespan has increased so the chance for cancer also increases. If you are worried about food then home cook and give them supplements. The genetic component is the main deciding factor.
Can’t find the Cure for Cancer if the Cause of Cancer isn’t known. Very disappointed in this article and the one line reference to Nutrition. Why is it that cancer in dogs has increased to a rate of 50% dogs die of cancer? Why did dogs, a few generations ago, just grow old and die quietly before all the marketed False Food flooded the shelves and TV? Could it be it’s because of the un-natural, processed Kibbles and Canned Foods manufacturers have pet owners believing is the “best choice” for their pet? Imagine feeding your children candy and McDonalds burger every day for 10 years? Do you think “enriching” these over cooked foods with chemically made vitamins will render this better? How about switching to Real Food – yeah, spending a little time in the kitchen for food preparation – what a concept! Common sense says if the Immune System is strong, your dog will have a better chance resisting dis-eases. Without living in a constant state of inflammation due to poor digestion, the Immune System has more chance of eliminating freaked-out cancer cells. Then move on to creating an environment that is free of lawn chemicals and pesticides, dyes, and so forth. It is really sad that Big Business has propagated the revolving door called dis-ease.
Over the Past 50 years dog foods such as Iams,pedigree, purina, science diet, and alpo have all been commercialized and those are all dog foods that have a known Carcinogen found in tobacco products and is a preservative found in dog food (GHB) you basically have been feeding your dog cancer for the last 5 OR 6 decades. It is in the dog’s genes to develop cancer now you know cancer wasn’t as prevailing in dogs 20-30 years ago because it wasn’t a part of their genes like it is now because dogs have been eating the same terrible dog foods for so long it’s now bred into them and that’s why dogs are doomed, as 1 in 3 dogs will develop cancer. It’s the food that had been fed to them many years ago it’s hard to reverse what’s already been done.
Can dogs die from selective crop spays, which kill all other plants but the crop planted in the same field. We live directly across the road from a farm that decided to rent their land to another farmer, who wanted to grow only barley. He sprayed the entire field with a Phyzer chemical product that killed all the grass, but didn’t touch the Barley. Both of our beloved dogs died from Cancer, within two years of this product being applied. We think it drifted over to our property line, directly across the road from the field it was used in. Does Phyzer have chemicals products that are dangerous to dogs and can cause them to get cancer and die from their useage?
Graham Hawkridge
Pontypool Ontario
Canada
L0A1K0