In my 13 years as a veterinarian, I’ve worked in emergency and general practice, as a freelance writer, a volunteer with the homeless population and most recently, as a palliative and hospice-care doctor.
While all of these positions were rewarding, working in palliative/hospice care has been deeply life-altering and fulfilling. It’s a gift to make end-of-life care as painless as possible. This includes supporting the patient – and owners – in a pain- and fear-free manner.
Perhaps you didn’t even know that this service existed for dogs. The idea of hospice for pets has been around and in practice since the late 1990s. Alice Villalobos, DVM, was a pioneer in the field, and coined the term “pawspice” to describe veterinary hospice work in 2004. The first International Symposium on Veterinary Hospice Care was held in 2009.
Also in 2009, the International Association for Animal Hospice and Palliative Care (IAAHPC) was founded with the goal of promoting animal end-of-life care education, research, and discussion amongst veterinarians and their clients. IAAHPC remains the driving force in advancing hospice care for pets. In 2016, the IAAHPC began offering a course in this work for veterinary practitioners, the Animal Hospice and Palliative Care Certification Program. You can search for certified practitioners at iaahpc.org.
WHAT’S THE DIFFERENCE BETWEEN THESE SERVICES?
While closely linked, palliative and hospice care are different. Both are concerned with the complex web of emotions and decisions surrounding the care of a beloved companion. This includes considering the social, economic, psychic, and physical demands of care.
They differ in that palliative care seeks to minimize suffering and maximize comfort at any stage of life and with any disease process. In contrast, hospice focuses on patients that are terminally ill and helping with a transition to a peaceful, assisted death.
It may be difficult to know when your dog is ready for palliative care or hospice. In the case of a terminal illness, hospice is best started when definitive options have been tried and failed, if there are no definitive treatments, or if you are not interested in aggressive treatment such as chemotherapy, surgery, and/or radiation.
An example of this is when an inoperable tumor is found and the dog is otherwise stable and relatively healthy. Hospice care includes monitoring the tumor and providing pain relief, comfort measures, and other care as the cancer progresses. When quality of life is declining, a peaceful passing can be planned.
Palliative care is different in that it can be started at any time and continue in conjunction with other treatment from your veterinarian. Osteoarthritis is an excellent case for palliative care. While it is a chronic and progressive condition, it does not cause terminal illness. Palliative treatment will focus on supplements, physical therapy, and pain management.
Veterinarians are starting to offer this concurrently with more definite therapies, but you can also find many mobile services that can come to your house for this care. This is helpful for older animals who are stiff and have trouble with car rides or those who suffer anxiety in a veterinary clinic environment. You can ask your veterinarian for a referral (if the service exists in your area) or often directly contact the hospice vet yourself.

Finn is extremely handsome and quite old at 17. He is a mix of Border Collie and Australian Shepherd. To look at him, you would never guess his age – that is, unless you watched him walk up some stairs. Finn has advanced arthritis in his hips and pelvis. As a result, climbing stairs and running can be difficult for him. He still loves to walk and hike with his owners, but as he’s aged, Finn has started slowing down and having longer periods of stiffness after exercise. He also started throwing up and having loose stools and a gurgly stomach occasionally. His veterinarian examined him and conducted diagnostics that included bloodwork and x-rays.
Those x-rays confirmed bone changes consistent with arthritis but also a fuzzy, indistinct area that suggested a tumor in Finn’s abdomen. Finn’s owners discussed these findings with their veterinarian. At Finn’s advanced age, they weren’t interested in extensive diagnostics and treatments, which they feared would be invasive. Finn’s owners called our office and asked for an assessment from our palliative care team.
Finn was a perfect candidate for this care. While his arthritis can be limiting due to the discomfort it causes, and he has intermittent GI upset, his overall quality of life remains good. He eats well and wants to interact with his owners, including going on walks. As a result, we decided together that there were several measures that we could implement to improve his quality of life.
For his arthritis, we started Finn on a low dose of a non-steroidal anti-inflammatory medication to be given daily. While it is tempting to give medication for pain only on a dog’s “bad days,” with chronic conditions such as arthritis, it’s better to keep a patient on this medication daily. We also included gabapentin for further pain control. In addition, Finn was started on Adequan, an injection administered on a tapering schedule that is the only FDA-approved disease-modifying osteoarthritis drug. This means that it modifies the progression of the arthritis. It can be beneficial even in dogs with advanced bone changes.
For his GI disease, since his bloodwork and x-rays did not show a clear cause, we took a symptomatic management approach. I recommended switching Finn to a novel protein diet (meaning one that he had not been exposed to before – in his case, lamb), adding probiotics to his food daily, monitoring his time outdoors to prevent dietary indiscretion, and medicating his nausea symptoms when they arose with Cerenia, a potent anti-emetic.
As of today, Finn is doing very well with his palliative care. He has more energy, less stiffness, and fewer episodes of upset stomach. His owners are very pleased with his progress.
WHAT TO EXPECT
A typical patient in a palliative-care or hospice practice will be seen anywhere from weekly to every few months. We may need to see an arthritis palliative care patient only once every three months or so, whereas a dog with terminal cancer may require weekly check-ins to adjust his medication.
We start by asking for the client to have their pet’s medical records sent to us so we can review detailed information about the dog’s condition, test results, and treatments. Then, in the practice I work for, a client’s initial appointment will be made with one of the veterinarians, who will do a preliminary assessment of the patient. That appointment is about an hour.
During that time, we meet the dog and owners and discuss the client’s goals for treatment. We describe both our palliative-care approach as well as the “nuts and bolts” about how to reach us after hours and what to do in an emergency. We then go over a plan to improve the dog’s quality of life. This plan differs for each patient and for each medical condition.
It is important during that initial visit to be clear about what your goals are in seeking palliative care. As doctors, we strive to provide relief of pain and improved mobility and cognition. But we need to do this within the boundaries of your ability to provide care. Being very clear about goals and limits is extremely helpful for us when caring for your dog.
From there, our clients communicate with us via text, phone, and email. We are available all day, but our clinic does not take emergency calls. This is different with every service, and it is important to know who to contact in case your dog has an after-hours emergency. Here, we refer to our local emergency hospital.
After the initial assessment, if a patient requires ongoing care with subcutaneous fluids, injections, or frequent bloodwork or blood pressure measurements, one of our technicians will take over those appointments, while keeping in contact with the veterinarian on the case.
QUALITY OF LIFE SCALE
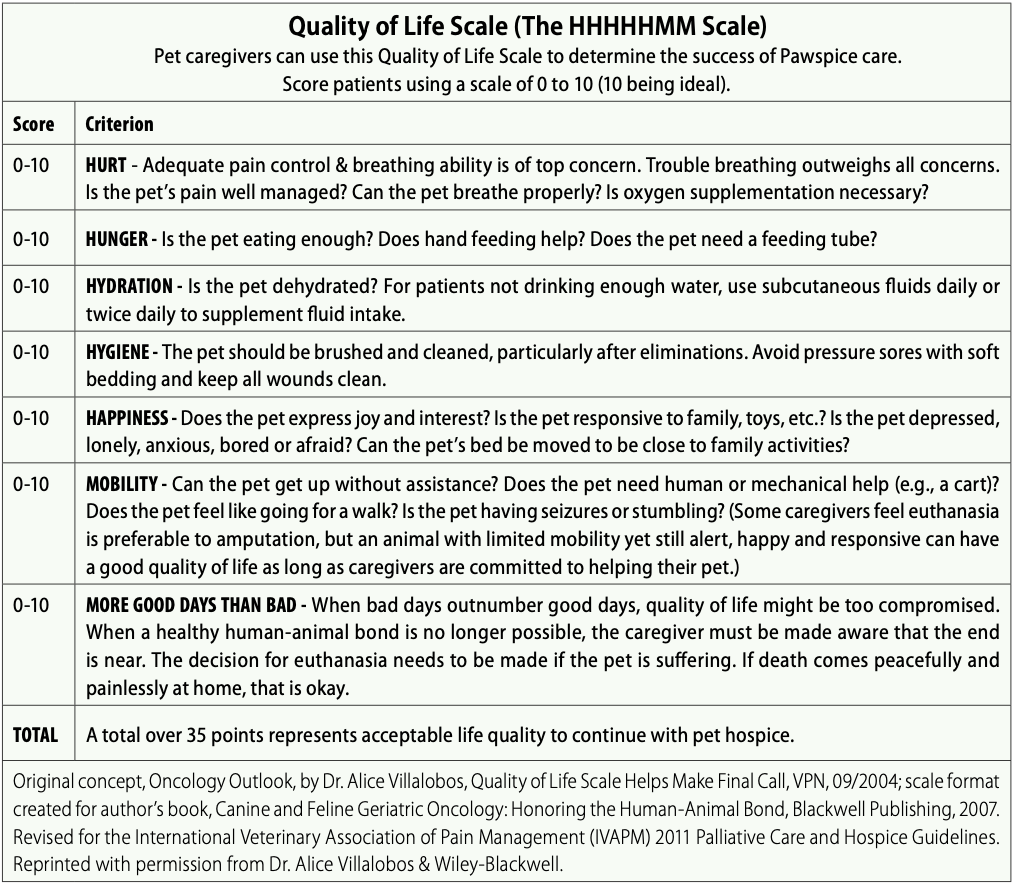
As palliative care continues, the team will check in often to ensure that your dog is doing well and your concerns have been addressed. There are several scales that have been developed to help assess quality-of-life concerns, and these can be very useful in forming an objective opinion on your dog’s condition.
The scale that I use the most is the HHHHHMM scale, which was developed in 2004 by a veterinary hospice pioneer, Dr. Alice Villalobos. The acronym stands for hurt, hunger, hydration, hygiene, happiness, mobility, and “more good days than bad.” A score of zero to 10 (10 being ideal) is assigned to each category. A total of more than 35 points represents “acceptable life quality to continue with pet hospice.” The scale is a helpful tool for reducing the blinding emotion of evaluating your dog’s comfort and happiness.
END-OF-LIFE DECISIONS
Once care is no longer providing comfort and quality of life for your dog, your veterinarian will start the difficult discussion of planning your dog’s transition. It is unfortunate, but an unassisted death is rarely smooth and peaceful for animals or humans. As a result, having a plan in place is very important.
Veterinarians can help ease your dog’s passing with pain medications and profound sedation before administering the euthanizing drug. While every practitioner has a preferred protocol, most euthanasia involves an initial medication (injectable or oral) to provide pain relief and relaxation. This is followed by an injection of a solution that slowly “turns off” the central nervous system. This leads to a deep coma followed by death. It’s as if your companion went to sleep. Done properly, it’s as painless and peaceful as possible for such a sad experience. Having a plan in place and discussing the sequence of events with your veterinarian ahead of time will help ensure that it goes smoothly.
I never imagined I would take on this work; in fact, it seems implausible – ludicrous, even – that I would accept such a position.
You see, in 2017, I found myself facing the decision of whether or not to continue life support on my terminally ill child. He had been in palliative care since birth for a condition that had no cure. As he aged, he became ill and dependent on many medications and a ventilator to sustain his life. When he was 5 months old, he developed serious complications after an illness and was hospitalized. He deteriorated, and my husband and I were faced with a terrible decision – the hardest that I have ever made. It was the guidance of our son’s pediatric palliative care team that helped us let go. Our son died with peace and dignity.
In 2020, a job opportunity – working in a veterinary hospice and palliative-care practice – fell into my lap. Initially, I was repelled by the thought. Why would I want to put myself in a situation where I was reliving the same conversations and decisions that I’d made for my beloved son, with distraught pet owners? It sounded like a particular type of torture.
Despite this, a small voice in my mind insisted that I might excel at this. I listened to that voice and took the chance, diving into the field and learning as much as I could. I quickly fell in love with the work – the animals, of course, but also their deeply caring owners and guardians and the stories that they shared.
Sitting with people in intense grief, guiding them and giving them peace about their decisions has helped heal my heart. It is an honor to be a steward for people and their beloved companions at the end of life.






Of my 15 aged rescued malamutes, that lived anywhere from 3 weeks to 3 years, I have always called the vet to come and euthanize him at home in his own comfort zone. All but one told me it was time to go; that he had had enough pain and suffering. They died peacefully in my arms – well a couple had to die at the vet clinic because they were already dying from something when I brought them in but they all had a gentle death.
The one dog that didn’t have a good death would not sedate. It made him more stressed. When we gave him the needle, he would not die but continued to live even though he was down. We had to give him another dose. I will live with that horror for the rest of my life.
My current dog has degenerative myelopathy, arthritis in both elbows, chronic disc disease at the base of his tail with suspected partial disc herniation. And there is right hip dysplasia with moderate arthritic changes as well as possible cruciate or meniscal injury in the right knee. We tried the various drugs and injectables but he seems to be responding better to his present regime. He has acupuncture once a week and rehab twice a week as well as gabapentin and galliprant plus some herbs. He is becoming more comfortable as we continue and I’m ordering some CBD too. He is a happy boy and still plays with his toys. He has learned he cannot run or get up stairs or on the bed but his bed is now beside mine. The vet told me she doesn’t think he has more than 6 months. I have a hard time with that as he only came here two years ago and he will have all the love and good life as long as he can.
Holly, Your dogs condition and treatment strategy is similar to ours with our Vizsla. Plus bladder cancer and geriatric onset of laryngeal paralysis and poly neuropathy (GOLPP). Yesterday we had to let her go. We started on this path thinking the cancer would take her out but it was GOLPP and disk disease. She couldn’t stand without help and could barely walk. She mostly stopped eating and could not defecate. It was a sharp decline in the end but months of slow progression of all her ailments that kept us wondering when would be the right time to let go. When would she tell us? Or would she? Would it be clear? The days prior we agonized over what other treatments to try, thinking maybe laser therapy or restarting water treadmill or steroids would ease whatever be this worsened state of disk or ataxia (muscle wasting). Or medication to improve her stress breathing caused by the laryngeal paralysis. But after the steep decline and the checklist provided in this article and from Ohio State U, the decision made itself crystal clear. It wasn’t even a choice any longer, and our sweet Lucy now told us so. On the last morning, each time I took her outside to pee, she insisted on lying down under or behind bushes where she had never gone before. Dogs, like cats, want to hide when they are close to dying. The final time, she chose the Japanese maple where my other Vizsla and two cats had both sought out the day of their passing. The spark and joy had also left her eyes, but she still wagged her tail (of course!). She spent much of that day in her bed, with our loving presence until the vet arrived. Her eyes now told us she was ready to let go. I am grateful for the subtle signs and for our willingness to ‘listen’ to her. She has always been the wisest among us, we just needed to listen. Her birthday is just 5 days away and we had wished we could make it, but we had no doubt that waiting even one more day would have been torture for her. I do believe that when the time is right for each our pets, the signal will be clear.
Having one of my dogs go thru not sedation – several years ago – it was horrible. I have never had that happen before or since. The terror my Sugar dog went thru still haunts me. On top of the feeling that the vets should have done a better job at calming him & caring. All my other dogs, cats, and my horse had a gentle way out of life, which they deserved.
We are responsible for our animals lives as well as their end of lives and need medical professionals who care.
No matter how short or long their lives are with us, its always so very hard to say good by.
Holly,
I barely have the courage to write that I, too, resonate, empathize and suffer from the PTS of the one that “wouldn’t surrender” to The Time in his life. An 18-year old dachshund with Superman MIGHT was injected 3x – the amount for a 150 lb much larger dog because my Nicky fought each injection and as you described above, “kept getting up” while he was “being put down”. IT KILLED ME and my heart cracked wide open with horror in witnessing it over and over again. I grieve deeply the loss of my first soul mate. I am the type of person that needs to understand, asks the tough questions, wants to look under the rug and behind the doors – to make sense of what happens. When I connected with one of the most amazing Psychic Mediums (Austyn Wells) to connect and communicate with Nicky after his traumatic passing, the one question that haunted me was “why did he fight it when we both knew it was ‘that Time’?”
“He wants you to know that you are not an easy Momma to leave. As hard as you think it was for you to let him go, it was harder for him. He wants you to know that you are MORE THAN ENOUGH, an amazing Mom and someone that is hard to walk away from.”
Those words broke me wider open and with humility, I accepted it as truth… I chose four-legged children in this lifetime and my first was Nicky. To hear what everyone Mom, of human children or four-legged children, begs to know is true… I received as a final physical parting gift from my Buddy… “Mom…you are ENOUGH as you are and I knew I had to leave you and I still didn’t want to.” HEAVEN on EARTH!! The words that keep a Mom rescuing over and over again. And so, we do it again and again. This time knowing and accepting that there is nothing to prove because Nicky told me… I am enough.
Amy, thank you for this truly beautifully written post. I am in the final days of Ozzies terminal something. Internal bleeding which his primary vet hasn’t diagnosed and referred me to unavailable internists. My research tells me it’s progression of 2 cancer surgeries . I stay at home or close to so I will know when it’s time to call the visiting angel- vet to come visit. I got comfort reading your psychic experience and plan to do the same. Thank you, you helped me.