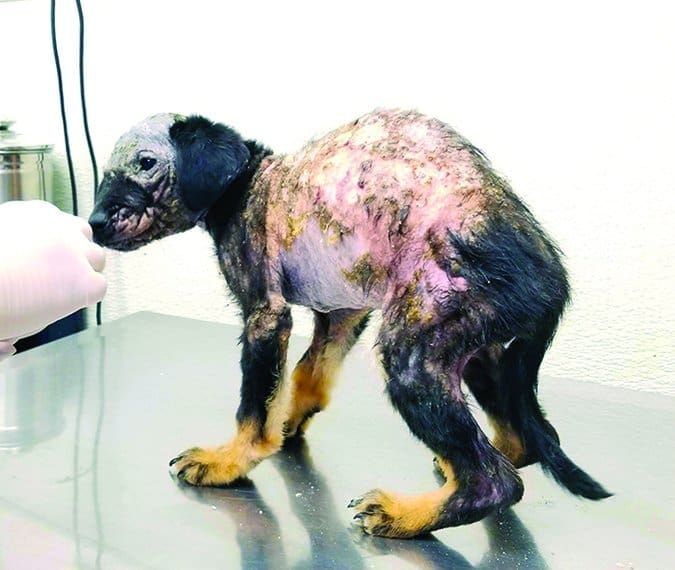
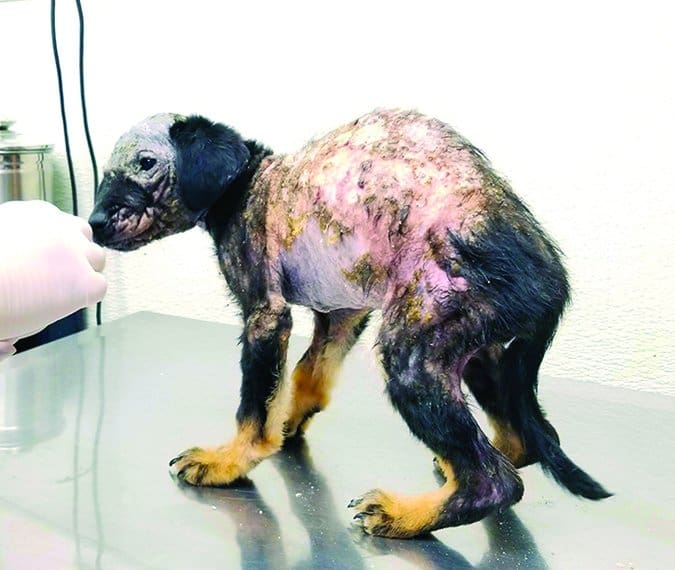
There may be no other canine malady that seems to inspire as much misinformation as canine “mange.” Internet searches often return pages that blame it on lice (wrong) as often as mites (right). Ask an older person about it and he may tell you to use a dangerous and ineffective treatment such as dousing the poor dog in used motor oil (a great way to sicken or even kill the dog). But the condition isn’t a mystery, and its treatment has never been easier. Let’s clear up the misinformation!
The term “mangy” is a general way to describe a dog who is itchy, missing hair, and has scabby, unhealthy-looking skin. Mange generally refers to one of two conditions: demodectic or sarcoptic mange, caused by two different species of mites.
Demodectic Mange
There are two types of Demodex mites that can afflict dogs: D. canis and D. injai; the former is much more prevalent. The mites are always present on dogs in low numbers as normal fauna. The skin is colonized with mites at birth, so puppies “catch” it from their mothers; it is not contagious between dogs otherwise. In a dog with a healthy immune system, the mites do not cause problems.


So, one wonders, if Demodex mites are a common and usually benign inhabitant of a dog’s skin, how does mange develop? It’s not a simple question. There are four ways to divide infestations: by age group (juvenile and adult onset) and by severity (localized and generalized).
Generalized Demodicosis
Generalized demodicosis happens when the immune system becomes suppressed and the mites proliferate out of control. This proliferation may lead to a sense of itching, causing a dog to scratch and self-traumatize. The scratching leads to breaks in the healthy skin barriers and allows bacterial and yeast infections to occur, which leads to more itching and discomfort, more self-trauma, and worsening infection and skin disease. It is a vicious cycle that can be difficult to stop.
A dog with generalized demodicosis has involvement of more than one site, an infestation that spreads, lasts for more than one to two months, or involves all four feet. The symptoms are hair loss, follicular casting (a yellowish debris is matted around the base of hairs), red bumps (called papules), and variable itching. West Highland White Terriers, Staffordshire Terriers, Shar-Pei, English Bulldogs, Boston Terriers, and several other breeds seem predisposed.
Generalized demodicosis can occur with both juveniles and adults. In puppies, there tends to be an underlying, inborn problem with the immune system. These puppies also will be susceptible to other illnesses like viral and bacterial infections.
In older dogs, another condition could trigger demodicosis. These triggers can include diseases like hypothyroidism and Cushing’s. Demodicosis can also appear if a dog has been on long-term steroids and has a weakened immune system.
In the case of generalized demodicosis, a full veterinary workup should be conducted to evaluate the dog for underlying triggers. This will include bloodwork, including a thyroid level, a urinalysis, and possibly x-rays of the chest and abdomen (in older dogs).
Localized Demodicosis
Localized demodicosis is the other possibility. These are small, well-circumscribed circular hair-loss lesions often seen on young puppies. Sometimes they are seen around the eyes. They do not tend to be itchy. These can clear on their own and often do not pose a problem. No one knows exactly why some puppies have this and others do not. It is rarer to see the localized form in adults.
Diagnosis of Demodectic Mange
The beginning of any diagnosis is a good history and physical examination. Your veterinarian will likely ask general questions about diet, exercise, vaccine history, as well as specific questions about the lesions. How long have they been present? Have they changed – smaller or larger? Do they bother your dog? Any known injuries? After a detailed history, your veterinarian will do a physical exam. This should include a nose-to-tail assessment including vitals and weight.
Once this is accomplished, the vet will gather samples. These will usually include a skin scrape, tape preparation, and impression smears.
In the first, a dull scalpel blade is used to scrape the edges of the lesions until a thin scrim of blood is noted. It is important to get a little bit of blood, as the mites can be deep in the hair follicles. This sample will be placed on a microscope slide with mineral oil and examined under a microscope at low magnification power.
The mites are usually easily visible. Demodex mites are long and cigar-shaped with six legs.
Your veterinarian should also place a strip of clear acetate tape over the lesions and press microscope slides directly onto the affected areas. These samples are stained and examined at high power. She will also look for evidence of secondary bacterial and/or yeast infections that must also be treated.
Sarcoptic Mange
Unlike Demodex, Sarcoptes is not normally found on dogs. This is a contagious mite that spreads from dog to dog. It can also spread from dogs to people, though it will not live long on humans. The most common Sarcoptes mite that afflicts dogs is S. scabiei.
Sarcoptic mange (often called scabies) is intensely itchy and uncomfortable for dogs. Dogs will dig and scratch at themselves, particularly on the sparsely haired areas of the body. These dogs are often in misery. The skin will be red and crusty around the elbows, base of the ears, belly, and outside of the knee. Secondary skin infections are extremely common. As with Demodex, in some cases, the skin infections are so bad that the lymph nodes become enlarged, and the dog may become depressed, lethargic, develop a fever, and lose appetite. No breed seems particularly predisposed.

Scabies may also be diagnosed if the humans living in the house with the affected dog(s) start itching! While canine Sarcoptes lives only transiently on humans, it can cause intense itching and red papules on the skin. These show up along the waistline, neck, and arms. It can occur within 24 hours of exposure and last for up to three weeks. Usually within one to two weeks, the lesions will resolve, as long as the dog is treated successfully and re-exposure does not occur.
Diagnosis of Sarcoptic Mange
The tests are the same as for Demodex, but Sarcoptes mites live very deep and can be difficult to find. Under the microscope, Sarcoptes mites are fat, round mites with six legs on the juveniles and eight on the adults.
Your veterinarian may scrape in four or five places in an attempt to locate just one mite and will also look for mite eggs. The absence of mites on a skin scrape does not rule out scabies. If your veterinarian is very suspicious, and the skin scrape is negative, she may scratch behind your dog’s ears. A response of thumping of the leg on the same side is called a “positive pinnal-pedal reflex.” While it is not specific for scabies, it is one sign that, paired with the other symptoms mentioned above, makes scabies a likely diagnosis.
What to Do About Mange on Dogs
Until fairly recently, treatment for both types of mite infestations was extensive and involved repeated use of lime-sulfur shampoos and/or dips (every five to seven days, for as long as it takes for the lesions to heal) and ivermectin. The dips are effective treatments, but they are time-consuming, hideously smelly, and carry other risks.
These treatments have been largely supplanted by a new class of chemicals called isoxazolines. These include the oral medications sold under the names Bravecto, Credelio, NexGard, and Simparica; Bravecto is also available as a topical “spot-on” treatment. These medications were all developed to treat infestations of fleas and ticks, but have proven to be so effective at killing mites, that most veterinarians are now using them “off-label” as their go-to treatment for mites. On-label use is expected within the next year.
If the affected dog is young and the lesions are minor, a one-time treatment with one of the isoxazoline drugs will likely be sufficient. In cases of generalized demodicosis, the dog may require another dose or two, given a month apart.
Concerns About Isoxazolines
You may have recently seen FDA warnings about the isoxazoline drugs. There have been reports of serious adverse effects, such as seizures, that may result from their use. The drugs are safe to use in the vast majority of patients, but the cases of adverse effects cannot and should not be dismissed.
As with any medication, it is important to review your dog’s medical history with your veterinarian. If there is history of neurological disease or seizures, the risks, benefits, and disadvantages of an isoxazoline drug should be weighed against those of different medications, such as (in this case) lime-sulfur dips and ivermectin.
There are many alternatives to these drugs for flea and tick control – and many pose less-serious potential adverse effects. But nothing beats the efficacy of the isoxazoline drugs for treating the mites that cause canine mange. Dog owners should be advised of the risks and advantages of using these drugs as well as the older alternatives.
While the primary treatment is focused on getting rid of the mite overgrowth, secondary skin infections must also be treated. These infections can be bacterial, fungal (yeast), or a combination of both. The samples your veterinarian took will help determine what treatment is needed.
Antibiotic resistance in veterinary medicine is becoming a significant problem. Many times, skin infections (yeast and bacterial both) can be treated with topical medications before oral medications. There are many different products such as mousses, wipes, and shampoos on the market. Type and availability will vary among veterinary offices. Topical therapy should be tried first to avoid encouraging antibiotic resistance. This will be done in conjunction with treatment of the mites with an isoxazoline and/or lime-sulfur dips.
If topical treatment fails for the infections (called pyoderma), oral therapy is next. This can include a combination of antibiotics like the cephalosporin class and oral antifungal drugs such as ketoconazole.
If first-line oral therapies do not treat the skin infections, then your veterinarian will likely recommend a culture of the skin to determine which antibiotic is most appropriate. This is becoming increasingly common as overuse of antibiotics is rampant in both human and veterinary medicine.
Once the mites begin to die (particularly with Sarcoptes), the itching may dramatically intensify. Using steroids (such as prednisone) in dogs with mite infestations is not a great idea, as this suppresses the immune system further. If the itching is intolerable and causing a dog to severely self-traumatize, then a very low dose of prednisone may be prescribed for a short course.
Since sarcoptic mange is contagious, all dogs who came into contact with an affected dog should be treated for the mites.
Your veterinarian may repeat skin scrapings after treatment, to make sure the mite overgrowth has been controlled, but given the effectiveness of the isoxazolines, this isn’t usually done anymore. Improvement in clinical symptoms is generally proof of successful treatment.
Mites are host-specific and do not live off of their preferred hosts for long. Still, it’s never a bad idea to wash your dog’s bedding, especially if she has skin infections and itching. It’s also a good approach to wash your dog’s combs, brushes, and collars.
Catherine Ashe, DVM, graduated the University of Tennessee College of Veterinary Medicine in 2008. She practiced ER medicine for nine years and now works as a relief veterinarian in Asheville, North Carolina.