If you live in or travel to the Southwest, particularly Texas, California, or Arizona, it is important that you know about a fungal infection called coccidioidomycosis. It is also known as San Joaquin Fever or Valley Fever (VF). This fungus can pose a significant threat to our canine companions, as well as to their human counterparts. There are two well-known species Coccidioides immitis and C. posadasii.
Coccidioides species are a hardy fungus that live in the soil. The dry, hot atmosphere of the Sonoran life zone are perfect for it. High winds, dust storms, and earthquakes encourage the release and spread of spores. Infection occurs when the spores (called arthroconidia) are inhaled. Lung disease develops and then spreads throughout the body to the lymph nodes and organs. Every system from the brain, skin, eyes, and bones can be involved. This is known as systemic or disseminated infection. Coccidioidomycosis can be a devastating disease. It is important to know the progression, symptoms, and treatment for this condition.
Valley Fever typically incubates in the body for one to three weeks, but it can lie dormant for years before symptoms develop. This makes it absolutely critical to always let your veterinarian know any travel history (including if your dog was adopted from another area of the United States). It may not seem like important information, but it could be life-saving.

Research indicates that most dogs living in endemic areas are exposed to Coccidioides species and clear the infection without significant illness. They may develop mild respiratory disease from which they recover without specific treatment. A 2005 study showed that outdoor dogs were about five times more likely to contract this condition than indoor pets. Another study showed that dogs with greater than one acre of land on which to roam were at increased risk. Walking dogs on a sidewalk was protective.
Life Cycle
In the desert, Coccidioides species exist as a mold. The mold is in long, partitioned chains called hyphae. These fragment into tiny, individual arthroconidia, which are aerosolized under the right conditions (hot, dry, and windy) and inhaled by hosts including dogs, cats, and humans, settling in the lungs.
This new environment induces them to undergo a change. They turn into spherules that fill with endospores. Once full, the spherules rupture and release the spores into surrounding tissue. The endospores can then turn into spherules themselves and propagate the infection. This is why every system in the body can be involved.
Symptoms
The associated symptoms are seen in every system from the brain to the bones. Initially, the fungus replicates in the lungs, leading to pulmonary disease. In cases where the disease does not spread beyond the lungs, the infection is considered to be localized. It can be mild or develop into pneumonia. Once the infection spreads beyond the lungs and infects other systems, it becomes disseminated.
The most common initial symptoms are lack of appetite, weight loss, malaise, fever, and limping. The limping may shift from leg to leg. These are non-specific signs and can be seen with other fungal infections such as blastomycosis, histoplasmosis, tick-borne diseases like Ehrlichia and Rocky Mountain spotted fever, and bone cancers such as osteosarcoma.
The following organ changes can be seen:
- Lungs. As mentioned above, a fungal infection in the lungs can cause pulmonary disease and pneumonia.
- Central nervous system (brain/spinal cord). Coccidioides in the central nervous system can lead to seizures, behavioral changes, and lethargy.
- Ocular. Uveitis is common with VF. The spores replicate in the eye tissue causing marked inflammation and discomfort. Outwardly, you may notice a whitish or reddish haze over your dog’s eye, the white of the eye (sclera) may appear red, and weeping may occur. The eye may appear sunken/smaller than normal.
- Bones. Valley Fever is particularly damaging to the bones. Osteomyelitis (destruction of the bone as a result of the spores and inflammation) can occur. It typically occurs in the long bones (the limbs), but it can affect any bone in the body. Radiographs (x-rays) usually reveal a destructive lesion and a periosteal reaction – when the bone begins to try to heal the lesion by producing more bone.
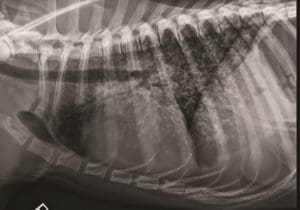
It is impossible to differentiate between metastatic cancer and Valley Fever changes on x-rays, so this is when travel history, further diagnostic testing, and other information such as signalment (age and breed) become absolutely essential.
- Cardiac. Coccidioides can affect the heart tissue, leading to pericarditis, a generalized term for inflammation of the heart muscle. It can also cause an accumulation of fluid in the pericardium (the sac around the heart). This is called pericardial effusion. It can cause heart failure quickly because the heart cannot contract properly.
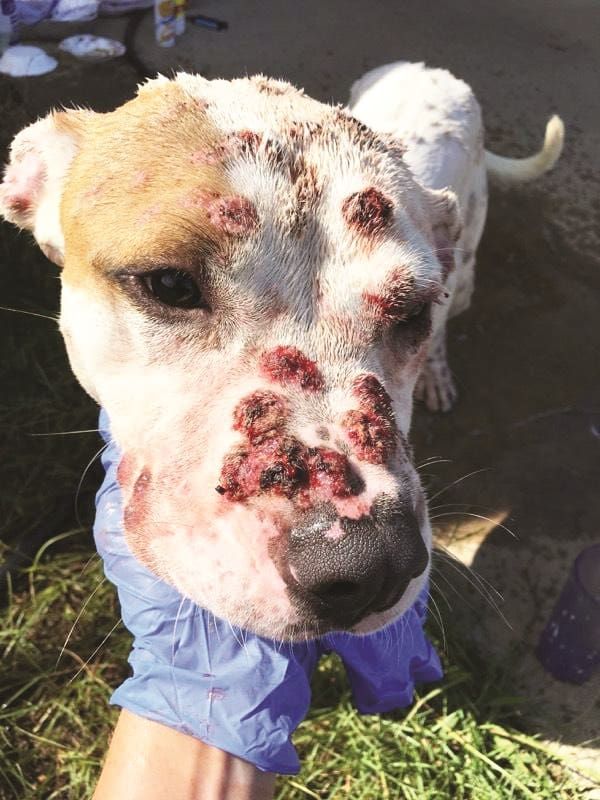
- Skin. Skin lesions are common with Valley Fever. These can look like open, weeping sores and bumps. They may form anywhere on the body. There may be many or a few.
- Liver and kidney. Outward symptoms of liver problems caused by Valley Fever can include jaundice (yellow tint to the skin), abdominal distention, and vomiting; symptoms of kidney problems can include increased drinking and urinating.
Diagnosis
Like many things with Valley Fever, diagnosis isn’t straightforward. Any time a patient presents with signs of significant illness, the first step in determining the cause is a thorough physical exam and history; the latter should always include any travel and adoption/purchase history.
A physical examination should proceed in a systematic manner from nose to tail. This exam should include full vitals, including weight and temperature.
Once these are accomplished, a “minimum database” – a set of tests that will provide the doctor with enough information to get him on the right track – is usually recommended. This generally includes a complete blood count (CBC), chemistry panel, and urinalysis. A complete blood count evaluates the red blood cell, white blood cell, and platelet counts, as well as whether the cells are normal in size and morphology.
In dogs with coccidioidomycosis, blood work changes can include anemia, elevated white blood cells, and low platelets. These findings indicate systemic inflammation and infection but are not specific to Valley Fever. A chemistry panel may show low albumin, an important carrier protein, elevated globulins (proteins that fight infection), and alterations in liver and kidney values, if those organs are involved. Again, these findings are not specific to Valley Fever.
If limping or coughing is present, x-rays are usually recommended. Both the lungs and bones can have marked changes that are very difficult to differentiate from cancer. In the lungs, large, “fluffy” infiltrates can be seen. It is often described as a snowstorm pattern. Again, these look very similar to cancer. The lymph nodes in the chest may also be enlarged (called perihilar lymphadenomegaly). Again, this can be caused by both fungal disease and cancer. In the bones, the changes may include destruction of the bone cortex with extra bone proliferation as discussed above.
Urinalysis may showed elevated protein in the urine, but as with blood tests, this is very non-specific.
As a result, if your veterinarian suspects Valley Fever, more specific testing needs to be conducted to make this diagnosis.
If draining skin lesions are present, your veterinarian may take impression smears and aspirates. This is relatively simple and non-invasive. A microscope slide can be pressed directly onto skin lesions that are oozing. A small needle can also be introduced and a sample taken (called a fine needle aspirate or FNA). Sometimes, the actual Coccidioides spores can be seen in these samples, along with severe inflammation.
If bone involvement is present, aspirates or biopsies of the bone can be taken and submitted to a pathologist. This is more invasive than a skin FNA and can be painful, so it should be done under sedation or anesthesia. Bones affected with Valley Fever are weakened and at risk for fracture during this procedure. They may also fracture with normal activity such as walking and running. This is called a pathologic fracture.
A fungal culture can also be done. This is when the fungus is grown on a culture medium. Ironically, Coccidioides can be difficult to grow in the lab, and this test can take up to two weeks to indicate a positive result. As a result, it is not the most useful test when trying to make a rapid diagnosis. Since Coccidioides is contagious to people, it must be grown in a specialized, biohazard laboratory. It is rarely utilized for diagnosis.
Antibodies
Serologic testing is more specific for Coccidioides. Serologic testing evaluates for the presence of antibodies produced by the immune system. Antibody production is a complex process, but it is fascinating.
Any time a dog is exposed to an attacker like a fungus, the immune system responds quickly. Because the offending organism is not from the body, it lacks familiar markers on the cell surfaces. The immune system recognizes this and attacks. Two particular cells are very important. B-cells attack the fungus directly by coating it with antibodies and preventing replication. It also tags the fungal bodies so that other immune system cells will recognize and destroy them.
Antigen-presenting cells (APCs) and T-cells are also important. APCs break up the organism and then show the fragments to the T-cells, which then destroy them. After the threat has been neutralized, most of the immune cells disappear. The only exception is memory cells, which hang around. These help the immune system respond much faster the next time this organism is encountered.

Serologic testing takes advantage of our understanding of this process. Your veterinarian will submit a blood sample to a laboratory that can search for antibodies that are specific for Coccidioides. The earliest antibodies produced are called immunoglobulin M (IgM). These are found at high levels in blood and lymph and respond earliest and fastest to infections. The results are reported as a ratio.
A ratio of greater than 1:8 is considered evidence of infection. A ratio that is greater than 1:32 likely indicates an active, systemic infection. IgM levels rise within two to four weeks of exposure and then quickly wane. They can be gone by four weeks.
Immunoglobulin G (IgG) is the second responding immunoglobulin and will last longer than IgM –sometimes, it’s detectable for years after infection. Often veterinarians recommend “paired” titers in which an early sample is taken, and then another is taken two weeks later to evaluate how the immune system is responding. This can also indicate active infection. Oddly enough, it is not always clear cut. Dogs have can negative titers (the immune system doesn’t react) and still be infected. They can also have high titers with a relatively mild infection. This is part of what makes the diagnosis of this fungal invader so tricky.
Titer tests for antibodies formed in response to Coccidioides are not 100% accurate. No test is. Other options include the EIA (antibody enzyme immunoassay) from MiraVista Diagnostics. This can be conducted on samples as varied as cerebrospinal fluid and urine. Unfortunately, it cross reacts with other fungal infections like blastomycosis and histoplasmosis, which also have similar symptoms, so an exact diagnosis may not be possible. This is when the dog’s travel history becomes critical.
Treatment
Antifungal drugs are used to target the Coccidioides fungus specifically. While antifungals are often very effective, they can cause side effects, such as loss of appetite, vomiting, lethargy, and increased liver enzymes. The drugs that are most commonly used to treat VF are:
- Itraconazole. This medicine is considered the drug of choice. It’s a good bit more expensive than the second-best drug, however.
- Ketoconazole. Usually the most cost-effective treatment choice. Treatment is generally a minimum of three months and at least two months beyond the resolution of obvious symptoms. With extended therapy, it can cause cataract formation.
- Fluconazole. Studies on the efficacy of this drug for Coccidioidomycosis are lacking, but if other drugs fail, it is an option.
- Amphotericin B. This drug is often used as a last resort in cases when the other drugs listed were ineffective.
For dogs with systemic involvement, therapy must also be targeted at the affected organs.
In dogs with severe lung disease, treatment may involve hospitalization for oxygen therapy, intravenous (IV) fluids to maintain hydration, IV antibiotics to combat secondary bacterial infections, steroids to minimize inflammation secondary to fungal die-off (this may occurs when antifungals are given and incite an overwhelming inflammation response in the lungs).
In dogs with bone involvement, therapy must sometimes be very aggressive. If the fungus has destroyed bone enough to lead to pathologic fractures, amputation may be the only option. In cases where the bone is damaged but not destroyed, the lesions will sometimes improve with antifungal treatment, as the body regenerates the damaged bone.
In cases of ocular involvement with uveitis, prognosis for vision is guarded. Antifungals do not penetrate into eye tissue very well, and the eyes can serve as a permanent nidus for infection. This is painful. In these cases, enucleation (removal of the affected eye or eyes) is often the only way to rid the body of Coccidioidomycosis.
Prognosis
In cases where only the lungs are involved (localized infection), response rates to therapy are as high as 90%. When other systems are involved, the prognosis drops to around 60%. Response to therapy is dependent on each dog’s immune system and can be very hard to predict. The prognosis is worse if multiple bones and/or the central nervous system are involved.
Once treatment is discontinued, Valley Fever can recur. It is very hard to kill the organism entirely and reports of recurrence years later and in different body systems are common.






Gosh it sounds as though denise follows the same principals as our President and his ill informed recommendation of Hydroxychoraquin! Science is NOT A MATTER OF OPINION. The facts matter. Doxycycline is an antibacterial not an antifungal.
Apparently people commenting have a reading comprehension problem. I never wrote that anti fungal drugs weren’t appropriate – they are. I simply said a lesser expensive drug, Doxycycline, was not mentioned. And while it isn’t an anti-fungal drug it has worked rather well in some dogs. Everyone is entitled to their opinion and that includes me. But I am not a fan of WDJ and I believe it prints misleading information; while someone posted here that the photo of the dog with lesions wasn’t Judd the caption certainly inferred it was. I stand by what I said and don’t for a minute believe my comments were “ungracious {Ehh}.” And I would not want “Roni” for a nurse because I never suggested strictly going to a vet who practices wholistic veterinary medicine. Do you people even read before you post? This forum is for education. If you want to be fed pablum by WDJ then by all means never question it.
Of course your entitled to your opinion. However, I strongly disagree with your assessment of WDJ. They are a relatively small operation/publication who aren’t biased by advertising money—which is nearly non-existent in these times. They need our support and I hope you’ll re-evaluate & reconsider.
🐾🐶🐾
I have a couple of questions since I hae never heard of Valley Fever before. Is it contagious from dog to dog ?
From dog to people? Or dog to Horse ? As in can a person have been exposed and then sneeze on the dog ( or visa versa ) and expose the recieving to Valley Fever ? Being that it could be in the lungs. ( As in Kennel cough.) As far as Western or Eastern Medicine goes I think it is a personal decision BUT all options should be listened to with a open mind. Then make a TRUELY educated decision. Thank you to Stacy and the WDJ for sharing the story of Judd and ALL the other info that gets passed to us so we can use the information to help us ask the questions to our vet so we CAN make a educated decision.
Hi Cheryl,
It’s not contagious. I totally support and utilize holistic medicine. However, if your pet or human has this disease, they need an antifungal drug. There are 3 commonly utilized: itraconazole, fluconazole and ketaconazole. My dog couldn’t tolerate fluconazole and was put on itraconazole. I am utilizing probiotics and K-9 immune support (mushrooms) as well as Denamarin (Sam-E and Milk Thistle) to support his recovery. When my cat had it, the fluconazole really upset his stomach. He had acupuncture and it greatly helped with nausea. He was a strictly indoor cat. The disease was airborne. He would sit by a screen door. It’s a nasty disease. Knowledge is power. The story needs to be told.
Thank you Mary
I agree with Ehh, Susan B Hayes and Betty Meadows regarding Denise Boggs. I am a Registered Nurse and the thought of people going strictly to people who practice Holistic Medicine and not Medical Drs., or Nurse Practioners or PA’s or taking our best friends to Veterinarians is thoughtless and foolish. We have medications for a reason and if you believe in not taking medications that can cure diseases, you take your chances with those diseases. The Whole Dog Journal is a magazine that gives people choices. Take it or leave it.
@Denise Boggs: You have misunderstood. The dog with lesions—read the caption—is not Judd; the photo of Judd is with his award ribbon. You wrote “one look at Judd and I thought ‘I have never seen a dog with Valley Fever with these types of lesions.’” (And might you consider that something is possible even if you haven’t seen it before?) The article does describe how diagnosis is difficult and that symptoms overlap with other diseases. Why are you so ungracious?