[Updated January 10, 2019]
When Laurie McCauley was in college in the late 1980s, she worked for a veterinarian who was nearing retirement. Recalling his veterinary-school days earlier in that century, he told her of a fellow student whose senior-year project was to periodically take a dog, break multiple bones, and then fix them. As incredibly inhumane as that sounds to modern dog lovers, “this was accepted at the time,” says Dr. McCauley, now a board-certified rehabilitation veterinarian and medical director at TOPS Veterinary Rehabilitation in Grayslake, Illinois. “They believed that animals did not feel pain.”
We’ve come a long way, baby. In the last few decades, veterinary medicine has come to embrace the idea of pain management for dogs and other companion animals. “Some of this is due to better recognizing behaviors that indicate an animal is in pain,” says Beth Boynton, DVM, FNAP, a professor of wellness at the College of Veterinary Medicine at Western University of Health Sciences in Pomona, California. “They tend to ‘hide’ signs, so the subtle cues are often lost. And we have much more effective and safer medications to use to help them than in the past.”
As recently as the late 1980s and early 1990s, Dr. Boynton continues, many veterinarians recommended no pain control for animals after surgery, believing it would keep them “quiet” so they wouldn’t move around and would heal faster. “We know from studies since then that that is not the case in any animal or human,” she says. In fact, administering pain medication before a dog even awakes from anesthesia is now standard procedure, as discomfort is more difficult to control once the nerves that signal pain have been activated. “Pain control helps healing, and that control should be started early. In fact, it is part of the standard of practice for all veterinarians, and ‘relief of animal suffering’ is in our Veterinarian’s Oath.”
Indeed, this newly minted attention to pain relief in dogs is as much a response to good science as it is about compassion. “There is research that shows that 60 percent of pain receptors in the body are ‘sleeping,’ and if they get ‘woken up’ by pain lasting 12 to 24 hours, then any later pain incident in the life of the patient is exacerbated,” Dr. McCauley says.
All this has led to an unprecedented focus on avoiding pain in dogs, even before it begins. Administering pain relief for “routine” procedures such as spaying is now standard practice. Dogs who need to stay quiet while recuperating are given light sedatives along with their pain medications, as opposed to letting their discomfort keep them immobile. “Modern veterinary thinking is that all pain should be relieved – period,” Dr. McCauley says.
Lucy Clark
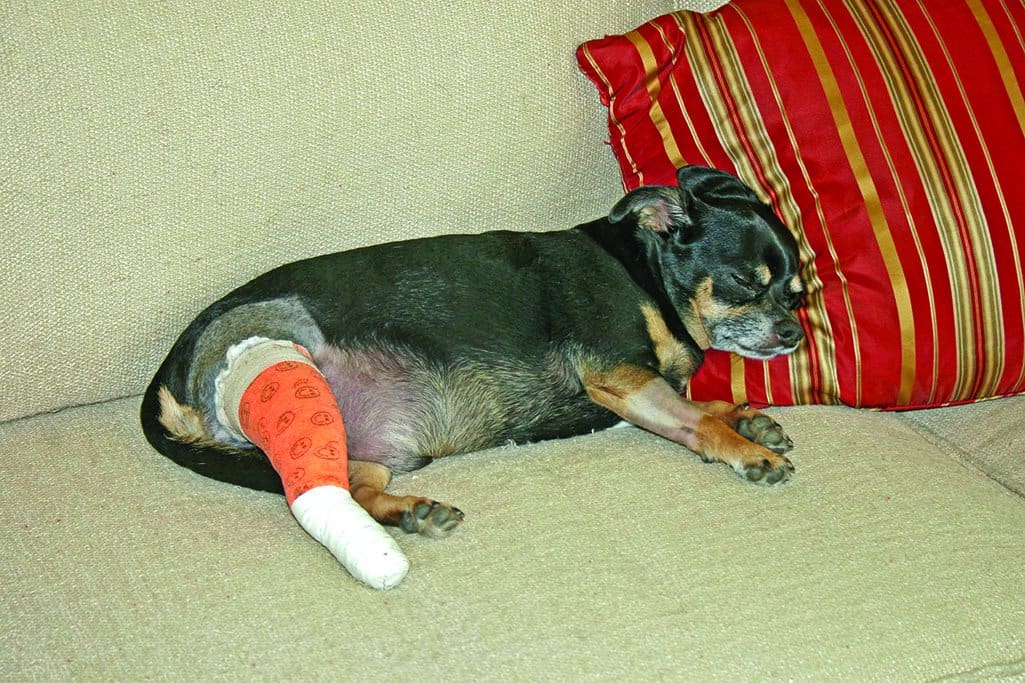
Types of Pain in Dogs
Pain is a response to cell damage or injury in the body. There are two types: Acute pain is often defined as pain that results from inflammation and healing after injury, and it can last for as long as the anticipated healing time, up to three months. Chronic pain is pain that continues on after that expected time frame.
Pain can also be classified by how it is generated. Nociceptive pain stimulates specific pain receptors, which may sense temperature, vibration, or chemicals released by damaged cells. Inflammatory pain derives more gradually from an activated immune system that responds to infection or injury. Pathological pain, which results from excessive tissue damage, produces extended discomfort and abnormal sensitivity. And maladaptive pain persists after healing has completed, caused by changes in the nervous system.
Earlier this year, in collaboration with the American Association of Feline Practitioners, the American Animal Hospital Association released updated guidelines for pain management in dogs and cats. The paper stresses that veterinarians need to anticipate their patients’ pain-management needs, and reassess continually until the pain is resolved.
The acronym “PLATTER” has been devised for pain management: PLan ahead with a patient-specific plan; Anticipate what the pain-management needs might be; TreaT, factoring in the type, severity, and duration of pain that is expected; Evaluate how effective and appropriate the treatment is, using a client questionnaire or a pain-scoring system, and Return to the patient to see whether pain management needs to be discontinued or modified further.
How Dogs Show Signs of Pain
It’s long been observed that dogs seem to try to hide any indication that they are in pain; biologists speculate this is based in some sort of survival instinct. If your dog has a potentially painful condition, you need to watch for little “tells” that indicate she may be experiencing discomfort.
Several veterinary institutions have developed scales that can be used to quantify the level of pain that a dog is feeling. The International Veterinary Academy of Pain Management (ivapm.org) offers a list of symptoms of pain, compiled by Dr. Michael C. Petty. They include:
-
Reluctance to walk on slippery surfaces or use stairs.
-
Becoming selective about what types of furniture to jump on and off of.
-
Attempting to stand with the front legs first.
-
Multiple “false starts” and circling when attempting to lie down.
-
Reduced running and jumping.
-
Abnormal wear on nails.
-
Unwillingness to initiate play or other interactions.
-
Aggression toward other animals.
-
Dislike of being petted or touched.
-
Change in sleep patterns.
-
Stiffness.
-
Decreased appetite.
-
Housebreaking lapses.
Types of Pain Medications for Dogs
The drug group most commonly used by veterinarians are non-steroidal anti-inflammatory drugs, NSAIDs (pronounced as “en-saids”). “They are great if there is active inflammation, but not as good if the pain is chronic in nature and the inflammation has ceased,” Dr. McCauley notes.
Examples of commonly used veterinary NSAIDs are carprofen (brand name, Rimadyl), etodolac (Lodine), meloxicam (Metacam), deracoxib (Deramaxx), and firocoxib (Equioxx and Previcox).
Aspirin is an over-the-counter NSAID, but should not be administered without a vet’s oversight because it has more harmful side effects and is less effective than approved medications. (And while we are on the subject of human pain relievers, owners should never administer acetaminophen, which is the active ingredient in pain relievers such as Tylenol. While some vets do use acetaminophen in dogs, it needs to be very carefully monitored.)
NSAIDs are generally safe, but can cause liver or kidney damage in some dogs. “Pets need to have blood tests prior to going on medications and be monitored appropriately while on them,” Dr. Boynton says. “Some pets develop serious liver or kidney disease while taking drugs and that needs to be detected as early as possible to minimize harm.”
Watch for adverse signs, such as behavior changes, reduced appetite, skin redness, vomiting, or loose or tarry stools, and contact your veterinarian immediately.
There are three other commonly prescribed pain medications in dogs:
-
Tramadol is a weaker opiate that does not require the extensive paperwork of more heavily regulated opiates such as morphine or codeine. (And in dogs as opposed to people, the drug is not metabolized into an opioid.) Unlike NSAIDs, Tramadol does not reduce pain and inflammation at the injury site, but rather changes brain chemistry to inhibit the reuptake of serotonin and norepinephrine, two chemicals associated with mood and responsiveness to pain. Used to control moderate to severe pain, Tramadol is sometimes prescribed for older dogs with chronic pain from arthritis or cancer. Side effects can include upset stomach, decreased heart rate, coughing, and constipation. In some states, Tramadol is now a controlled substance, requiring veterinarians to have a license from the Drug Enforcement Administration (DEA), and carefully log how it is dispensed.
-
Gabapentin is often used to control seizures in dogs and cats, because it stabilizes excessive electrical activity in the brain. But it also works well to help control nerve-related pain, and chronic pain from cancer and arthritis. Some dogs may experience vomiting, drowsiness, loss of balance or diarrhea.
-
Amantadine was initially used as an antiviral medication, but today is mainly used for pain relief. It works by inhibiting the nervous system’s NMDA receptor, which creates the sensation of chronic pain. Amantadine can be quite expensive, Dr. McCauley notes, but “is excellent for ‘big pain’ like an amputation.” Potential side effects include gastrointestinal disturbances such as nausea, vomiting, loss of appetite, flatulence and diarrhea, as well as agitation, which often dissipates after the first few days.
While all these medications can be used individually, they can also be used together so that their pain-relieving qualities outweigh the sum of their parts. And because less of each drug is used, this can mean little to no side effects. But, Dr. Boynton stresses, “this takes careful calculation, because some drug combinations are harmful or fatal.”
Dreamstime.com

Opiates: Not for the Masses
Veterinarians can prescribe opiates such as morphine for their canine patients. There isn’t a concern about addiction, because dogs can’t manipulate veterinarians into prescribing more of a particular narcotic because they just want to get high. Their human counterparts, however, aren’t always as transparent.
“The problem the veterinarian has to watch out for is if the client gets the medications for the dog and then uses them for themselves,” Dr. McCauley explains. “For this reason, the DEA has done a great job of creating guidelines to prevent veterinarians from overprescribing scheduled drugs.”
“Sometimes opioids are the best choice or part of a combination approach, and many of these drugs are a concern for human toxicity or abuse,” Dr. Boynton adds. “Pharmacy tracking is being better developed to monitor for abuse.”
Because of all the paperwork and close governmental scrutiny, many veterinarians do not prescribe opiates. (And some worry that having them on hand in the practice may also encourage break-ins.) But such strong narcotics may have a place in your dog’s care – if, for example, you are performing at-home hospice for a dog who is dying from a painful cancer. In such cases, have a candid conversation with your veterinarian to discuss concerns on both sides of the exam table.
If your veterinarian writes a prescription for an opioid for your dog so you can have it filled at a human pharmacy, be sure not to allow substitutions, Dr. McCauley warns. “For instance, Hydrocodone commonly comes with acetaminophen, which can be toxic for dogs depending on the dose.”
Integrative Approach
Such a “multi-modal” approach isn’t just for pain-relieving drugs. In its 2015 guidelines, the AAHA discusses the importance of an integrated approach to managing pain – one that does not rely solely on drugs.
Dr. McCauley ticks off a long list of complementary modalities that can help relieve a dog’s pain and speed healing:
-
Rehabilitation is a combination of pain management and making the animal stronger, using exercise to strengthen the affected area to prevent further injury or degeneration.
-
Laser therapy has hit the veterinary field by storm, she notes. “Research shows that it not only significantly decreases the inflammatory mediators, but also affects the nerve cells to decrease pain and inflammation.”
-
Acupuncture has been around for millennia, though its introduction into American veterinary practices didn’t start until the 1970s. “More and more vets are accepting this as mainstream and using it for all types of medicine, not just pain relief,” Dr. McCauley says. While not all acupuncture-certified veterinarians are well versed in Chinese herbal medicine, many are, and they can prescribe herbs that can help with pain relief. (As always, veterinarians need to be careful about dosage, as well as how drugs and herbs may interact.)
-
Dr. McCauley is a proponent of tPEMF units such as the Assisi Loop (assisianimalhealth.com). A non-invasive, non-pharmaceutical healing device for animals, the loop uses low-level energy pulses to reduce pain and inflammation, and speed healing. “We use it for acute or ‘acute on chronic’ problems,” Dr. McCauley explains. (An example of the latter is when an arthritic dog compensates until he plays hard or goes for a long walk, and then is sore.) “A beautiful thing about this is that we can sell them to our clients, and they can do the treatments as needed and do it at home.”
-
Dr. McCauley notes that massage therapy, manual therapy (which uses joint manipulation and mobilization as well as muscle manipulation), and chiropractic therapy can all relieve pain as well as muscle and joint problems for diminishing or eliminating pain and allowing improved movement.
While there are many options for augmenting your dog’s pain management, don’t forget the basics: “First, the diagnosis should be accurately made,” Dr. Boynton reminds. “If there is a broken bone, for example, that needs to be fixed before the animal will get real relief. Many times what is assumed to be arthritis may be something treatable, or it could be a serious cancer or infection. Signs can be very confusing in pets.”
Don’t Be Part of the Problem
The AAHA/AAFP guidelines stress that pain management requires a “team oriented approach” that includes the owner as a vital link. Because pain diagnosis depends so heavily on the dog’s behavior, noting changes in how your dog acts, plays, moves, and interacts in his normal routine is crucial.
Dr. McCauley notes that the more emotionally invested an owner is in her dog, the more likely she will appreciate the importance of pain management. “The people who have a four-legged furry child who sleeps, if not in bed with them, then at least in the bedroom, are the population that care a lot about pain meds and quality of life,” she says.
Dr. Boynton adds that far too many owners are unaware of the importance of pain medication for their dogs because they don’t appreciate just how stoic many dogs can be.
“There is still quite a lot of resistance. People often don’t understand that an animal who isn’t whimpering may be in horrible pain,” she says. “Animal survival in the wild often meant that they had to hide pain and keep going with the group, so signs of pain are often very subtle. People also may think that medications are expensive or dangerous.”
Bottom line: It’s not humane to let your dog suffer, and the science shows it’s not healthy, either. Most dogs can be given some type of pain control: Work with your vet to determine the safest and most effective drugs or combinations of drugs to keep your dog comfortable while she’s on the mend.
Denise Flaim of Revodana Ridgebacks in Long Island, NY, shares her home with three Ridgebacks, 11-year-old triplets, and a very patient husband.






