This procedure will require general anesthesia.” There are few statements that a veterinarian can make to a dog owner that causes more alarm and misgiving, sometimes greater than the anticipated procedure itself. Throughout the years, companion animal guardians have come to suspect that general anesthesia presents a threat to all but the most robust animals, and should be avoided if at all possible.
However, modern advances in all phases of veterinary medicine, including anesthesia, enable today’s veterinarians to significantly improve the length and quality of our companion animals’ lives, and perform lifesaving and life-enhancing treatments previously considered too risky or too complicated.
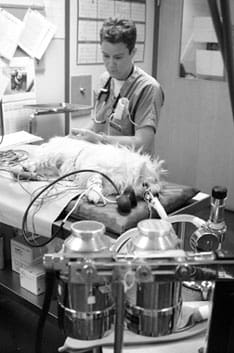
As in human medicine, however, veterinary healthcare consumers must choose from a variety of options for the surgical care of their dogs. Understanding the issues surrounding the use of anesthesia, the needs of their particular dogs, and the complementary or holistic care practices that can support an animal undergoing anesthesia will enable companion dog owners to provide the best possible guardianship of their animals.
Types of anesthesia
The definition of anesthesia is “without pain,” and anesthetic agents enable veterinarians to perform medical procedures on animals safely and humanely.
Local anesthetics, such as an injection of lidocaine to perform a skin biopsy, provide for the short-term “deadening” of a small site on a patient that remains fully conscious. Regional anesthesia requires the injection of the anesthetic into the nerves or around the spinal cord to cut off the sensation of pain from the surgical site. Regional anesthesia blocks only pain impulses from the part of the body being anesthetized. The patient is fully conscious and her vital signs normally remain unaffected.
Although extremely safe, local and regional anesthesia do have their drawbacks. Mostly useful in treating minor problems of the skin, the dog is awake and can struggle during the procedure. Physical restraints may further excite an already agitated dog, and complications arising during surgery may be difficult for the doctor to control or treat.
General anesthesia produces a state of complete unconsciousness and the total loss of feeling in the entire body during its administration, and for a time thereafter. Although general anesthesia does carry some risk of serious, adverse reactions, it has revolutionized the safety, quality, and range of surgical treatments offered to dog owners.
General anesthesia
The process of administering general anesthesia in anticipation of a surgical procedure includes several distinct phases or steps:
Preparation and premedication, when the doctor evaluates and treats the dog prior to the surgical procedure, and the owner prepares the dog for the surgery.
Induction, when the veterinarian administers a general anesthetic and takes the dog to a level of unconsciousness suitable for the surgical procedure.
Maintenance, when the veterinarian or the anesthesia technician maintains the dog in a state of unconsciousness, and the doctor completes the surgical procedure.
Recovery, when the dog returns to consciousness, begins to heal from the procedure, and eventually resumes normal activity levels.
Let’s discuss the elements of each of these phases of the process of administering general anesthesia, and discuss the options available for the care of your dog.
Preparation, premedication: Countdown to surgery
Suspend the use of all herbs at least 48 hours before the surgery, and advise your veterinarian if you use these remedies. Some herbs may thin the blood or interfere with the proper administration of anesthesia.
Prior to administering an anesthetic and performing an elective surgical procedure, a veterinarian will examine your dog completely to determine if she is in general good health. Usually, the veterinarian will draw blood before the day of surgery, especially if the patient is an older dog, or one whose health is compromised by injury or illness. The doctor will check the blood count for signs of anemia or a high white blood cell count that may indicate the dog has an infection.
A blood chemistry profile indicates to the doctor if the dog’s kidney and liver functions are normal. These tests are particularly important for dogs seven years or older, dogs with a recent history of kidney infection or other illness, and young dogs with congenital defects, such as a heart murmur. The veterinarian will refer to these test results before selecting the anesthesia protocol for your particular dog.
Although many veterinarians do not insist on performing a preoperative blood test for young, apparently healthy dogs, it’s worth the investment (about $70) to screen closely for any indications of hidden health concerns before scheduling surgery.
Follow your veterinarian’s instructions about giving food and water to your dog at home, before and on the day of surgery. Most doctors require owners to make food and water unavailable to the dog at least 12 hours before the surgical procedure. An empty stomach will prevent vomiting if the anesthesia makes the dog nauseous.
If your dog is particularly anxious at the veterinarian’s office, or suffers from separation anxiety, ask your vet whether you can bring the dog to the hospital just prior to the scheduled surgery, to reduce any time she may have to spend caged in a holding area before surgery. Although most veterinary hospitals have “drop-off” times early in the morning, even for dogs whose surgeries are scheduled for hours later, your good relationship with your caring veterinarian should encourage the doctor to permit you to bring your dog to the hospital just before the procedure, and to accompany her up to the time of surgery.
Some veterinarians may give the dog a mild sedative to relax the dog before the procedure. A particularly anxious dog may benefit from receiving a mild tranquilizer while you are still with him, before he has a chance to get “worked up” in your absence.
A tranquilizer called acepromazine is commonly given to dogs prior to anesthesia induction. “Ace” (as it is commonly known) should not be given to epileptics or other dogs who are susceptible to seizures, as it can lower the seizure threshold and cause seizure activity. Make sure you let your veterinarian know if your dog has ever had seizures so he can avoid using this drug.
The doctor may clip a patch of hair on the dog’s leg and insert an intravenous (IV) catheter, which will administer intravenous fluids to support the animal during surgery. Especially beneficial for older dogs, IV fluids help keep the dog’s blood volume and blood pressure stable. Fluids also help the dog replace lost blood quickly, and assist in flushing toxins from the dog’s system.
Induction
The act of creating a state of unconsciousness, muscle relaxation, and analgesia (freedom from pain) through the administration of a general anesthesia is called induction. Most commonly, veterinarians use a quick-acting, injectable anesthetic drug to swiftly “knock out” the dog before moving on to the next phase of anesthesia, which is maintenance.
Sometimes, injectable anesthetics are used as a sole agent to induce a short period of restraint for minor, non-painful procedures, such as radiology and ultrasound examinations, but in surgery, the injectable agents are most often used to quickly bring the animal to the “surgical plane” of unconsciousness, after which inhalant (gas) anesthetics are used to maintain anesthesia.
Once an injectable anesthesia enters the dog’s body, it remains in the fatty tissue until the liver metabolizes it, or the dog receives a reversal agent. Not all injectable anesthetics have reversal agents and, in the case of an overdose, the doctor can only provide supportive care until the agent leaves the dog’s system, usually in 40 – 60 minutes.
Some dog owners and veterinarians have concerns about using the combination of injectable and inhalant anesthetics in certain breeds. Brachycephalic (flat-faced) breeds such as Pugs, Bulldogs, Boston Terriers, and Shih Tzus are reportedly prone to complications such as respiratory depression when subjected to the anesthetic combination.
Greyhounds and other sighthounds (Whippets, Afghans, Salukis, Borzois, Wolfhounds, Deerhounds) sometimes exhibit a delayed drug metabolism, with prolonged anesthesia resulting from a combination of anesthesia drugs. Some have attributed this to a low percentage of body fat (where anesthetic drugs are stored before being processed and excreted by the liver and kidneys); other speculate that these dogs lack the oxidative enzymes in the liver that are needed to metabolize the drugs normally.
Guardians of these dogs sometimes ask their veterinarians to forego the use of the injectable drug, and “gas down” their dogs with inhalant anesthetic alone. This practice is controversial, however. Many animals panic when an inhalant anesthetic is used to induce unconsciousness, since a mask must be placed over their faces and the anesthetic they breathe may concern them. Struggling during gas induction raises the heart rate of the dog and causes the animal unnecessary discomfort. Also, escaped gas from mask inductions is wasteful and may be dangerous to the hospital personnel attending the dog, so many veterinary practices avoid this type of induction.
Again, communication with your veterinarian is key. Talk to her about your concerns, and ask about her anesthesia protocol for the type of dog you have. If you feel your concerns are being brushed off without full consideration or explanation, find another veterinarian to work with.
Propofol is the newest injectable anesthetic, used in human medicine and introduced into veterinary practice in 1987. For induction purposes, Propofol works rapidly and the dog slips into unconsciousness quietly and with little excitement. The drug is metabolized quickly by the dog’s body, and offers a short, smooth, and high-quality recovery. Many practices use this agent for outpatient surgeries. However, propofol is short-acting and difficult to adjust when used for hours at a time, so it is not appropriate for lengthy procedures.
Older types of injectable agents, such as ketamine, are less expensive, but may cause some spontaneous muscle activity upon induction and dogs tend to experience a rougher recovery period. Ketamine is usually mixed with diazepam (Valium) or another sedative or tranquilizer to control these effects.
After inducing the animal, the veterinarian places a tube through the dog’s mouth and into the trachea (windpipe). The doctor then connects the tube to a machine that delivers an inhalant anesthesthetic for the maintenance portion of the process; then he prepares the surgical site.
Maintenance
Sevoflurane is the latest inhalant anesthetic available for use in veterinary medicine. Isoflurane and, to some extent, halothane are most widely used. More expensive than the older agents, sevoflurane is noted for creating a speedy induction and recovery, and its relatively pleasant odor. However, due to the preference for IV inductions, the speed of induction with sevoflurane is not clinically important.
The anesthetist can titrate (adjust the strength) of gas anesthetics much easier than injectables, so it’s easier to manage the dog’s unconscious state using this method.
Dogs should be kept warm during surgery, especially extended procedures. Many clinics place their patients on special pads that contain circulating warm water to keep them from getting chilled. At a minimum, the dog should be covered with warm towels or blankets for a long surgery.
One of the most important factors in the maintenance phase of general anesthesia is the monitoring of the patient, both by the presence of an anesthetist and the utilization of various pieces of operating room equipment.
An anesthesia technician should watch the dog during surgery, looking for good, pink color in the dog’s gums and skin, and take the dog’s blood pressure periodically to check for proper circulation of the blood. Most doctors rely on a non-invasive pulse oximeter, which measures the oxygen saturation in the dog’s arterial blood. An electrocardiogram (EKG) monitors the electrical activity in the dog’s heart and indicates if the animal’s heart beats too quickly or too slowly or develops arrhythmias. An audible apnea (suspension of respiration) alarm may be used, but some consider it unreliable and inaccurate.
Ventilation equipment is often used during extended surgical procedures. Under anesthesia, animals do not breathe as deeply, nor do they fill their lungs and “sigh” as regularly as they do when they are awake. In effect, their lungs collapse slightly under general anesthesia. By occasionally squeezing the breathing bag attached to the ventilation equipment for the animal, the anesthetist can periodically fill the animal’s lungs, keeping them healthy and the dog’s blood properly oxygenated.
The services of a veterinary technician or anesthetic nurse and the utilization of monitoring equipment all add cost to the surgical procedure. However, they significantly contribute to the safety of your dog while under general anesthesia.
Lore Haug, DVM, and a member of the Department of Small Animal Medicine and Surgery at Texas A&M’s College of Veterinary Medicine, states that the minimum monitoring support she would personally require for one of her own animals about to undergo surgery is the presence of an anesthesia technician to watch and ventilate the animal, a pulse oximeter, and an EKG machine. She adds that the more ill an animal is at the time of surgery, the more different types of monitoring it will require during the procedure.
Inhalant anesthetics also provide analgesia, or pain relief. Pain is a sensory and emotional response to the stimuli that results from damage to bodily tissue. As a result of mechanically manipulating the tissue and organs, as in a surgical procedure, or by enduring thermal or chemical damage, the body reacts with the sensation of pain.
The American College of Veterinary Anesthesiologists’ position paper on the treatment of pain in animals suggests that the need for adequate pain relief is more compelling now than ever before, as modern anesthetic practices provide for rapid recoveries after surgery. Most surgical practices provide for initial postoperative pain relief through the administration of inhalant agents administered during surgery.
Recovery
The dedicated care of a veterinary professional to manage the dog’s recovery from general anesthesia until the end of the anesthetic period is as important as the surgical skill of the operating veterinarian. Some anesthetic agents take more time to clear from a dog’s system, and a recovering dog may show signs of lethargy, loss of appetite, or diarrhea. A dog must be monitored carefully and kept warm and hydrated for a prompt, smooth recovery.
Assuming the absence of complications during surgery, arrange to visit your dog as soon as possible after surgery; bring him home as soon as possible when cleared to do so. Your presence will calm your dog and reduce his stress and discomfort.
Some veterinarians apply a fentanyl patch to the dog’s chest to deliver pain medication through the dog’s skin and directly into his blood stream. Consult with your veterinarian about pain relief medications that may be needed during recovery at home.
Adjuncts to conventional care
Perhaps the most valuable aspect of holistic medicine is as a support for the animal’s life force or spirit during a health crisis. Many complementary care methods have an “energy medicine” component that can boost a compromised animal’s healing response. These include acupuncture and acupressure, Reiki, homeopathy, flower essence therapy, and aromatherapy, as well as herbal medicine.
Many holistic practitioners have a protocol for dealing with the psychic and physical effects of anesthesia.
Deborah Mallu, DVM, a holistic veterinarian in Sedona, Arizona, focuses on the psychic effects. Dr. Mallu reminds her clients that the external world is a reflection of the mind. Therefore, she favorably affects a dog’s external, or bodily, world by bringing peace to his inner world. She creates a positive, supportive space in her operating room by playing relaxing or spiritual music during the procedure, and engaging in only positive conversations, focused on the patient.
Dr. Mallu also assumes that the dog retains some level of consciousness even during general anesthesia, and speaks positively about the outcome of the procedure and the health of the dog at all times. She visualizes herself on her patient’s team, working with the dog to improve his health, rather than as a repairman attacking the dog’s body.
Dr. Mallu encourages her clients to visualize and explain to the animal what’s going to happen during the procedure. Rather than comforting the animal by describing what will not happen (“Don’t worry, it won’t hurt for long, you aren’t going away forever . . . ”) she suggests telling the animal what will happen (“You’ll be in the hospital for a short time, relaxed and pain-free during surgery, and home again before long. We can help you to feel only a little pain after the procedure.”). This approach short-circuits fear-based thinking and creates positive and emotionally stable interactions with your dog.
She keeps a flower essence remedy known as Rescue Remedy available for herself, her clients, her patients, and her staff members to settle the mind. During surgery, she may ask her technician to administer a homeopathic remedy to her patient, such as phosphorous to decrease bleeding and to help alleviate the effects of anesthesia following the procedure. Dr. Mallu may give aconite or arsenicum album to a very fearful animal.
The occasional use of single remedies, as described by Dr. Mallu, is not in keeping with the tenets of classical homeopathy, where remedies are selected based upon a comprehensive understanding of the entire animal. However, Dr. Mallu considers the above-mentioned remedies broadly functional for such as wide range of conditions that their use is occasionally warranted under her supervision. She does not administer these remedies if the animal is already under the care of a classical homeopath.
Dr. Mallu may administer acupuncture while the dog is asleep to control pain, bloating, and nausea following the procedure. She also strongly emphasizes the importance of “gentle tissue handling” during surgery, and minimizes postoperative pain by being particularly mindful that much of that pain results from the harsh handling of the dog’s tissues and internal organs. Dr. Mallu always closes with absorbable, subcuticular (under the skin) closures to maximize comfort at the incision site and discourage the dog from licking or biting at the sutures. In more than 20 years of veterinary surgery, Dr. Mallu has never used an Elizabethan collar to prevent a dog from biting at his incision, and makes minimal use of analgesics after surgery. She has a small cottage adjacent to her surgical suite in which the dog’s guardian can hold the animal, wrapped in a blanket, while the dog regains consciousness.
Dr. Mallu rarely uses aromatics to help with recovery after surgery because the dog has already received inhalant anesthesia. However, when indicated, she may fill a half-pint spray bottle with 3 drops of lavender oil, 10 drops of Rescue Remedy, and pure water, and spray the mixture lightly around the dog.
At home, she advises her clients to keep the dog comfortable and their own mind stable to help with the emotional recovery of the animal.
Acupuncture and acupressure
Chris Bessent, DVM, a Milwaukee-based holistic veterinarian, acupuncturist, and herbalist specializing in sports medicine for horses and dogs, concentrates more on the physical aftereffects of anesthesia.
In Dr. Bessent’s opinion, the anesthetic process is not over when a dog regains consciousness after general anesthesia. “Holistic doctors know that the anesthesia process often continues on for weeks after the treatment,” she says.
She explains that many dogs develop a liver qi (pronounced “chee” and understood as the energy or force associated with life and life processes in living beings) stagnation from the effects of general anesthesia. Anesthetics are toxins that the liver must eliminate, with a significant effort.
Dr. Bessent usually treats a dog one to two weeks after it receives general anesthesia. She performs a “pulse diagnosis” by taking the dog’s pulse at 12 positions on the dog’s femoral arteries in the hind limbs. After anesthesia, 90 percent of the dogs she examines have a “superficial” pulse that feels taut, like a wire. A “normal” or “balanced” dog’s pulse is moderate and not too tight.
Dr. Bessent also performs a “tongue diagnosis” and finds that 90 percent of dogs that have recently received anesthesia have a purple to red tongue, indicating a condition of “heat” caused by a liver imbalance. A healthy dog’s tongue is pink.
A few dogs are capable of “righting” themselves completely after anesthesia, but most show mild to significant long-term reactions to the anesthesia process. “Remember,” Dr. Bessent explains, “these reactions are not the direct result of the general anesthesia itself, but the result of the reaction of the dog’s liver to the anesthesia, which can then be treated.”
To correct liver qi stagnation, Dr. Bessent uses acupuncture and combinations of Chinese herbs, including coptis and scutellaria, or, sometimes, long dan xie gan tang. Dr. Bessent may recommend the herbal combination “Great Mender” to help speed healing for traumatized tissue. (Visit Dr. Bessent’s Web site at herbsmithinc.com for more information about herbal remedies.)
Normally, after a single acupuncture treatment and dose of herbs the dog is back to normal, as Dr. Bessent confirms with a follow-up pulse and tongue diagnosis. Older dogs, who are more difficult to “balance” following anesthesia, may require a second course of treatment 10 days to two weeks after the initial treatment.
Dr. Bessent points out that if guardians do not fully resolve the aftereffects of anesthesia on their dogs, a number of conditions may plague the dog afterward, mostly inflammatory in nature and settling into one place in the dog’s system. These conditions include the beginnings of allergies, gastrointestinal upset (vomiting and diarrhea), inflamed eyes, anal sac problems, vaginitis, seizures, and even irritability and aggression.
On occasion, Dr. Bessent will examine a dog before it undergoes anesthesia. She performs a preoperative pulse and tongue diagnosis, and balances the dog, if necessary, with acupuncture. She advises her clients not to administer any herbs to their dogs within 48 hours of surgery.
“General anesthesia is a necessary and safe process,” Dr. Bessent says. “But animals need more supportive care surrounding the event to reduce or eliminate imbalances following treatment.”
Keep in mind
Modern general anesthesia provides the veterinarian with one of her most useful health care tools. Guardians can embrace anesthesia as an important aid in their dog’s lifelong health care, providing for less apprehension and better overall outcomes for your dog.
Become informed and share your desires about general anesthesia with your veterinarian. If she is not sensitive to your concerns, consider selecting another practitioner. Incorporate traditional and holistic practices into your support regimen for your dog, and enjoy the longer and healthier life your canine companion can experience with the help of today’s sophisticated veterinary medical techniques.
Also With This Article
Click here to view “What You Should Know About Anesthesia Before You Schedule Your Dog’s Procedure”
-by Lorie Long
Lorie Long is a frequent contributor to WDJ. She lives in North Carolina with two Border Terriers, Dash (a three-year-old female and agility queen) and Chase (a five-month-old male with an agility future).





