[Updated March 26, 2018]
HOSPICE FOR DOGS: OVERVIEW
1. Educate yourself about your dog’s condition to facilitate more productive conversations with your veterinarian.
2. Ask your veterinarian if he is comfortable helping guide you through hospice care or if he can refer you to other options and resources in your area.
3. Focus on your dog’s quality of life; continue to engage him in daily life while keeping him comfortable and pain-free.
4. Take care of yourself! Talk with dog friends, read books, utilize Internet resources, and seek out a pet support counselor or group to help you cope with transitions.
When we first adopt that pudgy puppy, or spring that delinquent adolescent canine out of a shelter, our new dog’s senior years and final days are far from our thoughts. But if we’re lucky enough to enjoy a long life together, eventually, we’ll spend a number of months or years caring for him as a senior dog – and sometimes, a challenging and emotionally difficult time seeing him through to a peaceful death.
Fortunately, there are many resources available to help us support our beloved canine companions – even those who have been diagnosed with chronic or terminal illness – in maintaining the best possible quality of life before they die.

Hospice care, or “pawspice,” the term coined by Alice Villalobos, DVM, former President of the American Association of Human Animal Bond Veterinarians (AAHABV) and founding member of the Veterinary Cancer Society, is supportive assistance in evaluating and managing our pets’ quality of life as they near the end of their days, a time period that can span from days to months.
“In-home ‘pawspice’ care is a wonderful next step,” says Dr. Villalobos, who has a practice in Hermosa Beach, California. “It should be introduced as an interval between the thought and the final act of euthanasia, if the owner really feels that their pet still has a quality of life.”
Another veterinarian, Nancy Kay, DVM, DACVIM, of Rohnert Park, California, and author of Speaking for Spot: Be the Advocate Your Dog Needs to Live a Happy, Healthy, Longer Life, commonly recommends hospice when clients simply want a bit more time for closure with their terminally or chronically ill pet. “They recognize the disease is not treatable (or they have chosen not to treat), but their dog or cat continues to have enough of a ‘sparkle in their eyes’ suggesting that it is not quite time to proceed with euthanasia.” Occasionally Dr. Kay has a client who, for moral, philosophical, or religious reasons, is opposed to euthanasia. She offers hospice as an option, but qualifies this decision.
“If I am concerned that a patient is suffering and we don’t have the means to either make the animal well or euthanize, I make sure that a medical professional is keeping close tabs on the patient and appropriate medications and supportive care are being administered to keep the patient as comfortable as possible. Once someone opts for hospice care at home, I try to connect them with a house call practitioner – someone who can then keep tabs on how the patient is within their home environment and administer appropriate medications.”
Pet hospice programs range from those in which clients are given guidance by veterinarians for managing their pets at home, to more formal programs such as that offered by Colorado State University’s Argus Institute, which goes so far as to offer in-home hospice care by trained veterinary staff and volunteers. For purposes of this article, we use the term “hospice” to describe veterinary end of life care for our pets who are chronically or terminally ill, and whose passing comes either unassisted or via euthanasia. The terms “natural” and “unassisted” death are used in the context of an animal dying on its own time, while under care.
Hospice for Dogs
As Cathy and Jim Maher of Dahlonega, Georgia, were dealing with the challenges of kidney and heart disease in their 14½-year-old Lhasa Apso-mix, Dakota, he began to develop additional medical issues. He was diagnosed with hypothyroidism. Three months after that, Dakota suffered a scary bout of acute pancreatitis, and three months after that, he developed pulmonary hypertension, requiring additional medications to help his heart work more efficiently and open vessels and airways in his lungs. In addition to a number of conventional medications and regular appointments with his veterinarian, Susan Wynn, DVM, CVA, CVCH, RH, of Georgia Veterinary Specialists in Atlanta, Dakota received an assortment of complementary treatments, including frequent acupuncture, monthly chiropractic adjustments, and massage and acupressure at home.
A year and a half after Dakota’s initial diagnosis, Cathy recognized that the little dog had entered a new phase of failing health. With a heavy heart, she and Jim made the mental adjustment from trying to “cure” Dakota to providing hospice care. Their team of veterinarians continued to work on providing the right combination of treatments to ensure Dakota’s quality of life.
Most important to the Mahers was that Dakota, a retired long-time therapy dog, was comfortable. They also focused, more than ever before, on cherishing and documenting the memories, particularly the good ones, that they had with him. Under the guidance of their veterinary team, they administered medications, supplements, and fluids at home, sometimes prioritizing them when it became difficult to administer all of the recommended medications.
“We took walks every evening, just not as far as we used to,” says Cathy. “When he was tired, we carried him. When he had to urinate more frequently because he was receiving fluids subcutaneously twice daily (which we administered at home), we outfitted him with diapers so that he could be more confident and comfortable. But the most important part was taking time to just sit in the sun together, take naps – I spent a lot of time sleeping on the floor with him! – and just enjoying each moment. I took time off when I needed to be at home. It also meant preserving memories and having family photos made with him.”
If you’ve just been handed a big dose of reality and learned that your senior dog has a chronic or terminal illness and perhaps six months or less to live, you might ask now what? According to Dr. Wynn, founder of the newly formed dog hospice program at Georgia Veterinary Specialists, the journey begins with first having the best possible understanding of your pet’s condition.
Do as much research as you can about your dog’s condition, gathering information from the best sources you can. Some of Dr. Wynn’s favorite resources include VeterinaryPartner.com, particularly for their great drug monographs; American Animal Hospital Association’s (AAHA) pet care articles, FAQs, and practice guidelines; and Morris Animal Foundation’s Resources for Pet Owners with Cancer Patients.
“Once you comprehend your pet’s illness and the goals of his treatment plan, you will be able to have a better conversation with your veterinarian,” says Dr. Wynn. “In hospice, patients generally have chronic or terminal conditions, but the goal is to manage the disease as well as possible to increase quality of life. The primary objective of palliative care is relief from pain or discomfort and emotional support for the owner.”
Utilizing the team approach common to human hospice care, emotional support is more typically available from outside sources – ideally recommended by the veterinarian, rather than being provided directly by the veterinarian. Inspired by a presentation given by Dr. Villalobos, Dr. Wynn shares with her own clients information gleaned from Villalobos’ work and provides us the following as critical issues that need to be addressed when our senior dogs reach the hospice stage of their lives:

Jim Maher
Critical Factors of End of Life Care for Dogs in Hospice:
1. Recognizing When Our Dog is in Pain
We, as pet owners and even veterinarians, are terrible at recognizing pain in our dogs, yet pain management is critical to quality of life. “Pain can be very detrimental to a pet,” says James Gaynor, DVM, MS, and author of Handbook of Veterinary Pain Management. “Physiologically, pain can be so detrimental that it can decrease healing and can actually cause problems with other organ systems.” But, he points out, it’s natural for dogs to hide pain. He cites research performed by investigators at the North Carolina State University College of Veterinary Medicine in which dogs were videoed for 24 hours continuously after routine spay surgery. Throughout the monitoring period, researchers would enter the kennel and interact with the dogs. During the time of interaction, the dogs would hide their pain, greeting the researchers at the cage door and wagging their tails. When the researchers left the dogs alone, they were restless and showed signs of discomfort.
Although a physical exam and radiographs can help a veterinarian detect pain (or potentially painful conditions), owners would be wise to look for subtle changes in their dogs – often the most significant indicator of a problem, and one that needs to be communicated to the dog’s veterinarian. If your dog is lethargic, reluctant to rise or walk, grumpy, or displays other behavioral changes, you should suspect that he’s in pain.
Dr. Kay adds, “I am the first to admit that reading pain can be extremely difficult in dogs and cats. Scientifically speaking, blood pressure measurements seem to be the most reliable indicator of pain status (blood pressure increases when pain is present). Needless to say, continuous blood pressure monitoring isn’t feasible outside of the hospital environment. Animals are so variable in terms of how they outwardly manifest pain. Many people expect to hear whimpering or whining. My sense is that only the minority of dogs and cats vocalize when in pain. Inappetence and reclusive behavior are likely more reliable outward indicators.”
At home, the most objective measure we can use is the dog’s pulse and respiration, and before a crisis strikes is a good time to get a baseline, says Dr. Wynn. An increase in either pulse or respiration can be an indicator of pain.
What’s normal? For small dogs and medium dogs, 70 to 100 beats per minute (bpm), and 60 to 90 bpm for large/giant dogs. Your dog’s pulse should be easily palpated, strong, and regular, and a relaxed dog might have a slower pulse. Normal respiration for dogs is 10 to 30 breaths per minute. Ask your veterinarian to show you how to read both on your dog.
2. Managing a Dog’s Pain
Dr. Wynn reports that, “In practice, veterinarians now tend to give the animal the benefit of the doubt, and administer analgesics if there is any possibility of pain. An improvement in behavior or activity proves the principle.”
Pain can be managed with both conventional and complementary methods. Anti-inflammatory drugs (Rimadyl, Deramaxx, Metacam, Previcoxx, Etogesic) and analgesic drugs (tramadol, buprenorphine, and others) most likely will be necessary to keep the hospice patient comfortable. Anti-inflammatory and analgesic herbs can be used in concert with prescription pain medications, as can acupuncture, which has been shown to release serotonin.
Dr. Wynn also recommends massage, saying, “We should all be thinking about using massage a lot more; it is known to help relieve pain and depression. In humans, it is one of the most proven effective alternative therapies in cancer patients to relieve pain, nausea, and especially fatigue.” Find a massage therapist who is trained and certified (Certified Massage Therapist or CMT) in massage for dogs.
3. Keeping the Dog Hydrated
In human medicine, dehydration is suspected to increase sensitivity to pain. Dehydration can cause discomfort in the canine hospice patient, too; he might feel sluggish, lose his appetite, and experience constipation. Humans can suffer from headaches when dehydrated, and some vets speculate that this is possible in dogs, as well. When an individual is close to death, however, one must observe the dog closely to determine whether fluid administration seems to brighten the dog’s demeanor or make him feel worse; for example, fluid administration in dogs with certain conditions can cause edema, which can induce breathing difficulties.
A well-hydrated dog’s skin should snap back immediately; if it takes two or three seconds, typically you’re seeing dehydration. Note that older dogs typically have some loss of skin elasticity, so this test can be variable depending on the dog. You might also find that your dog has dryer, tackier mucous membranes, to the point that when you open your dog’s mouth, the saliva will be sticky; normally, the mouth and gums should be wet.
You can hydrate your dog orally and subcutaneously, but trying to use a syringe to do so is typically a tough job: An average dog requires approximately 60 milliliters (2 ounces) of water per kilogram of body weight per day just to maintain normal function. In a dog experiencing increased water loss due to frequent urination, vomiting, or diarrhea, you’ve got an even bigger job. It’s important for you to learn, from your dog’s veterinarian, the maintenance amount that you need to administer to keep your dog hydrated. Subcutaneous fluid administration is easy to do; your veterinarian can teach you how to give fluids at home.
4. Happiness/Responsiveness to the Dog’s Environment
What gives your pet joy? Happiness and responsiveness to his environment are both big parts of quality of life. Dogs can get “down,” especially in periods of change. If our dogs can’t do many of the things they used to enjoy, why wouldn’t they become depressed?
At a minimum, Dr. Wynn says, we know that dogs experience boredom. “Dogs are intelligent animals. It’s important to think of ways to get them engaged in their environment. For example, obedience dogs and other dogs who have had ‘jobs,’ are used to thinking through problems and being rewarded; it’s important to get creative and think of other problems for them to solve. Like putting kibble under a cup, and letting them find the right cup.” For the dog who has been accustomed to grooming, bring out the brushes. If your dog has always enjoyed going for rides in the car, that’s a great way to get her out, and to help her to engage with her environment.

Lisa Rodier
“We know for sure that anxiety occurs in dogs,” Dr. Wynn adds. “If your dog is confined to an area like a crate or a bed, move the bed closer to where the family spends time. Dogs are smart, and they certainly know if their environment has changed, or worse, if the attitude of their caregivers has changed. Your dog has been losing senses of sight, hearing, smell, and now you’re away from them? You need to be proactive about preventing that.”
5. Your Dog’s Mobility
Keeping your hospice patient mobile increases her circulation. It’s also critical to minimizing anxiety and problems with hygiene by helping the dog to maintain her normal elimination habits. Getting your dog up also keeps her engaged in her environment and reduces the incidence of pressure sores.
It’s our job to keep our pets moving, particularly if they can’t do so on their own. Early on, in the stages when the dog can still walk, ramps are useful for maintaining a level of independence, and body harnesses allow for a little extra assistance when needed. In later stages when the dog has more trouble getting around, consider rear end slings, whole body slings, and properly fitted carts.
6. Dog’s Hygiene and Grooming
Maintaining your dog’s grooming routine and keeping her clean is critical to her well being. If the dog is incontinent, she can easily get urine and feces on her skin, making her more prone to infection, so use diapers and special beds to manage that issue. Keep the dog comfortable by keeping her hair groomed, clipped, and free of mats.
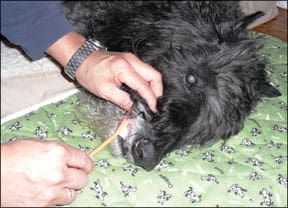
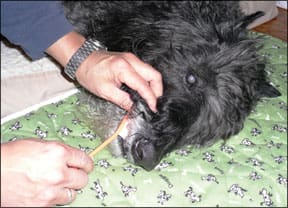
Don’t neglect her eyes, nose, and mouth; wipe with a damp cloth, squirt water in her mouth, and even brush her teeth. Dr. Villalobos favors the comforting “mother tongue technique,” in which the dog is wiped with a warm damp cloth, using long strokes to mimic the grooming of a mother dog.
7. Nutrition of Dog in Hospice
For many pet owners, this is a very emotional topic; we tend to get upset when our dogs won’t eat! Dr. Wynn explains, “Our main goal is to identify treatable reasons that the pet is not eating, such as pain or nausea. While nutrition is a concern for hospice patients, we must realize sick animals may no longer feel hunger, and since the body is unable to store nutrients for future use anyway, force feeding would lead to deterioration in quality of life.”
This explains why a feeding tube is often not recommended; the primary purpose to use one is to more easily administer medication. “We don’t want them to starve,” she says, “but we don’t want to force food on them. What we can do is tempt them. Warm their food so they can smell it better – aging pets have diminished senses of smell and taste – and present small amounts of novel and smelly foods, such as baby food, cheddar cheese soup, pizza, Alfredo pasta, fast food hamburgers, bacon, braunschweiger, or add a drop of smoked flavoring to other foods.”
Appetite stimulants such as mirtazapine and prednisone can be used, although Dr. Wynn particularly likes to utilize acupuncture because it is an anti-depressant, good for pain, releases serotonin, and can quell nausea. It’s also recommended that you identify the daily caloric goal for your dog (about 100-130 kcal/pound of bodyweight per day), and compare it to the amount the dog consumes to better regulate food intake and know whether your dog is taking in enough calories.
Your Dog’s Quality of Life During Hospice Care
Ask anyone, “What is quality of life?” and you’re certain to engage in a lively philosophical discussion. While researching this article, I came upon a definition that made lots of sense to me, particularly because it was discussed in the context of hospice care for pets. (The book is Geriatrics and Gerontology of the Dog and Cat, a veterinary textbook; the quote was from “Owner Services and Hospice Care,” a chapter written by veterinarians Guy Hancock, Franklin D. McMillan, and Tina R. Ellenbogen.) Quality of life, the authors contend, is driven by feelings. “Feelings appear to play such a central role in quality of life that feeling states can be regarded as the single common denominator for all factors that influence quality of life . . . . Any factor that does not have an influence on feelings is not a factor in quality of life.”
Feelings contribute pleasantness or unpleasantness on a continual basis and can be of emotional or physical origin. Physically unpleasant feelings include weakness, nausea, pain, pruritus, hypoxia, thirst, hunger, constipation, and temperature extremes, while physically pleasant feelings come from physical contact and gustatory (taste) pleasures. Emotionally unpleasant feelings include fear, anxiety, boredom, frustration, loneliness, separation distress, depression, hopelessness, and helplessness; emotionally pleasant feelings are evoked by social companionship, play, and mental stimulation.
The authors use removal of a lipoma, a toe amputation, or loss of hearing in one ear as examples of factors that are unlikely to affect the dog’s feelings and therefore his quality of life. In contrast, factors that would induce negative feelings include osteoarthritis, glaucoma, and social deprivation.
“A pet does not need to be in pain in order to be suffering,” comments Dr. Kay. “I suggest that an owner thinks about how she feels when she has a bad case of the flu; she may not be in pain, but she may certainly suffer!”
Quality of life is a balance between pleasant and unpleasant feelings, and one way to think of quality of life is via a scale with pleasant feelings on one side and unpleasant on the other; the goal for our pets is to achieve a balance. But if even a single unpleasant feeling is strong enough, it can tip the scale and alone make quality of life very low.
Various quality of life scales are becoming increasingly utilized in veterinary hospice care. As you begin the journey with your pet, ask your vet whether she has a quality of life scale that the two of you can utilize to more objectively assess changes in your dog’s condition.
Dr. Villalobos utilizes a scale called “HHHHHMM” (Hurt, Hunger, Hydration, Hygiene, Happiness, Mobility, More Good Days than Bad Days). Patients are scored in each category on a scale of 0-10, with 10 being best. In general, a total score of 35 or higher is indicative of a continuing “good” hospice experience but use your dog’s veterinarian as a sounding board. It’s important to have an ongoing dialog with your her about what you’re seeing, so don’t try to go it alone.
Lisa Rodier
Knowing When It’s Time
In some cases, owners use hospice care for their pets in the same way that it’s used in human medicine: to maintain the patient until her natural death. Others use hospice until they feel that allowing the animal to continue to die at his own pace is cruel, and they have the patient humanely euthanized.
According to Dr. Wynn, “End of life changes signal that it’s time to consider whether we will choose euthanasia or for our pet to die at home. Changes can include starvation due to prolonged anorexia, changes in behavior, decreased urine production, changes in breathing, temperature changes, loss of bowel or bladder control, lung congestion, restlessness, confusion, and decreased responsiveness.” When the signs indicate that our pet is in a transition stage, she recommends that we shift our focus from quality of life, to quality of death. We need to ask ourselves the following difficult, but necessary, questions:
– What would a quality death be like?
– How would I prefer to say goodbye: during an episode of suffering or a calm doze?
– When I look back, what would be important to me about how my pet’s death was handled?
– What is the worst thing that could happen regarding my pet’s death?
Most of us yearn for a peaceful death for our pets, typically one that involves them passing away in their sleep. Unfortunately, this is not very common.
Dr. Kay says, “Certainly most of my colleagues would guess that more than 90 percent of pet caregivers will need to make the decision to euthanize their pets. When someone tells me their pet passed away on its own, I let them know how incredibly lucky they are. Hospice care, in my experience, does not always translate into death by natural causes. Most of the time it is implemented to maintain comfort until it is clear to the decision makers that euthanasia is indicated. In my mind, end-of-life care is all inclusive. Hospice until death occurs naturally is just one version of end-of-life care, as is hospice until the family opts for euthanasia.”
Dr. Wynn gently reminds us that dying is part of the experience of owning a senior pet. She suggests we consider the following: Will euthanasia be easier later than now? Is the proportion of good days to bad days “right”? Will there ever be another day or hour of good quality life that is better than right now? What regrets would you have if euthanasia occurs too soon or too late? What is the bottom line for you: invasiveness or cost?
Holistic veterinarian Ella Bittel, DVM, of Los Alamos, California, supports pet owners who wish to allow their pets to die on their own time (while under care), reserving euthanasia for when the animal’s pain or comfort level cannot be managed by the “best care that we can provide.” Pet caregivers who strive for this type of death for their animals, she says, optimally would follow the hospice model of care (palliative and comfort care sufficient to keep the dying and their family comfortable) and ideally have 24/7 access to a veterinary professional should a crisis arise.
Dr. Bittel qualifies this by saying that we need to be aware that there can be situations when euthanasia is warranted, despite our wishes, given the animal’s condition. She believes that many veterinarians lack education about hospice, and as a result, sometimes advise their clients to choose euthanasia too quickly.
“Because hospice care is not yet a part of the curriculum in veterinary schools, many veterinarians lack information about what true hospice care entails, are uncomfortable supporting owners seeking hospice for their animal, and often think that the dying process as it unfolds without euthanasia equals unbearable suffering,” she says. Dr. Bittel also takes issue with the use of the term “hospice” when describing end-of-life care services for our pets that culminate in death via euthanasia close to 100 percent of the time, maintaining that the term hospice comes from the human hospice model that supports individuals in dying peacefully in their own time.
Whose Decision Is It?
While it would be so much easier to allow someone else to make the heart-wrenching decision to euthanize our pets, it’s almost always in our best interest to decide ourselves. While Dr. Kay will guide a client through the decision-making process, she says it must be the client who makes the final call. “If I believe a situation is hopeless, I will tell her. I make sure she is staying ‘real’ rather than floating on the river in Egypt (denial). But I always want the decision to be the client’s, not mine. The very best way to ensure the client’s long-term peace of mind is when she has made the end-of-life decision for her pet.”
Dr. Kay hosts a support group for grieving owners at her practice, and observes, “Those who end up stuck in various stages of guilt (some have been in the support group I facilitate for more than a year) tend to be people who feel that the decision-making was taken out of their hands – a relative made the decision or an intimidating veterinarian said, ‘You should…’ I coach people who are reluctant to euthanize by acknowledging their desire to avoid making the decision too soon. I then let them know how some people experience long-term suffering when they recognize they’ve waited too long.”
I asked Cathy Maher, who was extremely bonded to Dakota, how she knew that it was time to say good-bye to him. With tears in her eyes she recalls, “Dakota refused all food beginning on a Thursday in June 2009. His last meal was homemade pizza (approved by Dr. Wynn) the night before. I came home during lunch on that Thursday, and he was walking around, but still refused food. That evening, he continued to refuse food and spent a majority of time lying in his bed or in my arms. He had difficulty drinking from his water bowl, so I gave him water through a syringe. We made an appointment to see his internist, Todd Green, DVM, the next morning so that he could assess Dakota.
“When we saw Dr. Green, we asked that he administer pain management medication, and we took Dakota home. It was our intention to allow Dakota to pass peacefully at home in his bed, and we planned for euthanasia as a back-up if Dakota was in pain and distress.
“However, within an hour, Dakota began to whimper and cry. I knew in my heart that he was actively dying and in distress, and continuing to support a natural death was no longer an option to us. We lived within 10 minutes of the veterinary hospital, so we called to let them know we were returning. On the way, Dakota’s eyes became glassy and distant and his cries and screams intensified. Dr. Green met us on the back porch of the clinic and Dakota was euthanized under a tree in the nature preserve.”
Although it’s still difficult today (think waterworks!) for Cathy and me to discuss this, she is confident that Dakota’s hospice journey, despite it being overwhelming at times, was a good one, and the right decision for their family. She is also quick to point out that the role of your dog’s veterinarian in the success of your plan cannot be underestimated. Dakota’s veterinarians, particularly Dr. Wynn, were an integral part of helping them to help Dakota enjoy the rest of his life.
“Dr. Wynn’s will to help him be comfortable and his will to live were amazing,” says Cathy. Dakota Maher passed away on June 12, 2009. Because of the Mahers’ journey with Dakota, Cathy was inspired to create “Pawprints,” a pet caregiver support network, whose mission will be to honor the human-animal bond by providing compassionate support, resources, information, and educational opportunities to individuals and families caring for their aging, chronically or terminally ill companion animals.
“Anticipatory Grief” During End of Life Care for Dogs
A term that I encountered while researching this altogether was “anticipatory grief.” For an explanation of the term, particularly in relationship to pets, I queried Sandra B. Barker, Ph.D., NCC, LPC, who is a professor of psychiatry and director for the Center for Human-Animal Interaction at the VCU – Medical Campus, and also founded the pet support hotline at the Virginia-Maryland Regional College of Veterinary Medicine. She describes anticipatory grief as a normal process for individuals facing the death of a person or pet.
“Anticipatory grief occurs when pet owners begin grieving for a pet who is still living, but often terminally ill or declining in health such as occurs with older pets. Owners may experience sadness, loneliness, and other symptoms of grief as they think about life without their pet.
“In my experience working with pet owners, anticipatory grief has been helpful for pet owners, in that it begins to prepare them for the death of their pets and often helps them accept the loss with less difficulty after the actual death. Some owners will consider what they want to do for their pet now, knowng that they won’t be around for much longer. It might be a last trip to the beach, special treats, or a celebration of the pet with those who loved the pet. Owners may also begin to consider how they want to treat their pet’s remains after death, how they want to commemorate their pets, or whether to obtain another pet. These types of anticipatory expressions are generally helpful for the owner.”
Drs. Barker and Kay both recommend that joining a pet support group prior to your pet’s death can be helpful. Dr. Kay facilitates a group at her clinic that is open to the community and is comprised equally with individuals who have lost a pet and those with pets who are terminally ill.
Lisa Rodier lives in Alpharetta, Georgia, with her husband and two Bouviers, and volunteers with the American Bouvier Rescue League.