My friend Chris was awakened by a bump in the night – a noise coming from the living room in the middle of the night. She listened intently for a moment, and, hearing nothing more, fell back asleep. But when she heard a dog’s nails scrabbling wildly on the hardwood floor in her hall a few hours later, she remembered the bump sound and jumped out of bed to investigate.
She found her Bloodhound/Border collie-mix, Indi, thrashing on the floor. At first she thought Indi was having a seizure; the dog’s front paws were madly paddling at the slick floor. Then Chris realized that Indi’s back legs weren’t moving at all.
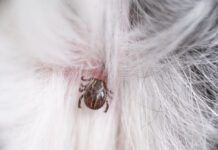
I would have had heart palpitations, but Chris used to work in a veterinarian’s office, and she instantly suspected tick paralysis. As she comforted and calmed the big dog, she ran her hands all over Indi’s body, feeling for an engorged tick. After a few minutes, she found one in Indi’s armpit; it was swollen to the size of a fat sunflower seed. She removed the tick, taking care to get the entire insect (mouthparts and all), and kept searching. Only when she was satisfied that there were no more ticks on Indi’s body, did she get dressed and prepare to take the dog to the emergency vet clinic.
Tick paralysis is caused by a neurotoxin produced by egg-engorged female ticks, who transmit the toxin from their salivary glands to the dog during feeding. The production (and transmission) of the toxin is greatest when the tick has been attached to and feeding from the dog between five and seven days. Five species of North American ticks produce the neurotoxin: the blacklegged tick (a.k.a. the deer tick), American dog tick, Rocky Mountain wood tick, the Lone Star tick, and the Gulf Coast tick. Most North American cases occur between April and June, when the ticks are at their peak reproductive activity.
If your dog suddenly seems paralyzed, there is a good chance it is tick paralysis. Here are steps to take when you suspect tick paralysis in dogs:
1. Check your dog immediately for ticks, and remove any you find. Then check again just in case.
The sooner you remove the tick, the better the dog’s prognosis. The earliest sign of this condition is often a change in the dog’s ability to bark, caused by laryngeal paralysis. He may also have trouble eating, and may gag, drool, cough, or vomit. The back legs are almost always the first to be affected, but as the paralysis spreads, he may lose coordination of all four legs. Death can occur if the paralysis stops the dog’s breathing. However, the moment the tick is removed, the dog will slowly start to improve.
2. Don’t give your dog water (or food).
While you want your dog to stay cool, and you do want him to be well-hydrated, if his larynx is partially paralyzed, he may not be able to swallow properly and can choke. Taking water or food into his lungs due to the incoordination could trigger further health crises.
3. Go to the veterinarian, and try to keep your dog calm.
If your dog is having trouble breathing, get him to the vet as quickly as possible so oxygen can be administered. Keeping him calm and cool will reduce his need to pant.
4. If you don’t find a tick, take him to the vet as soon as possible anyway.
Your vet may be able to find a tick that you could not, but if no ticks are found, further tests will be needed to determine the cause of his condition.
The vet will probably administer intravenous fluids, to help flush the toxin from your dog’s system. No other treatment is generally needed. Most cases of tick paralysis resolve completely within 24 hours of removing the tick, as long as further complications have not developed (from a lack of oxygen or inhaling water, for example).
5. Prevent further tick bites by any means necessary.
If ticks are numerous in your area, make sure your dog is treated with a spot-on tick repellent such as Frontline. According to many anecdotal reports, these preparations are less effective today than they once were – but they are still more effective than nothing, and more effective than any of the homemade sprays made from essential oils that we’ve tried. It may also be wise to avoid trails or areas where ticks are found during the peak season (April to June) for the tick’s production of this toxin.
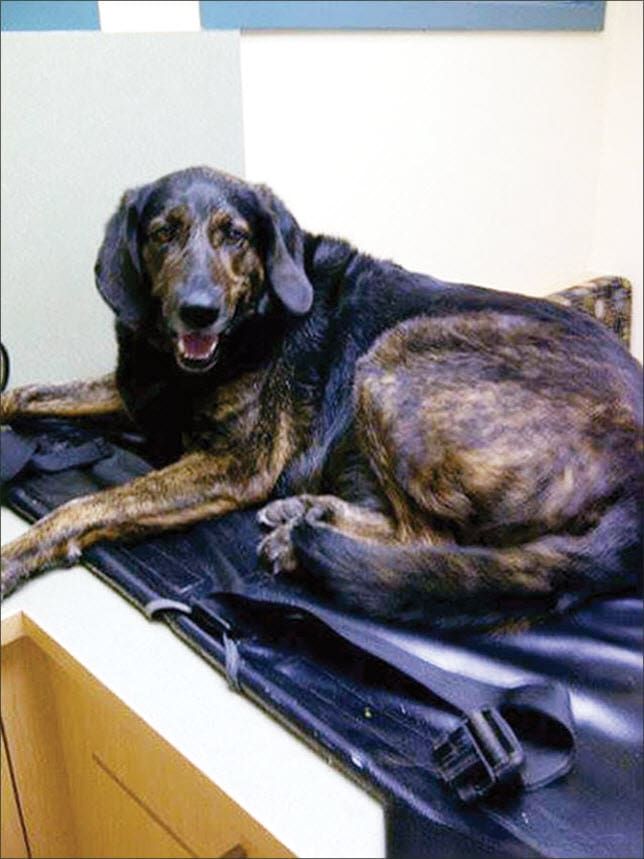
Indi spent the day receiving fluids under observation at the vet’s office. By the time Chris picked her up in the afternoon, she was able to walk (somewhat woozily) out of the clinic and hop into Chris’ van by herself. By bed time that night, she was completely recovered.





Our Bichon woke up yesterday with his back legs paralyzed. Only his front 2 legs are good but his left front leg (Arm) is not doing so good. We didnt find a tick on him either but this read seems to be exactly what our dog has. It all happened from one day to another.
This happened to my Standard Poodle after I had been fighting ticks and I thought he was tick free. The young vet I saw immediately said he needed an MRI. Of course people want to do all they can afford (or sometimes more) to save their pet. Never was tick fever mentioned! Be sure to ask for 2nd opinion from Senior Veterinarian! Worth it for new vet grad to learn rather than refer out to specialists for unusual cases.
I’m thinking of using Bravecto. Its oral and kills attached ticks in 12 hrs.
Seems to be the best solution to a bad problem.
Been used for 20 yrs or so in Australia so lots of data for it.
Any thoughts on it?
Hi please help me my dog paralysed,found a tick on him,it’s a pekinese,what should I do pls I don’t have money
How is your dog doing now? The paralysis usually resolves itself in a few days if all the ticks are removed.
Nned help animal hospital drained me but did nuthing my rotts been down now for 2 full days seems paralyzed on 1 side found a tick on her at clinic but it was just crawling on her fur no tellin if it bit her but vet did nuthing but sure did take almost 500 please any ideas im broke with kid on way