Little attention is paid to the dog’s liver, part of the hepatobiliary tree (which also includes the gallbladder and bile ducts). The oversight is odd, because the liver performs many important jobs in the dog’s body. It’s responsible for everything from production of protein and clotting factors to mobilization of glucose from fat stores to provide energy. It metabolizes drugs and filters the blood. It can even regenerate if damaged. As much as 75 percent of the liver can be compromised before any clinical signs are seen. Due to its many functions, it is also susceptible to infection, inflammation, toxins, and cancers.
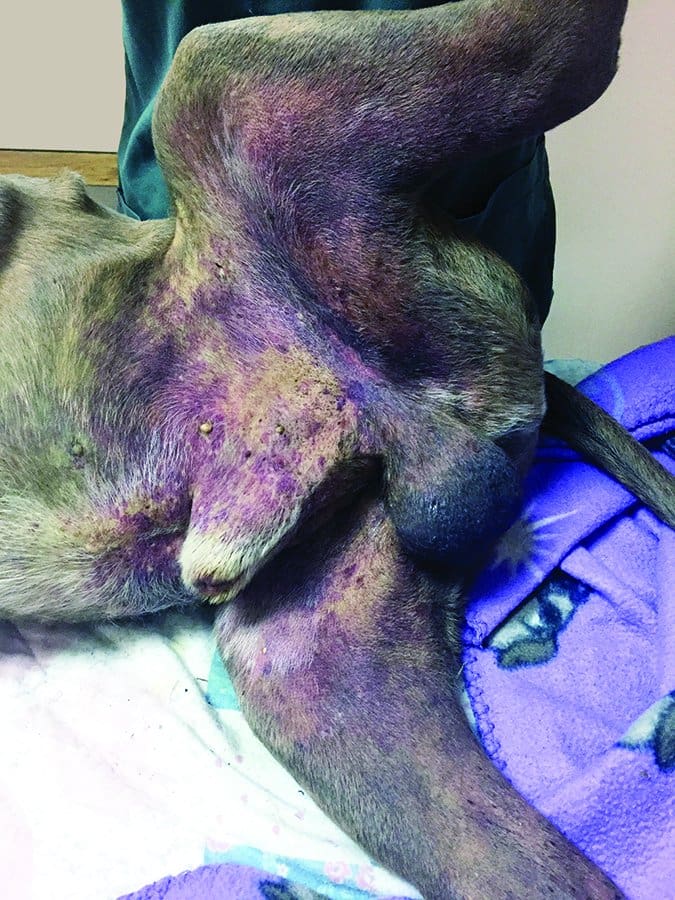
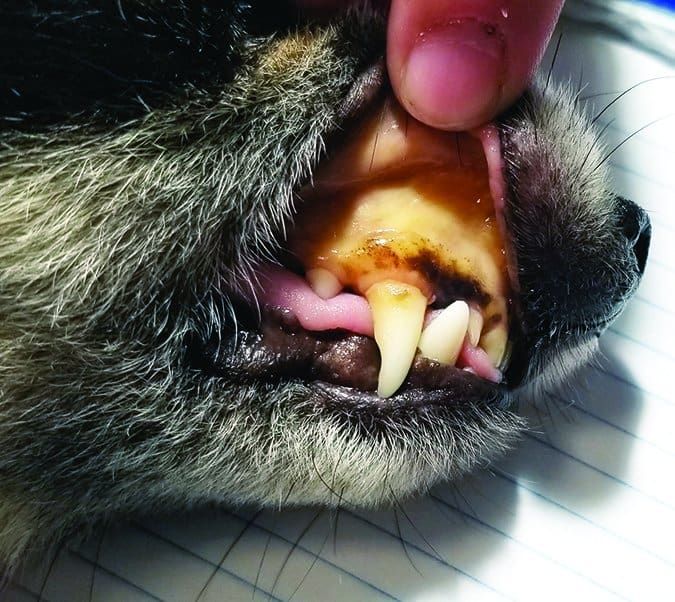
Signs of liver disease can include lethargy, decreased appetite, vomiting, diarrhea, bruising of the skin (small patches of bruising are called petechiae; larger patches are called ecchymoses), abdominal distention, weakness, and a yellow tint to the skin and gums (called jaundice or icterus).
Liver Tests for Dogs
If your veterinarian is concerned about liver disease, she may recommend several tests. The first and least invasive tests are blood tests, including a complete blood count (CBC) and chemistry panel.
The CBC evaluates red blood cells, white blood cells, and platelets, all of which can be affected with liver dysfunction.
The chemistry panel can evaluate values for individual enzymes released by the liver. These are the alanine transferase (ALT), alkaline phosphatase (ALP), gamma glutamyl transferase (GGT), and total bilirubin (Tbili). These tests are basic liver assessments, but they do not indicate actual liver function.
ALT is an enzyme that may be released with any source of damage to the liver. Blunt trauma, anaphylactic reaction, systemic illness such as thyroid disorders, and other problems that have nothing to do with the liver can cause an elevation of ALT in the blood. Just because ALT is elevated doesn’t mean the liver is failing, however. This result is interpreted in conjunction with clinical signs and other bloodwork and imaging changes.
In contrast, the liver enzymes ALP and GGT are released only in response to a problem in the hepatobiliary tree. ALP can also be found in the bones and intestines. Young, growing dogs will often have ALP elevations due to bone growth, while older animals with bone cancer can have high ALP levels, too. Again, an elevated value of this enzyme alone does not necessarily indicate disease.
Bilirubin is a yellow pigment found inside the liver and also in red blood cells. The liver metabolizes bilirubin, and when the liver is failing, blood levels of bilirubin will increase. This is what causes the yellow tint to the skin when a dog has jaundice.
The next assessment looks at the function of the liver. This is usually done with tests for bile acids, ammonia levels, and coagulation profiles. Bile acids are secreted by the liver in response to eating. Testing must be done while fasted; a blood sample is drawn, then the patient is fed, and another sample taken one to two hours later.
The liver is essential in making clotting factors. When it begins to fail, this ability is impeded, and uncontrolled hemorrhage can occur. There are specific tests to evaluate clotting times – called prothrombin time and activated partial thromboplastin time (PT and APTT).
Ammonia is a waste product, and when the liver is failing, ammonia levels will rise. All of these function tests are usually sent to outside laboratories for evaluation.
Imaging of the liver generally includes X-ray and ultrasound. More advanced studies may be conducted with CT scan or MRI with contrast. X-rays can determine if there is liver enlargement or large liver tumors, but it cannot show any of the liver’s internal architecture; ultrasound, CT, and MRI are used for this.
Samples of the liver can be taken in two ways. In a fine needle aspirate, a small needle is introduced into the liver and suction applied; then the sample is evaluated under a microscope. In a biopsy, a piece of tissue is taken via exploratory surgery or laparoscopically, and is tested with a culture and/or with a microscopic examination.
Types of Liver Trouble in Dogs
Given the complexity of this organ’s work, it shouldn’t come as a surprise that there are a number of different ways that the liver can be compromised. We’ll organize them by the type of problem.
Congenital Problems
The blood vessels in the liver normally have a very particular arrangement. Some puppies are born with extra or aberrant blood vessels called portosystemic shunts (PSS). Think of the liver as a blood filter; with a PSS, much of the blood bypasses the liver.
Symptoms of a PSS develop because the liver is not metabolizing properly due to the abnormal blood flow and the buildup of waste products in the blood. These symptoms may include abnormal behavior (particularly after eating), failure to gain weight and grow, and seizure activity. Liver function tests (such as a test for bile acids) and imaging can often identify the shunt. Surgery to improve blood flow to the liver is the treatment of choice in young dogs.
Some breeds are particularly prone to PSS. These include Yorkshire Terriers, Pugs, and Miniature Schnauzers.
Portal vein hypoplasia (formerly called microvascular dysplasia) is another congenital problem that can be present at birth or develop later in life. It is very similar to a PSS, and sometimes, it can be extremely difficult to differentiate the two based on the usual liver testing. The difference is that most dogs are asymptomatic, and the abnormality is found on routine pre-anesthetic screening bloodwork or at the time of another illness. The only change may be mild elevations of liver enzymes.
Infectious and Inflammatory Liver Ailments
Leptospirosis is an infectious disease, caused by a bacteria found in stagnant water such as ponds and puddles. It is most known for causing kidney failure in dogs, but it can also induce liver failure. The initial symptoms are vomiting, diarrhea, lethargy, fever, red, painful eyes (uveitis), and sometimes muscle pain and stiffness or cough. Illness can be severe and life-threatening.
There is a leptospirosis vaccine, but it’s generally considered a “lifestyle” vaccine – meaning that it may not be appropriate for all canines. For example, dogs who have little or no access to puddles or ponds may have little risk of encountering the leptospira bacteria, making the vaccine unnecessary. But the fact that leptospirosis is zoonotic (humans can contract the disease) makes some veterinarians (including me) recommend the vaccine for all dogs. It’s best to discuss this vaccine with your veterinarian.
Hepatitis is a general word for liver inflammation. There are several types in dogs, including infectious hepatitis and inflammatory hepatitis. Copper storage hepatopathy is a well-described disease in which the liver accumulates too much copper. Predisposed breeds include Labrador Retrievers, Doberman Pinschers, Bedlington Terriers, and West Highland White Terriers.
Canine adenovirus can cause an infection in the liver. Vaccination has largely eliminated this condition although it can still occur in unvaccinated dogs.
Toxicity-Induced Liver Trouble
The liver is especially susceptible to toxins. As a filter for the body, it metabolizes many of the substances in the blood.
Xylitol is a common sweetener found in kitchens, especially those of diabetics. It prevents wide fluctuations in insulin and glucose in humans. In dogs, however, it can cause a hefty insulin release. This drives blood sugar down, leading to hypoglycemia. The symptoms occur within 30 minutes of ingesting xylitol, and include weakness, tremoring, seizures, and coma. If a large enough dose is ingested, liver failure will occur. This can take two days to a week to manifest, so just because your dog isn’t showing any immediate symptoms doesn’t mean the ingestion should be ignored.
Xylitol is also included in sugar-free gums and candies, as well as some compounded medications and peanut butter. Always check for the presence of this chemical before giving your dog a new treat or compounded medication.

Sago (cycads) palm are another source of deadly liver toxins. These plants were once isolated to subtropical and tropical areas, but today, sago palms are now available almost anywhere. They are extremely poisonous to dogs, leading to death within a day to a week after ingestion. Every part of the plant is considered toxic, so these should not be kept in homes or in landscaping where dogs are present.
The initial symptoms of ingestion are rapid in onset (within minutes to a few hours) and include drooling, vomiting, diarrhea, and lethargy.
If you suspect your dog has eaten sago palm, do not wait to see if symptoms manifest. Immediate and aggressive decontamination is needed. Your veterinarian will likely induce vomiting to remove any sago palm from the stomach, give activated charcoal to prevent further absorption, and then start intravenous (IV) fluids.
Aggressive treatment is absolutely imperative. Most dogs who ingest sago will spend anywhere from a week to two in the hospital. Treatment will include IV fluids, nutritional support, antibiotics for secondary bacterial infections, and other advanced therapeutics such as fresh frozen plasma transfusions and vitamin K administration. Liver values and clotting times will be checked at least daily and maybe more often. If your dog isn’t eating, a feeding tube may be placed through the nose or IV nutrition given into the catheter. The prognosis for survival, even with treatment, is only about 50 percent.
Beware the Deadly Sago Palm
Dr. Kimberly Chambers is a veterinarian in Conroe, Texas. She knew that sago palms (Cycas revoluta) were poisonous, and so when she moved into her beautiful new home, she had the sago palms in her yard cut down and removed.
Some time later, Dr. Chambers adopted a puppy, Theo.Last June, at four months of age, Theo was digging in the yard and – apparently – dug up and chewed some roots of the palm that were still in the ground.
Dr. Chambers didn’t see this happen, but about an hour after he had been outside digging, Theo vomited in the house. The bits of the root jogged her memory; she realized it was likely sago palm roots. She induced Theo to vomit some more, and then drove quickly to the closest specialty veterinary hospital.
At first, it seemed as if Theo might have been treated fast enough. He had only mild elevations in his liver enzymes. He was sent home with liver supportive medications and orders for Dr. Chambers to monitor him closely. But his appetite was poor. He grew, but he remained thin.

Weeks later, since he was still underweight, Dr. Chambers had Theo’s liver imaged with ultrasound. With that, the damage the sago had done to Theo’s liver finally came to light. Despite its ability to regenerate, the liver can withstand only so much damage. Theo’s liver had marked fibrosis (replacement of healthy tissue with fibrous, non-functioning tissue). He also had some fluid in his abdomen secondary to low proteins and a “leaky” liver.
Over the next few weeks, Theo’s abdomen continued to accumulate fluid. Dr. Chambers would drain his abdomen via abdominocentesis, but because of his damaged liver, the fluid always returned. One day, Theo didn’t want to come out of his crate and he didn’t want to eat. His gums were pale and his belly was bloated. Dr Chambers knew it was time. She and her family fed Theo brisket for dinner and breakfast (with whipped cream). And then they said goodbye to him in the most peaceful way possible.
Theo fought a tough battle, but despite early and aggressive, expert care, he died. He serves as an important reminder to keep all sago palms out of houses and yards where dogs live.
Exposure to the toxins in blue-green algae can be fatal within minutes. Blue-green algae (more properly called cyanobacteria) can be found in freshwater lakes, ponds, and brackish water but also in less obvious places, such as aquariums. Algae can be present throughout the year, but is found in higher concentrations in warmer months. Not all blue-green algae makes toxins, but you cannot determine that by looking. Thus, never allow dogs to swim in water with algal blooms.
Cyanobacteria can produce two primary types of toxins: anatoxins, which cause sudden death due to respiratory paralysis, and microcystins, which lead to liver failure. Symptoms of microcystin toxicity are similar to those of other liver toxins and include vomiting, diarrhea, lethargy, and lack of appetite. If blue-green algae ingestion is suspected, do not delay in seeking treatment. As with other toxins, it will center on supportive care, as there is no antidote.
Medications are a common source of deadly liver toxins. Several medications that are frequently used by humans have been implicated in canine liver failure. Acetaminophen can be used at safe levels in dogs. It is often used in oncology when combined with opioid medications to control cancer pain. Like any substance, the dose makes the poison. At high enough doses, acetaminophen can cause liver failure.
Carprofen, a common non-steroidal anti-inflammatory drug (NSAID) used for the treatment of pain, has been implicated in liver failure. Why some dogs develop this rare problem is unknown. Overall, carprofen is an extremely safe choice for pain control but, rarely, a dog will develop problems. This may be more common in Labrador Retrievers for unknown reasons.
Because of its reliance on the liver for metabolism, phenobarbital can lead to liver failure in some cases. This is a ubiquitous medication in veterinary medicine, used in the control of seizures. Dogs on phenobarbital will need monitoring of liver values, and if indications of hepatic damage occur, may be switched to a newer anti-seizure medication such as Keppra or zonisamide.
Acquired Liver Problems
Some liver ailments are acquired over time, not from an acute insult. Vacuolar hepatopathy is an age-related condition characterized by liver cells (called hepatocytes) that appear swollen and foamy under a microscope. Liver cells accumulate damage over a lifetime; when stressed, they respond by swelling and developing vacuoles – little fluid-filled cysts inside the liver cells themselves. This often results in an enlargement of the liver. This non-specific change can be insignificant or linked to a host of illnesses.
Some of the most common causes of vacuolar hepatopathy are long-term steroid use or chronic steroid overproduction (as in Cushing’s disease) and the use of phenobarbital for seizure control. The findings on bloodwork can be nonspecific but generally include an elevated ALP. If your dog is otherwise healthy and asymptomatic, your veterinarian may not be alarmed by this test result. However, if there are symptoms of illness, more testing is indicated.
The liver does develop cancers. The most common are hepatic adenocarcinoma and hemangiosarcoma. There may be no symptoms as liver cancer develops. Sometimes, a large liver tumor is found on routine examination or through senior bloodwork. This is the ideal situation. If found incidentally, many liver tumors can be successfully removed. Hepatic adenocarcinomas are often completely cured by removal, as they are slow to metastasize.
Hemangiosarcomas, in contrast, are much more aggressive tumors. They grow silently and then rupture. Often, they are discovered when a previously healthy, older dog collapses suddenly. Surgery will address the hemorrhage and remove the source of bleeding, but by the time they are discovered, these tumors have already spread. Surgery alone can yield up to three months of survival time, while adding chemotherapycan increase survival to six months to one year.
Liver Support for Dogs
There are many medications that your veterinarian may use to treat your dog’s liver disease. But there are also several good over-the-counter supplements that can help support a damaged and healing liver.
Denamarin and vitamin E have antioxidant effects in the liver, as well as some anti-inflammatory properties. Denamarin is a canine-specific product containing silymarin, an extract of milk thistle, which offers particularly good anti-inflammatory action. Vitamin E is a fat-soluble vitamin found in high concentrations within the liver. Both supplements can be used in addition to conventional medical treatments to support a damaged liver.
Turmeric has recently received increased attention for its anti-inflammatory effects in both human and veterinary medicine. While there are no large, controlled studies evaluating its efficacy, it is safe for use in dogs. A word of caution: Don’t buy from sketchy online sources or administer human products. Seek out a reputable veterinary product such as CurcuVet made by ThorneVet (available from Amazon and many veterinarians). Internal quality control is essential in finding a good product.






My dog miniatureEskimo 3 months ago was diagnosed withenlarged heart it’s some cure for hem ?