[Updated August 22, 2018]
A dog’s cardiovascular system is physically and mechanically an incredible assemblage, and its capabilities are almost mystical – literally and figuratively driving the dog’s vital force. However, there are several conditions that can adversely affect the heart in a small percentage of dogs (a much lower percentage than that of humans with heart or vascular disease).
Fortunately, there are also several good, natural, and alternative approaches that can be used to treat canine cardiovascular disease. In my experience, these treatments have been as effective (and safer) than the Western medicine treatments I once used.
Ways to think about the canine cardiovascular system:
Conventional Western medicine views the heart as a simple mechanical pump – a very complex piece of machinery with a simple function as a pumping machine. Other scientists have studied the heart from the perspective of its bioenergetics – studies of the bioelectrical and biomagnetic fields are often centered in the heart, and scientific advances in these areas have led some practitioners to conclude that healthy “cardio-energetics” may be the most important contributor to vibrant overall health.
Many holistic practitioners recognize that the heart is also a primary source of the body’s bioelectric and biomagnetic fields. These energetic fields may be the body’s major source of inner information, necessary for proper functioning of the immune system and other organ systems.
Energy fields may also be responsible for much of the body’s ability to create cellular, organ-related, and whole-body memory fields that are in turn connected to other animals and to the natural environment. According to this line of thinking, since the heart is the primary producer of bioelectric and biomagnetic fields, it may be the organ with the highest intelligence in the form of memory. And the heart is almost certainly the organ that has the most potential for interconnecting with other animals (including humans).
Finally, we now know that the heart’s energetics extend into the surrounding environment almost infinitely. Some traditions have said that it is this heart connection – man to beast – that is the reason the animals were sent here in the first place.
How the Heart of a Dog Works
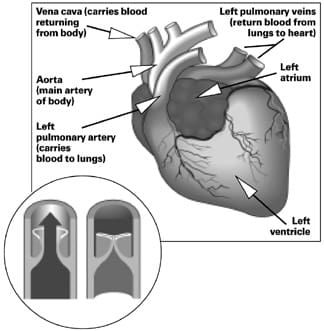
Okay, enough of theory. Mechanically, the heart consists of two pumps, located side by side and joined along their entire length. Each of these muscular pumping stations is comprised of two chambers, the atrium and ventricle. The atria, located at the cranial part of the heart (nearest the head), are primarily receiving chambers where the blood from veins is collected before its passage into the ventricles. Separating each atrium from its adjacent ventricle is a one-way valve consisting of two or three leaflets, or cusps. The valve on the left has three cusps and is called the tricuspid valve. There are two cusps on the valve between the chambers on the right side of the heart, close together in a shape that resembles a bishop’s miter (thus it is called the mitral valve).
The right side of the heart supplies blood to the lungs where the oxygen from outside air is added and carbon dioxide from cells is expired. This part of circulation is a relatively short course, thus the right side of the heart is not as muscular as the left.
After being aerated by the lungs, the blood circulates into the left atrium (via the pulmonary vein). Then, through the tricuspid valve, it enters the left ventricle. From here the muscles of the ventricle propel the blood through miles of vessels, beginning at the aorta. The heart must not only have enough power of contraction to propel the viscous fluid though miles of vessels, but also maintain a constant beating, as they say, 24/7 for the lifetime of the animal.
There are several factors that control heart rate and rhythm. The sinoatrial (SA) node, located in the muscles of the right atrium, instigates the electrical flow that initiates contraction and propels it across the heart. (Surgically implanted artificial pacemakers can be used to stimulate the SA node when necessary – and yes, this surgery has become relatively common in dogs.)
Heart rate is also under biochemical influence. Stimulation of the sympathetic nervous system (with epinephrine or nor-epinephrine, for example, either provided via injection or from the natural “flight or fight” mechanisms) results in increased heart rate; parasympathetic stimulation slows the heart. Heart rate is also inversely related to systemic blood pressure – when blood pressure increases, heart rate decreases, and vice versa. Blood pressure is further controlled by chemicals (angiotensins) that operate at the kidney to conserve or eliminate fluids in the urine.
The Sounds a Heart Makes
The heart has a voice of its own, and the audible dictation of the cardiac voice is easily heard. The closing of each set of valves is forceful enough to make a slight thupping sound, which is easily heard by placing your ear on your dog’s chest. The first of the thups issues from the tricuspid and mitral valve closures and the second from the pulmonary and aortic valves (the egress valves that prevent regurgitation of blood back into the chambers). The thups create the familiar “lub-dup, lub-dup, lub-dup” sound we are all familiar with.
With a low-tech ear-to-the-chest method you can detect obvious heart murmurs, which I would describe as a “mushing” or “slushing” of the lub-dup sound. Heart sounds are, of course, more apparent when a stethoscope is used to amplify them. Electrocardio-grams, echocardiograms, and MRIs may also be employed for capturing the best possible “sound” of the heart.
Checking Your Dog’s Pulse
A normally functioning cardiovascular system should pump blood to all areas of the body with equal force and rhythm; an animal’s pulse is a reflection of the overall health of the system.
Pulses are especially important in Eastern medicine. Traditionally, the character of the wrist pulse is examined and correlated with a diagnosis that then indicates a direction for treatment. The pulse is taken with three fingers, and three depths of pressure are used for the final determination that combines the nine “readings” into a comprehensive diagnosis.
Our dogs don’t have a good “wrist” site for pulse readings, but some veterinarians have substituted the carotid artery (in the neck) and/or the femoral artery (on the inside of the hind leg) for the traditional wrist readings. My own take on this is that we don’t yet have enough information on these “new” sites to be certain they are giving us readings that are accurate for diagnosis, and I know for a fact that my fingers are not trained well enough to feel the subtleties that a Chinese-trained practitioner has learned with decades of practice.
Electrocardiograms for Dogs
Muscle activity requires a transfer of ions from outside muscle cells into their interior; as these ions are transferred across the cell wall, a minuscule electrical charge is produced. An electrocardiogram (ECG or EKG) records the electrical potential, generated by the electric activity of the heart, taken from electrical leads placed on the surface of the thorax and body extremities. Thus the ECG represents the extracellular electric behavior of the cardiac muscle tissue.
ECGs have become a relatively common form of diagnostic aid, available in many veterinary hospitals. Dog and human ECGs are obtained in the same manner – you get the patient to relax, hook her up to several leads that are connected to the ECG recording machine, take readings on a moving graph paper for several minutes, and interpret the readings.
The heart’s “beat” is created by an electrical activation sequence that proceeds, in a self-propagating wave, from the muscles of the apex of the heart to the muscles at the base. Abnormalities can be detected in the frequency and amplitude of the electrical waves, in the spacing between segments, and in the character of the segments and waves.
However, ECG interpretations are notoriously inconsistent; not even the most skilled interpreters (Board Certified cardiologists) agree with regularity. Numerous studies have shown that family practitioners fail to properly diagnose a high percentage of ECG readings. Also, correspondence between computer models of readings, cardiologists, and general practitioners is not good. I know of no studies that evaluate the reader accuracy of veterinarians, but my guess is that we would fare no better than our physician counterparts.
To summarize, I think it is more important that the practitioner has the ability to get his nose out of the machinery and look at the whole animal. And, until I’ve been able to evaluate the animal’s condition – including his energetics – I always take machine-based results with a grain of salt.
Symptoms of Heart Disease
Common symptoms of heart disease include exercise intolerance; persistent, low-grade coughing; reluctance to move; difficulty breathing or forced respirations; poor blood perfusion (delayed capillary refill time or cyanosis with exertion); and, the animal may sit with his elbows out. Remember that these are the same or similar to the symptoms seen with respiratory disease; it is important to separate these two conditions.
Common Heart Diseases
Heart disease is the number one killer of humans. In dogs, however, heart disease is not nearly so prevalent, affecting only about 10 percent of all dogs. Furthermore, the most common types of heart disease in dogs are not the same as the typical heart conditions in people. Following are some of the more common types of canine heart disease.
Congenital heart disease is perhaps the most common heart disease in dogs with an overall rate of affected animals around 1 percent of the total population. Many diseases such as cardiomyopathy and degenerative valvular disease of small breeds of dogs may have a significant heritable component.
Almost any physical part of the heart may be defective at birth. Symptoms vary with the location of the defect, but most often can be detected by listening for a murmur. The murmur may be characteristic for the type and location of the defect, or more likely, ECGs or other diagnostic aids will be needed to pinpoint the problem. Many animals with defects (and audible murmurs) live a quality life without any signs that a problem exists; others may require surgery to repair the defect.
Valve and endocardial diseases can be caused by any number of conditions including genetic abnormalities; aging, worn valves; and infections (many valve conditions can be traced back to gingival infections; as we advised in “Your Dog’s Mouth“, it’s important to keep your dog’s teeth clean).
Adult heartworms can mechanically interfere with heart valve function. Anytime a heart condition is diagnosed, ask your vet to test for heartworm adults and larvae.
Myocardial disease is also a condition with any number of potential causes including hereditary, nutritional, and infectious. Dilated cardiomyopathy can, for example, be due to a carnitine (an amino acid) deficiency in some dogs that apparently inherit an inability to properly metabolize carnitine. Parvovirus and certain drugs can also induce dilated cardiomyopathy.
Today’s most common form of dilated cardiomyopathy affects only large breed dogs, and tends to be an acute problem that occurs in middle-aged dogs. In this disease, cardiac contractile function is lost, cardiac output decreases, the body compensates by stimulating the sympathetic nervous system – which tries to inappropriately increase heart rate, ultimately resulting in arrhythmias and/or heart failure.
Congestive heart failure can also be caused by a number of conditions. Regardless of the cause of heart disease, the body reacts to a decrease in cardiac output by activating the sympathetic nervous system (increasing heart rate and cardiac contractibility), constricting vessels, and activating the biochemical system (angiotensin) to retain fluids and increase blood pressure. While these mechanisms are life-saving in the short term, if they become prolonged, they produce undue stress for the heart muscle. Unchecked, conditions that affect the function of the heart may ultimately lead to complete or congestive heart failure.
Arrhythmias are abnormalities of cardiac impulse formation, conduction, rate, and regularity. Their causes include poor nutrition, genetic defects, problems with electrical conduction across the myocardium, and biochemical disturbances. Quiet, healthy dogs have a heart rate that is slightly irregular, so diagnosing true arrhythmias requires an ECG or other diagnostic aids, and any diagnosis needs to be correlated with clinical signs – if they exist.
Exercise the Dog, Strengthen the Heart
Oxygen is at the top of the list of nutrients needed by a healthy heart, and exercise is the way to be sure your dog’s myocardium (heart muscle) gets a generous supply. All dogs should have at least a daily 20- to 30-minute aerobic trot-along and a few heart-stimulating romps (after having his heart vet-checked as okay), along with several additional trips to the fireplug during the day.
The second best “medicine” for your dog’s heart is an environment that helps him keep from getting fat. Basic metabolism isn’t all that difficult to understand: Whatever the amount of energy (in the form of calories from food) that goes into the body, it will be utilized first for fueling bodily activities (basic metabolism and muscular activity or exercise), and then, whatever calories that are left over as excess will be deposited as fat. So, to keep it simple, if your dog is putting on weight, you need to either decrease the calories he consumes, or increase his amount of daily exercise – or better yet, do both!
Conventional Heart Treatment
Your conventionally trained vet will be able to tell you a lot about Western veterinary care for your dog’s heart condition – especially if she or he has graduated from vet school in the past decade – so I won’t use much space discussing conventional care. Conventional Western treatment for cardiac conditions, of course, depends on the condition, but a normal protocol would include some or all of the following:
• Diuretics – to remove excess body fluids present because the heart isn’t moving them along properly.
• Digitalis (or digoxin) – to improve heart function
• Vasodilators – to lower blood pressure. Nitroglycerine might be the drug of choice here, or others may be selected.
Alternative Care for the Heart
While Western medicine requires a definitive diagnosis before a proper treatment protocol can be initiated, most alternative medicines are prescribed for symptoms. Furthermore, most of the natural and alternative remedies used have a wide range of effectiveness for many conditions, and they are typically safer (although perhaps not as potent) as conventional drugs.
Heart-Healthy Nutrition
The best preventative “medicine” you can provide for your dog is heart-healthy nutrition. The cardiac-impaired patient should be on a well-balanced diet that helps maintain his ideal body weight. If your dog is overweight, a mild reduction in food intake is recommended – about 80 to 99 percent of caloric maintenance levels. Ideal weight reduction would amount to a slow, steady weight loss of 1 to 3 percent of total body weight per week. For specifics on a weight-loss program, see your vet.
Many heart patient dogs are older animals who also suffer from kidney and/or liver disease. Years ago, very low-protein (14 to 15 percent) diets were automatically prescribed for dogs with kidney or liver disease, as high protein diets force the kidney and liver to work overtime. Unfortunately, some of these animals, particularly those who are on this diet long term, may develop malnutrition. Today, we prescribe a diet with a slightly higher level of protein, with a special emphasis on the protein’s quality (high biologic value) and digestibility for these dogs.
Dogs with severe and chronic heart disease may also show signs of protein-energy malnutrition, seen as loss of both fat and lean body mass (“cardiac cachexia”). A diet containing high-quality protein will help prevent this condition. B vitamins, choline, and inositol are good supplements to help maintain a healthily functioning liver.
Diets high in salt may increase blood pressure, which in turn adds to the physical stress to the heart. Low salt diets that include 0.05 to 0.5 percent (dry matter) sodium are indicated for the canine cardiac patient. In addition, stop sharing any salty human treats such as potato chips, pretzels, processed meats, canned fish and vegetables, and cheeses. Many commercial dog treats also contain high salt levels, so check the label for salt content when feeding or treating your cardiac-compromised canine.
Whenever we supplement the diet, the most important consideration is to maintain a balance of nutrients. One of the first things I do with new clients is to look at the supplements they already give their dogs. Invariably, there are several products that contain the same or similar nutrients. Overdoses of any substance can be dangerous. And digestion, assimilation, and metabolism often depend entirely on the overall balance of several independent nutrients. Talk to your vet; don’t just “wing” it!
Human patients with chronic cardiac failure are frequently deficient in iron, zinc, magnesium, potassium, chloride, and B vita-mins. Although similar problems are not well documented in dogs, B-vitamin supplementation is recommended, provided in a balanced vitamin-mineral supplement. Vitamin E (along with a balanced level of selenium) has been shown to be beneficial for heart muscles in many people, and vitamin C has healing activity and helps maintain the integrity of the heart walls and blood vessels.
Some types of diuretics cause decreased levels of potassium (hypokalemia), which predisposes the patient to digitalis intoxication and to cardiac arrhythmias. If your dog receives a diuretic medication, check with your vet to see if potassium supplements are recommended. Also see dandelion (in the herbal section, below) for a natural diuretic that restores potassium levels.
At least two amino acids, taurine and carnitine, have been directly implicated in heart conditions in some species. There is evidence that carnitine may be involved in occasional canine heart problems.
L-carnitine (the bioactive form) is similar to the B vitamins, and its main function is to help transport fatty acids, which are then burned within cells to provide energy. Carnitine deficiency is usually the result of genetic factors that cause the patient to require higher amounts of carnitine than normal. Deficiencies at the cellular level may contribute to some types of muscular problems including muscular dystrophy and cardiac myopathy.
The normal dog’s body can manufacture carnitine if sufficient amounts of iron, vitamins B-1, B-6, and C and the amino acids lysine and methionine are available. Carnitine is naturally available from meats and other animal-origin foods.
Coenzyme Q-10 (Co Q-10) is a vitamin-like antioxidant substance whose actions in the body resemble those of vitamin E. Co Q-10 plays a critical role in the production of energy in every cell of the body, aids circulation, stimulates the immune system, increases tissue oxygenation, and has anti-aging effects. It also counteracts histamine and is thus beneficial for treating allergies, asthma, arthritis, or respiratory disease. It has been shown to be effective in reducing mortality in experimental animals afflicted with tumors and leukemia, and it may reduce the side effects of cancer chemotherapy.
Co Q-10 has a great impact on heart tissue, and it has become the supplement to consider for treating and preventing heart disease. Its mode of action is to strengthen the heart muscles, and it has proven beneficial (in humans) for treating congestive heart failure and high blood pressure. It is thus used for almost any heart condition.
Natural sources high in coenzyme Q-10 include mackerel, salmon, and sardines, and it has also been found in beef, peanuts, and spinach. The amount of Co Q-10 present in the body declines with age, so the aging dog is a prime candidate for supplementation. It is oil soluble and should be taken with oily or fatty foods.
Fatty acids are the basic building blocks for fats and oils. Those that can’t be made by the body and that are necessary for health are called essential fatty acids (EFAs). Every living cell of the body requires EFAs for rebuilding and producing new cells. They are also involved in the production of prostaglandins, the chemical messengers and regulators of various body processes. In addition, EFAs are beneficial for healthy skin and hair, for reducing blood pressure, as an aid in the prevention of arthritis, for lowering cholesterol, and to reduce the risk of blood clot formation.
The two basic categories of essential fatty acids are Omega-3 and Omega-6. Omega-3 EFAs include linoleic and gamma-linolenic acids; they are found in raw nuts, seeds, and legumes and in unsaturated vegetable oils from borage, grapeseed, primrose, sesame, and soybeans. Omega-6 EFAs, including alpha-linolenic and eicosapentaenoic acid (EPA) are found in fresh deepwater fish, fish oil, and certain vegetable oils including canola, flaxseed, and walnut. Note that these oils need to be consumed in liquid form, they don’t tolerate heat, and they are subject to spoilage.
Once again, consult with your holistic veterinarian to ascertain proper dosages of any supplements. Dosages should vary for each individual patient and will depend on whether maintenance or therapeutic dosages are desired. Also, you should be absolutely certain you provide the supplements in a balanced format for proper absorption, assimilation, and metabolism, and for correct interaction with other supplements.
Herbal Remedies for Dogs with Heart Problems
Herbal medicine has much to offer canine cardiac patients. Most herbal remedies convey mild, supportive care without appreciable adverse side effects.
Hawthorn (Crataegus oxyacanthoides) is the queen of all cardiac tonics, with ample scientific evidence to justify its claims. Hawthorn has many beneficial effects on the heart including enhancing oxygen utilization by the heart muscles; improving blood supply to the heart by dilating the coronary arteries; improving metabolism in the heart, which increases the heart’s force of contraction; helping stabilize cardiac activity, thus eliminating some types of rhythm disturbances; and reducing blood pressure.
In short, hawthorn acts on the heart in a normalizing way, by either depressing or stimulating the heart’s activity, depending on the need. It is thus an excellent herb to consider whenever a general tonic is needed for the circulatory system. It is used for treating heart failure or weakness, congestive heart failure, arrhythmia, and high blood pressure (due to its tonic activity, it will normalize high or low blood pressure).
In addition, hawthorn helps stabilize collagen, perhaps via its synergistic activity with vitamin C. Collagen stabilization helps make capillaries less permeable and fragile. Hawthorn reduces destruction from any inflammatory process such as periodontal disease, arteritis, and arteriosclerosis. It can thus be used as an aid for treating the cartilage deterioration and ligament instability associated with arthritis.
Compared with digitalis, in general, hawthorn is safer and milder in activity. Digitalis has a direct action on the heart; hawthorn lowers blood pressure by dilating the peripheral vessels, thus preserving critical reflexive blood pressure regulation. Hawthorn does not cause the cumulative effects that occur with digitalis.
Hawthorn can be used by itself or in combination with digitalis, where it has a synergistic effect. With the combination, your practitioner may be able to lower the digitalis dosage to about one-half the normal dose. Further, the herb may partly ameliorate undesirable effects of digitalis.
Hawthorn toxicities have not been reported, although you should use caution if it is being used along with digitalis, and at least one report recommends that it not be used along with beta blockers as it may antagonize them.
I like it that hawthorn was once considered a sacred herb. Hawthorn has long been recognized as a healer of that part of the heart that is not simply mechanical or biochemical – a healer of the spirit and soul that may reside within our hearts.
Motherwort (Leonurus cardiaca) is an excellent herb often found growing as a weed along fence rows or at the edges of lawns. Motherwort has three primary actions: as a cardiac tonic; sedative and antispasmodic; and as a tonic that helps stabilize the female reproductive tract. It is thus indicated for all heart conditions, but especially for those that are associated with anxiety and tension. It is often used to treat increased heart rates.
Motherwort has been shown to improve metabolism in the heart, reduce heart rate, increase coronary perfusion, inhibit platelet aggregation, and may cause mild hypotension. Sensitive people may develop a contact dermatitis from the plant, but other toxicities have not been reported.
If the heart is not functioning properly, fluid can build up in the lungs, causing respiratory distress. Enough of a fluid backup can cause edema (water collection at various parts of the body). Dandelion root (Taraxacum officinale) is an excellent diuretic and general tonic, and has beneficial activity for the liver and gall bladder. In animal studies, dandelion has proven to be a strong diuretic, comparable to the action of the drug, furosemide. However, while furosemide depletes potassium from the body, dandelion, with its high levels of potassium, re-supplies it naturally. Dandelion is a very safe herb to use; virtually no adverse side effects have been reported.
Cayenne (red or chili pepper, Capsicum spp.) is probably the most useful of the systemic stimulants, regulating blood flow and equalizing and strengthening the heart, arteries, capillaries, and nerves. Cayenne is a general tonic and is specific for the circulatory and digestive systems. It has the ability to balance blood pressure, correcting it to a normal range.
As a stimulant, it can be used any time an animal is debilitated – whenever the circulation is stagnant or there is congestion in the body and whenever there is a lack of energy or vitality. Cayenne is also an outstanding carrier herb, helping in the transport of other herbs and medicines to various parts of the body, but especially to the heart, stomach, and brain. Very high doses over long periods can cause internal problems such as chronic gastritis, kidney and liver disease, and neurological effects.
I find that many pets (cats included) really like food seasoned with a pinch of one of the many kinds of cayenne, and since there are at least 1,700 different pepper varieties, you should be able to fine one that your dog enjoys.
Other heart-healthy herbs to consider:
• Yarrow (Achillea millefolium) is a standard herb for treating fevers, and it is used externally as a wound-healing aid. It also lowers blood pressure and tones the blood vessels.
• Rosemary (Rosmarinus officinalis) has long been considered to be an effective memory aid, and it is used to stimulate the appetite and to promote digestion. It also stimulates blood circulation, and it is a good tonic herb for the aging dog.
• Ginkgo (Ginkgo biloba) improves brain function by enhancing blood flow to the brain, stabilizing cellular membranes, and improving oxygenation of tissues. These cell-level activities may also be directly beneficial to heart tissues.
Homeopathy and the Heart
Homeopathic remedies are used to treat the symptoms of disease, and several have been used to help with heart conditions. Crataegus may used in cases of heart weakness and also for irregular heartbeat, myocarditis, and edema. For arrhythmia Convallaria is a good choice, and for valvular disorders Adonis vernalis may be helpful. Rumex may be helpful for the long-standing heart disease in older animals, and Spongia tosta is also a good remedy for chronic cases where the respiratory pattern is gasping and violent.
Flower Essences for Heart Health
Flower essence remedies are used to alleviate emotional problems. Fix the emotions, the theory goes, and the physical problems will also clear up. Flower essences that may be beneficial for heart problems include mimulus (also a remedy to restore courage in the animal that has a fear of known things or is shy or timid); oak (the remedy that restores resilience, endurance, strength, and stamina, and is especially indicated for dogs dealing with chronic and serious heart disease); and Rescue Remedy (the emergency remedy to be used for any acute event that may be related to the heart).
Improving Matters
No matter what medical approach we take to try to help the heart patient – whether it’s Western, alternative, or a complementary mix – we may do no better than alleviating the worst of the symptoms. And if the problem is structural (a physical defect in the heart, for example), medicines will not fix the defect; the best we might accomplish is to enhance the dog’s quality of life. However, in the case of debilitating cardiac conditions, that’s a lot! As always, I suggest that guardians explore all their medical options for care and treatment of their canine companions.
YOUR DOG’S HEART HEALTH: OVERVIEW
1. Have your dogs examined by a holistic veterinarian annually. Discuss any and all nutritional supplements with him or her.
2. Make sure your dog exercises daily, for at least 20-30 minutes.
3. Feed your dog a food that contains the highest-quality protein you can afford.
4. Two words: Hawthorn tea.
Dr. Randy Kidd earned his DVM degree from Ohio State University and his PhD in Pathology/Clinical Pathology from Kansas State University. A past president of the American Holistic Veterinary Medical Association, he’s author of, Dr. Kidd’s Guide to Herbal Dog Care and, Dr. Kidd’s Guide to Herbal Cat Care.






What is your answer to this question please?
Hi. My 13yr. old 4lb. Maltese has congestive heart failure as well as a murmur. He currently takes vetmedin, furosemide,lasix. I just started him on a cbd oil. Can I give him other supplements in form of drops such as Young at heart or canine cardiac support. Not sure if these should or can be used together.Thanks for your time and help