Heartworms are horrible. No arguments there. Anyone who has ever known or had an infected dog knows how slowly but surely the parasites can sap the animal’s strength and vitality. Going through the treatment to kill the heartworm is no walk in the park either. The “cure” is quite capable of killing the dog in the process of trying to save its life.
But some people just don’t like the idea of giving the dog the chemical preventatives that can keep the pooch safe from infestation. And some dogs are sensitive to the drugs, reacting to each dose with vomiting, diarrhea, and other symptoms.
Heartworm is one of those health issues where an aggressive approach – traditional or alternative – is needed to save the dog. But the most effective approach to prevention and/or treatment combines the best of both veterinary worlds.
Elaborate Life
The life cycle of this insidious killer is complex, requiring two hosts – a dog and a mosquito. The heartworm’s life starts out in a dog, shifts to a mosquito for a short time, and then ends back in a dog. It’s a fascinating and deadly journey.
Living in a dog’s pulmonary arteries, adult female worms mate with males. Shortly thereafter, the females produce thousands of infinitesimally small “babies,” each less than 1/800 of an inch.
At this stage, the baby heartworms are called microfilariae (from the Greek word mikros, small, and Latin filum, thread). The microfilariae can circulate in the dog’s bloodstream for as long as two years. Scientists do not attribute any particular health problems to the presence of the microfilariae, even though the density of the microfilariae can increase over time if the parents are allowed to thrive. Veterinarians can see as many as 10-15 microfilariae in a single drop of blood from an infested dog; if you do the math, it works out to about 200,000 microfilariae circulating through an average 50-pound dog.
As ominous as this sounds, without a mosquito to carry them off to their next life stage, these microfilariae cannot develop further. If you could keep mosquitoes away from the dog for the rest of his life, the heartworm would progress no further.
Unfortunately, the world is full of mosquitoes. When one bites an infected dog, it can’t help but to ingest a couple of microfilariae with its blood meal. Inside the mosquito, the microfilariae continue their development, shortening and thickening into the first of several larval forms. It takes them two to three weeks to molt twice (going through what are called the L1 and L2 stages) and reach a form (L3) that will carry them back out of the mosquito into another dog. They can not develop further without another dog.
The larvae then move to the mosquito’s mouth, positioning themselves for their next move. When the mosquito bites another dog, the larvae are deposited onto the dog’s skin. After the mosquito withdraws, the larvae crawl into the tiny bite wound, and take up residence in the dog’s subcutaneous tissues.
The (L3) larvae spend the first week or two molting again, before taking a form (L4) that will enable them to migrate through the dog’s subcutaneous and muscle tissue. They take another 40 to 60 days journeying toward the dog’s upper abdomen and thoracic cavity. When they get about 1/10 of an inch long, they penetrate the dog’s veins and make their way to the right side of the heart, where they become full-fledged adults.
Up until this stage, a newly-infected dog shows no sign of disease. It’s only after the worms grow to adult sizes that the dog’s disease process starts. It can take a minimum of six months to more than a year from when he is first bitten by the infected mosquito for the dog to show visible signs of the infection.
Adults Only
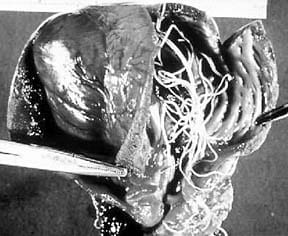
Once they are adults, heartworms are restricted by their size from circulating everywhere through the dog’s circulatory system, but they still get around. Their preferred site is the right heart and pulmonary arteries, but they can also lodge in the veins of the liver and veins entering the heart. Very occasionally, they take up residence in other sites, such as the eye, the cerebral arteries, or the systemic arteries in the rear legs. (Worms in those sites must be treated surgically.) As they feed on nutrients they draw from the dog’s blood and tissue, they can grow to an astonishing 14 inches. Physically, their most damaging activity is the obstruction and interference with the performance of the heart valves and pulmonary arteries.
If the dog is host to enough worms, they can cause what is known as Caval Syndrome. By literally packing the right side of the heart, they cause an increase in the venous pressure in the liver, which damages the liver tissue. The liver dysfunction, in turn, changes the quality of the red blood cells the body produces, leading to a number of blood disorders. Eventually the system fails, manifesting itself in a sudden and dramatic collapse of the dog. Oddly, not all dogs with untreated heartworm develop Caval Syndrome, and the ones that do are usually younger, from three to five years.
How much damage the worms do depends on several factors, most importantly, the number of adult worms in the dog’s body and the dog’s activity level. Sedentary dogs with 25 or fewer worms may never show signs of the disease. Active dogs with the same number, or dogs that host 50-100 worms will exhibit moderate to severe heartworm disease.
Interestingly, the immune systems of some dogs are able to wage war, to a limited extent, on the heartworm cycle. An immune mediated response is thought to be responsible for some dogs ability to remove microfilariae from their circulatory system. Though the dog’s system has not displayed the ability to damage or dislodge adult worms, an otherwise very healthy dog may be able to outlive the worms, which can survive in the heart for five to seven years.
Pet Detecting
The tests that can detect canine heartworm have increased in sophistication. Nevertheless, it takes two tests to make an accurate diagnosis.
The earliest test used for this purpose, called a Knott’s test or a Filter test, consists of a simple examination of the dog’s blood under a microscope, and is still used today to detect the presence of the microfilariae. If these are seen, it indicates the dog currently hosts an adult population of the worms.
But a dog with no visible (through a microscope) microfilariae can still have heartworms. This condition is called “occult dirofilariasis,” and it could mean:
• He is hosting a population of adults that are all male or all female, and thus, not producing any babies.
• He is hosting a population of adults that have been rendered sterile through the use of Ivermectin or other preventative drugs, and thus are not producing any babies.
• He is hosting a reproducing adult population, but his immune system is successfully waging a war on the circulating microfilariae, efficiently removing them from his blood.
• The heartworms he is hosting are not yet adults. The second blood test used to diagnose heartworm infestation zeroes in on the adult population. The earliest test used for this purpose worked by detecting the antigens (foreign proteins) shed by adult heartworms. The problem was, it could only indicate whether adults had ever been in the dog’s system. It would detect antigens even if the worms were dead and gone.
The adult detection test used today has a similar fault. It detects only the antigens produced by live, adult females, so it can miss all-male adult infestations, or juvenile females. If the dog was bitten by an infected mosquito only in the last six months, the test will not detect the juveniles.
Traditional Treatments
The traditional path to full treatment is long and arduous – but far preferable to the longer and more arduous death by heartworm. Because the heartworm lives in the dog in three distinctly different forms – microfilariae, larvae, and adult worm – three different drugs, administered in separate stages, have to be employed to rid the dog of the invader.
The first step is to get rid of the adults, which cause the most damage. Just a couple of years ago, there was only one option for this treatment, an intravenous injection of an arsenic-based drug called Caparsolate. The treatment is essentially chemotherapy, the administration of a deadly drug that is supposed to be deadlier to the parasite than it is to the patient. The drug required two injections of the drug for two days, and each injection was a hold-your-breath endeavor. Caparsolate had to be injected directly into the dog’s veins, and if even a minute amount came in contact with muscle or other tissue, it caused horrible wounds accompanied by massive tissue sloughing.
In 1995, a company called Rhone-Merieaux introduced Immiticide, a much better drug, and it quickly replaced Caparsolate as the treatment of choice. Another deadly and powerful drug, it, too, presents veterinarians with some challenges, but compared to the alternative, most veterinarians feel it is light years better. The current maker of Immiticide is Merial Limited, a company that was born of a merger between Rhone-Merieaux and Merck, and is based in Iselin, New Jersey.
The two injections that are required for a complete Immiticide treatment are usually administered 24 hours apart, in a very specific site rarely used for injections: deep in the back muscles located above the L3 and L5 lumbar vertebrae. Immiticide does not cause tissue sloughing, but many dogs exhibit irritation at the injection site, including pain, swelling, and reluctance to move.
The dog’s post-treatment symptoms are similar with both the old and the new treatment. The drugs kill the worms, leaving the dog’s body to carry the dead and decaying worms out of its circulatory system. The dead worms are carried in the bloodstream to the lungs, where they are gradually reabsorbed. Depending on the dog’s health and the total number of worms in his system, this can be a mild or a violent process. The dogs usually cough, gag, and vomit, experience fever and lung congestion, and are understandably depressed and lethargic.
Both treatments require the dog to be kept as quiet as possible (preferably caged) for the first few days. All increases in heart rate and respiration force a greater amount of dead worm fragments into circulation. If too many particles flood into the lungs at once, they can block the blood vessels to the lungs and cause death. Following a treatment with Caparsolate, veterinarians recommend the dog be kept physically restricted for one to two months. This restriction is shorter following Immiticide treatment.
Ten to 20 percent of dogs with a high worm burden will die as a result of the Immiticide treatment. (The number seems grim until you consider that even without treatment, dogs with that level of infestation suffer a much slower, progressively debilitating death.) If a heart X-ray, antigen test, or the dog’s symptoms suggest that the infestation is very severe, the dogs can undergo a modified treatment protocol, consisting of a single injection, which kills the weaker worms, followed by two more injections a month later. The cost for the entire treatment depends largely on how the dog reacts to the drugs and to the death of the worms. For most lightly infested dogs, the experience totals a week or two of discomfort with no further veterinary treatment required. Under these circumstances, the bill from the veterinary hospital would average $400-600. A dog that experienced difficulties, however, may required extended veterinary care, including administrations of fluids, steroids to reduce any fever or inflammation and help quell the coughing, and supportive therapies for the liver. In this case, the bill can easily reach upwards of $1,500.
Both the Immiticide and the Caparsolate treatments are contraindicated (not recommended) for the most severely infested dogs with Caval syndrome. After the adults are killed, the next step in traditional treatment is to kill any microfilariae that are still in circulation. Since the microfilariae cannot mature without an intermediate host (time spent in a mosquito), you’d think you could skip this step. But you have to administer yet another drug to kill any larvae that may have been deposited on the dog in the last 60 days, and the drugs used for that purpose also kill the microfilariae at a dangerous rate. (A too-sudden die-off of the microfilariae can cause shock and subsequent death of the dog.) The drug used to kill the microfilariae, dithiazanine iodide, is given orally until the microfilariae are absent from the blood, usually one to two weeks.
Final Step – Should Have Been the First
It’s only at this point that you can administer the final treatment – the one the dog should have received before he ever came in contact with mosquitoes. The drugs used halt the development of any larvae present in the dog’s tissues. They comprise the “preventative” action that should be used for the rest of the dog’s life. Each drug costs about $30-40 for a six-month supply. Currently there are three types of drugs available for preventing heartworm development in dogs. The first drug used to prevent larval development was diethylcarbamazine (DEC), marketed as Filaribits, Dec-acide, Caricide, and Hetrazan. DEC is still used, but it must be given to dogs daily throughout the mosquito season, since it kills only the L3 larvae which have not yet taken L4 form, a process the larvae undergo within the first 36 hours on the dog.
Today, DEC is used less frequently than the newer, once-a-month products Interceptor, HeartGard-30, and Sentinel. Interceptor was the first of the monthly preventatives, introduced to the market in 1993 by Novartis Animal Health. The active ingredient in this drug is milbemycin oxime, which kills the L3 and L4 stage heartworms as well as other intestinal parasites such as hookworm, whipworm, and roundworm.
Novartis also makes Program, an oral insect development inhibitor (IDI) made available in 1994 for the purpose of killing fleas. In 1997, the company brought out a combination of lufenuron and milbemycin oxime that they call Sentinel.
Perhaps the best known monthly preventative, however, is HeartGard-30. An Ivermectin-based drug, HeartGard received an early reputation for being poorly tolerated by Collies and other particularly chemical-sensitive dogs. Recent dosages seem to have corrected the problems, which usually manifested as vomiting, diarrhea, depression, and/or a lack of appetite.
HeartGard, Sentinel, and Interceptor are approved only for use as anti-larval drugs, but each has been used on dogs hosting a population of adult heartworms with mixed results. The danger is that these drugs can kill the population of microfilariae so rapidly that embolism (an obstruction of the arteries) occurs. Also, while neither drug has demonstrated an ability to kill the adults worms, it may have a sterilizing effect on them, keeping them from producing any more microfilariae. With only a light infestation, protected from further infestation by the anti-larval drugs, a dog could conceivably outlive the heartworms.
Alternative Approaches
So far, we have discussed only the traditional veterinary approach to heartworm prevention and treatment. Due to the seriousness of the disease, most holistic practitioners recommend that their clients use the traditional drugs. Some use herbal or homeopathic remedies to support and help the dog’s body deal with the chemical treatments. Some, however, use only alternative methods to protect their own dogs’ health, and most are happy to help and support a client who wants to do the same. But the completely drug-free approach requires a huge commitment from dog owners, and unless owners devote themselves completely to the task of building and maintaining their dogs’ immune systems, they may find their dogs infected after all.
WDJ interviewed three holistic veterinarians with a wide range of experiences with non-traditional and traditional heartworm prevention and treatment. All three agree that keeping the dog healthy in order to boost his own immune system response to heartworm infections is critical (for more information about this process, see Dr. Christina Chambreau’s article, “Five Steps to Fitness,” in the April 1998 issue of WDJ). But each has taken a very different approach to the heartworm problem.
California veterinarian Nancy Scanlan says she is lucky; none of her clients have ever had a heartworm positive dog. There is heartworm in California, however, and she advises most of her clients to use the traditional drugs for preventing infection. However, she suggests also using herbal, homeopathic, and nutritional supplements to help the body detoxify after preventative use.
Representing the middle ground, Indiana veterinarian Carolyn Blakey supports those of her clients who use traditional drugs as well as those who take a completely alternative approach to prevention and treatment. She has seen success with both approaches, she says, attributing that achievement to the homeopathic remedies and nutritional supplements she administers to improve the dogs’ circulatory function.
And on the far left, Texas veterinarian William Falconer says he provides a fully homeopathic alternative to the traditional drugs for heartworm. This means a totally unique constitutional remedy tailored to each individual dog, an approach he claims has enjoyed 100 percent success.
We’ll describe each practitioner’s approach in the next issue.
-By Nancy Kerns
We would like to thank Nancy Scanlan, DVM, of Sherman Oaks, CA, William Falconer, DVM, of Austin TX, and Carolyn Blakey, DVM, of Richmond, IN for their help with this article.





