No word strikes fear into the hearts of dog owners like bloat. It is a fairly common occurrence and requires immediate intervention and surgical treatment. But what exactly is it? And what should you do if you suspect that your dog is suffering a bloat?
Bloat is the nontechnical term for gastric dilatation and volvulus (GDV), a condition in which the stomach rotates around itself to become twisted. The stomach can twist halfway (a 180-degree torsion), all the way leading to a 360-degree torsion, or anywhere in between. Once twisted, the stomach becomes stuck, and fluid and gas cannot exit. A dog cannot vomit, as the entrance to the stomach (the cardia) is obstructed, and nothing can leave the stomach via the intestines, because the exit (pylorus) is also blocked.
Due to this twisting, the stomach rapidly fills with fluid and gas, leading to abdominal distention. As the stomach quickly expands, blood vessels supplying it rupture and lead to hemorrhage. The massive stomach pushes on the diaphragm, making it hard for the dog to breathe. It also causes pressure on the caudal vena cava, which brings deoxygenated blood from the body back to the heart. Without blood circulating, shock occurs rapidly.
Bloat Symptoms in Dogs
The symptoms of bloat are classic and include restlessness, discomfort, pacing, abdominal distention, gagging, salivating, and non-productive retching.

The earliest signs may be as subtle as increased drooling and pacing/restlessness. Frequently, this occurs soon after a meal, especially if the meal is followed by exercise. Certain breeds are more likely to develop bloats such as Great Danes, Standard Poodles, and Dobermans, but any breed can bloat. Sex does not seem to be related.
Bloat is an immediate emergency. The longer the stomach stays twisted, the more damage is done. If twisted long enough, the stomach tissue will die and rupture, leading to spillage of stomach contents into the abdomen.
If you suspect your dog is bloated, an emergency trip to the veterinarian is a necessity. Do not wait overnight to see your veterinarian in the morning. The sooner that GDV is addressed, the better the chances for recovery.
At the Veterinary Clinic
When you arrive, the technical staff should take your dog directly to the treatment area for examination. Bloat can often be determined based simply on signalment (age and breed) and physical examination. The belly will be tight and tympanic (meaning like a drum).
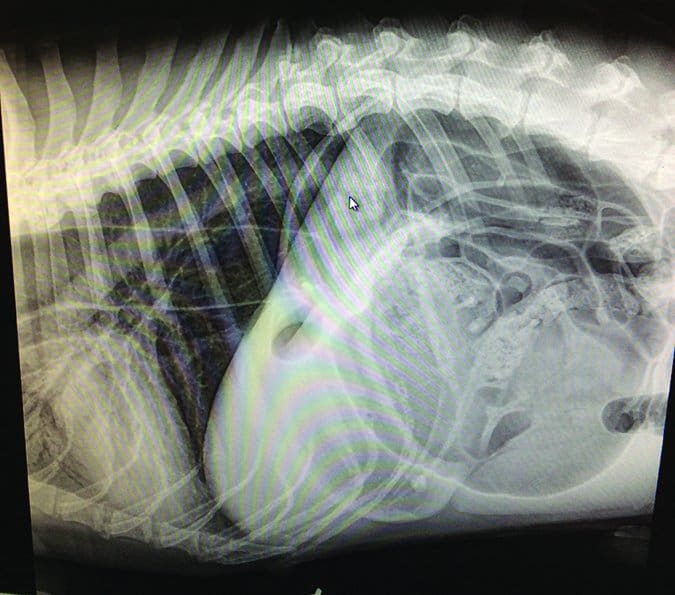
To confirm the diagnosis, your veterinarian may take a right lateral abdominal x-ray. This will reveal a classic “double bubble” – a folded, compartmentalized stomach. They are often called “Smurf hats” or “Popeye arms” because of their characteristic appearance.
Time is of the essence, so your veterinarian will treat your dog immediately. A quick physical exam generally will reveal the following abnormalities: an elevated heart rate, panting or fast breathing, a tight, drum-like abdomen, and abdominal pain.
An IV catheter will be placed to administer fluids and correct shock. Pain medications are needed as soon as possible and may include an opioid such as hydromorphone, morphine, or fentanyl.
As your veterinarian and the technical staff work to stabilize your dog, they will also conduct diagnostic testing. This will include bloodwork to evaluate for internal organ damage, as well as checking blood pressure. In a specialty setting, it’s likely that the veterinarian will also check coagulation factors (your dog’s ability to clot) and blood lactate levels.
Lactate has been extensively studied in GDV. It is produced as a backup source of energy in the body. Lactate is always being produced, but in shock, when oxygen levels are decreased, lactate production is much higher. It can be measured with a hand-held device much like a blood glucose monitor. Many studies have been done to evaluate how helpful this is in determining outcome in GDV patients. Currently, it is thought that a high lactate level that decreases with IV fluids and surgery is a good indication for recovery.
GDV often occurs in older dogs, so your veterinarian also may recommend three-view chest x-rays to evaluate for the presence of any abnormalities. One study showed that 14 percent of dogs with GDV have concurrent aspiration pneumonia, likely from gagging and inhaling drool and watery stomach fluid that can escape the twisted stomach. Many GDV patients are older, and three-view x-rays can also evaluate for metastatic cancer that would make the surgery prognosis poorer. This recommendation is dependent on the vet who treats your dog. Any delay in surgery can be detrimental to your dog, so in cases of elderly dogs (greater than eight years of age) in particular, this recommendation must be weighed carefully.
Stomach Decompression for Dogs
Before surgery, your veterinarian will likely try to decompress the stomach – that is, relieve the gas buildup in the stomach. This can be done in one of two ways. The first is to pass a tube down the esophagus into the stomach – an older but still accepted method. It can often be done in an awake patient. This rapid decompression can help buy time for the twisted stomach. In some rare cases, passing a tube can untwist the stomach, but the procedure also poses the risk of puncturing through the twisted stomach entrance (cardia).
Another method of decompression is called trocarization. In this technique, large gauge needles are inserted through the skin into the stomach to relieve the air. This is currently the more commonly used approach because it is quick, doesn’t require multiple staff members, and can be very effective. It poses a much lower risk to the dog, but is not without risk altogether: it’s possible to lacerate the spleen during this procedure.
There is a great video online of a veterinarian performing trocarization on a Bernese Mountain Dog with GDV.
Surgery for Bloat
The goal in a GDV is to stabilize the patient as quickly as possible before surgery. A GDV can be successfully treated only with surgical intervention. This often puts the veterinarian and owner in a very difficult spot. Decisions must be made quickly and with decisiveness to allow for the best outcome. GDV surgery can be very costly, and most dogs will remain in the hospital for two to three days post-operatively. The prognosis is dependent on each dog and how long the torsion has been present. In general, survival rates for the surgery are high.
Your veterinarian will take your dog to surgery as soon as possible. This should not be done until the patient is as stable as can be expected. To some extent, full treatment of shock is impossible until the stomach is de-rotated in surgery. The patient’s condition should be optimized. This means stabilizing blood pressure, bringing heart rate down to normal or near normal, controlling pain, and decompressing the abdomen either via stomach tube or trocarization.
In surgery, your veterinarian will open the abdomen, identify the twisted stomach, and then de-rotate it. Once de-rotated, the stomach is checked for damage. In some cases, part of the stomach tissue has died and must be removed. The spleen will be checked next. It lies alongside the stomach and shares some blood vessels. When the stomach twists, the spleen does as well. Damage to those blood vessels can lead to a damaged spleen. In some cases, the spleen must also be removed.
Once the stomach and spleen are addressed, the stomach is sutured to the right body wall. This is called a gastropexy. This will prevent the stomach from rotating again in 90 percent of cases. However, in about 10 percent of cases, a dog can still develop a bloat. It is imperative to always monitor your dog for the symptoms of bloat, even when they have undergone gastropexy.
There are several different techniques for gastropexy. The most common is the incisional. This is when an incision is made into the outer layer of the stomach (serosa) and a matching one made on the wall of the body. The two are then sutured together, holding the stomach in place.
Surgery generally lasts about an hour to an hour and a half.
Post-Operative Care
Most dogs will remain hospitalized for one to three days after surgery. Post-operative care will include IV fluids to maintain hydration, pain relief, and close monitoring. Complications can include arrhythmias, hemorrhage, and infection. In some cases, a syndrome called systemic inflammatory reaction syndrome (SIRS) can occur. Disseminated intravascular coagulation (DIC), a massive and fatal collapse of the ability of the body to clot blood, can also occur.

Patients should be monitored around the clock after surgery, preferably at an emergency and/or referral hospital. Not all veterinary hospitals have staff on duty all night, so be sure to ask your veterinarian if this is something that will be available, or whether a transfer to a clinic with a night staff is possible.
Excellent attention to recovery is important. This will include monitoring of heart rate and rhythm (by ECG), temperature, and comfort level. Most patients are fasted for about eight to 12 hours after surgery. They are then offered a bland, easily digestible diet.
Arrhythmia and Bloat in Dogs
It is very common for a dog that has GDV to suffer from arrhythmias during or after surgery.
The most common are ventricular tachycardia and slow idioventricular rhythm. The ventricles are the lower chambers of the heart. When a dog goes into shock, the heart muscle becomes irritable and can develop irregular beats, particularly in the ventricles. Tachycardia occurs when the heart rate is faster than 150-160 beats per minute. When the heart rate is normal but the rhythm is abnormal, this is a slow idioventricular rhythm.
In most cases, these resolve within a week without specific treatment. If the arrhythmia persists, it is important to have the heart evaluated by a cardiologist. Since Great Danes in particular are prone to both GDV and cardiomyopathies, concurrent heart disease could be present.
Bloat Prevention
Much research has been devoted to this topic. The causes for GDV are poorly understood. At various times, an array of different recommendations have been made to prevent bloat, including the use of raised food dishes, the avoidance of raised food dishes, avoiding exercise after meals, and feeding smaller, more frequent meals rather than one large meal. More recent research has identified a possible link between motility disorders and GDV. At this time, unfortunately, there are no hard and fast rules for preventing bloat.
Prophylactic gastropexy is strongly recommended for the highest risk breed, the Great Dane, as some estimates show one in three will experience GDV. This can be done at the time of spay for females. It can also be done laparoscopically for males at practices that offer this modality.
Standard Poodles, Rottweilers, Irish Setters, and Weimaraners are also considered at-risk breeds for which prophylactic gastropexy should be considered. In other breeds, the benefits versus risks of preventative gastropexy are less clear. But one thing is certain:
No matter what type of dog you own, if you observe the classic symptoms of bloat – restlessness, discomfort, pacing, abdominal distention, gagging, salivating, and non-productive retching – you need to get your dog to a veterinary emergency room ASAP.
Mesenteric Volvulus: A Diagnostic Puzzle
While less common than GDV, mesenteric volvulus is a similar condition that requires immediate veterinary care and can be deadly in a matter of hours. For owners of German Shepherd Dogs and Pit Bulls (the most predisposed breeds) it is especially imperative to know about this condition.
With a mesenteric volvulus, the small intestines twist at their origin (called the root of the mesentery). This leads to obstruction of blood flow and death of the upper GI tract. The cause of MV is unknown. There seems to be an association with exocrine pancreatic insufficiency (EPI) in which the pancreas does not produce digestive enzymes. However, this has been shown in only one study. Other causes have not been identified.
The symptoms are frequently very sudden in onset and include vomiting, extremely bloody diarrhea, abdominal pain and distention, and collapse in a dog that was previously normal. The gums will be pale, and the heart rate and breathing rapid. The abdomen may be distended and extremely painful. An emergency trip to the veterinarian is warranted. Do not wait!
Unfortunately, these symptoms present a diagnostic dilemma for the veterinarian. Acute collapse can represent several conditions including Addisonian crisis, anaphylaxis, and acute hemorrhagic diarrhea syndrome. If mesenteric volvulus is not identified within one to two hours, death often results. Therefore, if your dog exhibits these symptoms, your veterinarian should conduct treatment and diagnostics immediately.
Treatment for Mesenteric Volvulus
Initial treatment and testing should happen simultaneously when possible. An IV catheter will be placed to administer fluids and correct shock (manifested by low blood pressure, high heart rate, and rapid breathing). Oxygen may also be given by face mask or nasal prongs. MV is an extremely painful condition, so pain medications should be given.
Your veterinarian should also be conducting diagnostics at the same time. X-rays and/or ultrasound of the abdomen are critical in diagnosing MV. Bloodwork should also be done concurrently to evaluate internal organ function, as well as determine the severity of shock and to rule out other diseases. Most MVs are readily apparent on x-ray, but this is not always the case. Ultrasound also can be helpful.
Surgery for Mesenteric Volvulus
The treatment for mesenteric volvulus is immediate surgery. Even with prompt surgery, the prognosis is extremely guarded for survival. While the stomach can be twisted for hours in a GDV and the patient recover, the intestines do not tolerate the lack of blood flow for long. As a result, the veterinarian must intervene quickly and decisively.
This can lead to a hard decision for both owners and veterinarians. The diagnosis often cannot be definitively made on x-rays and ultrasound. It can be heavily suspected based on clinical signs, breed, and testing, but until the doctor performs surgery, it is not always a certainty. As a result, owners are often forced to make a major decision with an ambiguous diagnosis and recovery. Like any major emergency surgery, it is expensive. MV surgery and post-operative care can cost several thousand dollars. This is an excellent example of why it is important that you have a close and trusting relationship with your veterinarian, as well as an emergency fund and/or pet insurance, which can help offset the cost and stress in the case of MV.
If mesenteric volvulus is suspected, your dog will undergo rapid emergency surgery to de-rotate the intestines. If too much damage has occurred and the intestines cannot be saved, a resection and anastamosis (removal of intestines and sewing ends together) can sometimes be done. However, in some cases, the damage is too extensive, and euthanasia is necessary.
Post-operatively, the patient will likely be hospitalized for several days and undergo careful monitoring. After surgery, complications such as sepsis, systemic inflammatory response syndrome, disseminated intravascular coagulation, and organ failure can occur. Thus, it is imperative that patients are observed closely after surgery. Complications can occur for several days to a week afterward.
Mesenteric volvulus carries a very guarded prognosis for recovery. It is critical that owners of German Shepherds and American Pit Bull Terriers be aware of the symptoms and act rapidly if they are noted.







Anyone concerned about bloat should read the Purdue study. Elevated bowls are thought to I crease the chances of bloat by 52%
Karen, that study is now very out of date, raised bowls are not suspect in bloat cases.
My son’s dog had the surgery and recovery went well but he now refuses to eat. We have tried chicken and rice, eggs, most everything. Any suggestions? The surgery was 16 days ago.