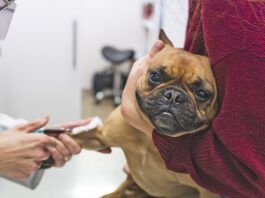
Dog Ear Infections: Symptoms, Causes, and Treatment
While inner-ear infections occur more in dogs with drop ears, like Cocker Spaniels, any dog can experience an ear infection. Infections can be in one or in both ears. A proper diagnosis of ear discomfort will usually require ear cytology.
Pancreatitis in Dogs: Causes, Symptoms, and Treatment
While there are hundreds of reasons for not eating in dogs, if your dog is not eating, pancreatitis is a possibility, especially if your dog has symptoms of pancreatitis like not eating, vomiting, diarrhea, abdominal pain, and fever.
All About Anal Glands in Dogs
Anal glands in dogs are two small sacks that sit on either side of the anus. They can become full which causes discomfort, and they can leak which causes foul odors.
How to Handle Dog Skin Conditions
Dogs can have many different skin conditions. Some skin problems are minor and easily fixed, while others are trickier to diagnose. Some may be controllable but not curable, while others can be cured. It makes sense with any skin condition to begin with basic treatment options, like parasite control if you see fleas.
Hypothermia in Dogs
Although hypothermia is usually a cold weather problem. Swimming in cold water, or wet and chill due to rainy weather can also cause hypothermia in dogs.
A Guide to Dog Allergy Medications
There are several manifestations of allergies in dogs, including atopic and flea allergy dermatitis, allergic rhinitis and bronchitis, hives, and insect bite hypersensitivity. Symptoms...
Puppy Strangles: Symptoms, Diagnosis and Treatment
Also known as juvenile cellulitis the puppy strangles is a rare condition whose cause is not known. Most dogs are able to make a complete recovery.
Dogs Can Get Bartonella, Too
In both people and dogs, bartonellosis often shows up with cardiac signs while it is asymptomatic in cats.
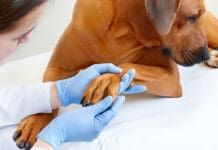
Treatment and Signs of Parasites in Dogs
Parasites in dogs affect both the dogs internal organs like the heart and digestive system, their skin, and orifices like the nose and ears.
Identifying Fungal Infections in Dogs
There are many kinds of fungal infections in dogs, including systemic fungal infections, fungal skin infections, and fungal ear infections.
Babesiosis in Dogs
Babesiosis in dogs is a tickborne disease that attacks red blood cells over time gradually causing anemia. The disease is seen worldwide, and the infection is carried for a lifetime.
Why Your Dog is Licking Their Back Near the Tail
If your dog keeps licking their back near the tail it indicates discomfort due to allergies, fleas, hot spots or other issue to investigate.