At this time last year I didn’t know stem cell therapy for animals was a thing. While searching for a job where I could use my biology background and love of animals, I found a posting for a stem cell technician at a local veterinarian’s office. I got the job! – and have found that there are few things as thrilling as having a part in changing a dog who had been in so much pain she could hardly move to become one who’s able to trot around and enjoy life again.
Stem cell therapy is a powerful tool in treating degenerative or other diseases as well as injury. It’s an effective way to regenerate damaged or diseased tissue using cells from the dog’s own body. It was first used in a veterinary context in 2002 for tendon and ligament repair for horses.1 Since severe leg injuries can be detrimental for horses, particularly for those involved in sports of racing and jumping, stem cell therapy was a game changer. The results were remarkable – most of the treated horses were able to return to their previous activity.
Eventually stem cell therapy was utilized in treating companion animals, primarily for the same issues of tendon or ligament repair but has largely become focused on arthritis. While not a cure-all, stem cell therapy is a low-risk approach to treating injuries and degenerative diseases, providing our dogs with a better quality of life without dependence on medications.
STEM CELL BASICS
What is a stem cell? It’s not quite as simple a question as it sounds. There are different types of stem cells, but the first main characteristic of a stem cell (SC) is that it can become one of a number of different cell types (called differentiation), giving rise to different tissues. Stem cells are also very proliferative, meaning they quickly divide and produce more cells, but at varying rates depending on the type of SC.
There is a difference between embryonic and adult stem cells. Embryonic stem cells (ESCs) are responsible for embryonic development. They are pluripotent, which means they can develop into any type of cell in the adult body. And they are vastly proliferative, more so than adult SCs. ESCs do not exist in the organism after birth.
An embryo develops from a single cell into a complex organism composed of multiple tissues. The course of development involves many stages, but in short, a few cells proliferate and eventually develop specialized cells that compose all the various tissues of the body. ESCs in the early embryo proliferate, or divide, to produce more cells very quickly. They are pluripotent, which means they are capable of becoming any cell type in the organism. As development proceeds cells eventually become more specialized and less proliferative. There are many stages or levels as SCs move toward specialization.
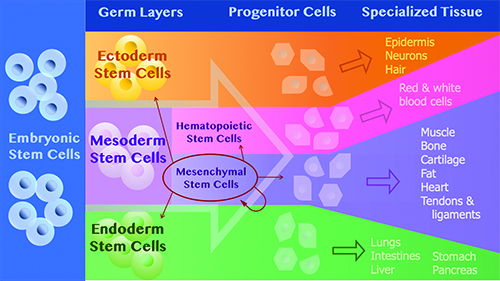
Early in development, ESCs differentiate into one of three germ layers, each of which gives rise to certain parts of the fetus. The endoderm (endo = inner) gives rise to many internal organs, including the lungs, pancreas, stomach, and liver. The mesoderm (meso = middle) gives rise to bone, cartilage, tendons, ligaments, muscle, heart, fat, and some nervous tissue. The ectoderm (ecto = outer) gives rise to neurons, outer layers of the skin and hair. As ESCs divide they produce new SCs that are specialized to one of these layers. Those SCs produce more SCs as well as “progenitor cells,” the precursors to specialized cells that compose distinct tissues.
The mesoderm lineage produces mesenchymal stem cells (MSCs) which are the cells used for therapy. The MSCs are considered multipotent (as opposed to pluripotent) because they can give rise to a limited number of tissues. MSCs and SCs from the other two lineages are present in the fully developed organism but are dormant or inactive until they are needed. They are activated by injury or disease at which time they begin proliferating and differentiating.
Upon hearing what I now do for a living, friends sometimes ask me: Isn’t stem cell therapy controversial? In our context, no! The controversy involves the use of embryonic stem cells. There are objections to their use in humans from ethical and religious points of view. Also, from a clinical perspective, ESCs have proven to be difficult to employ properly and in some cases hazardous. Because of their highly proliferative nature they can actually replicate too much. This can lead to mutations in the cells which can result in cancer.
What we use are adult stem cells. There are no ethical concerns because the cells can be extracted from a living organism with minimal risk. For SC therapy in the veterinary context the cells are taken from the same animal who will use them for therapeutic purposes. And because adult stem cells are less “hot” in terms of proliferation their genome remains much more stable essentially eliminating the concern of developing cancer.
PUTTING STEM CELLS TO THERAPEUTIC WORK
There are plenty of adult SCs in an adult organism. They are typically dormant and become activated in response to tissue damage or disease, which begins a complex cascade of cellular and chemical signals. The local SCs become activated and migrate to the specific area and proliferate to create more stem cells as well as progenitor cells to replace specialized cells (like cartilage or bone) that have been impaired.
Importantly, MSCs can be used to treat tissues to which they do not give rise; their main function in those cases is to activate the SCs in that tissue. SCs also modulate the immune system, decreasing the inflammatory response. The primary function of the stem cells used for therapy is to directly (in the case of tissues of the mesoderm lineage) or indirectly (for endoderm or ectoderm lineages) regenerate healthy tissue to replace what is damaged or diseased.
So, in cases of arthritis or dysplasia where there is damage to bone or cartilage, the MSCs produce and become those cells; in cases of ligament damage they produce ligament cells. In cases of the other two lineages the MSCs stimulate the SCs of that lineage to produce new cells, such as liver cells or skin cells. Since it causes the body to regenerate new, healthy cells, SC therapy is often referred to as regenerative medicine.
To undertake stem cell therapy we must first extract the MSCs, concentrate them, and then get them to the area of injury or disease. The closer the cells can be placed to the specific site of trouble the better. For cases of arthritis the MSCs are injected into the diseased joint; for areas or organs where injection is not possible MSCs are administered intravenously. As the SCs travel through the blood to reach various organs they are available to respond to specific areas of distress in those tissues.
Most dogs who receive SC therapy will need to receive multiple treatments. The time between treatments depends on the individual. Repeat treatments are given anywhere from one to two months to a year or so apart. In my work I’ve seen a few cases where the problem has ceased after one treatment. This is not common, but it does happen.
TREATMENT PROCESS
For SC therapy, MSCs are extracted from the body of the animal to be treated. They are present in tissue such as bone, fat, skin, brain, and heart.2 Initially SCs were extracted from bone marrow. However, there is a greater abundance of MSCs in adipose (fat) tissue, and this tissue is less traumatic to harvest, so this is the source used most frequently.
There are a few sources of adipose tissue in a dog. Some vets take fat from the scapular (shoulder) area. Others, including the veterinarian I work for, Dr. Robert Hagler in Lafayette, California, prefers to use fat from the umbilical area. This is a relatively simple procedure, but does require general anesthesia.
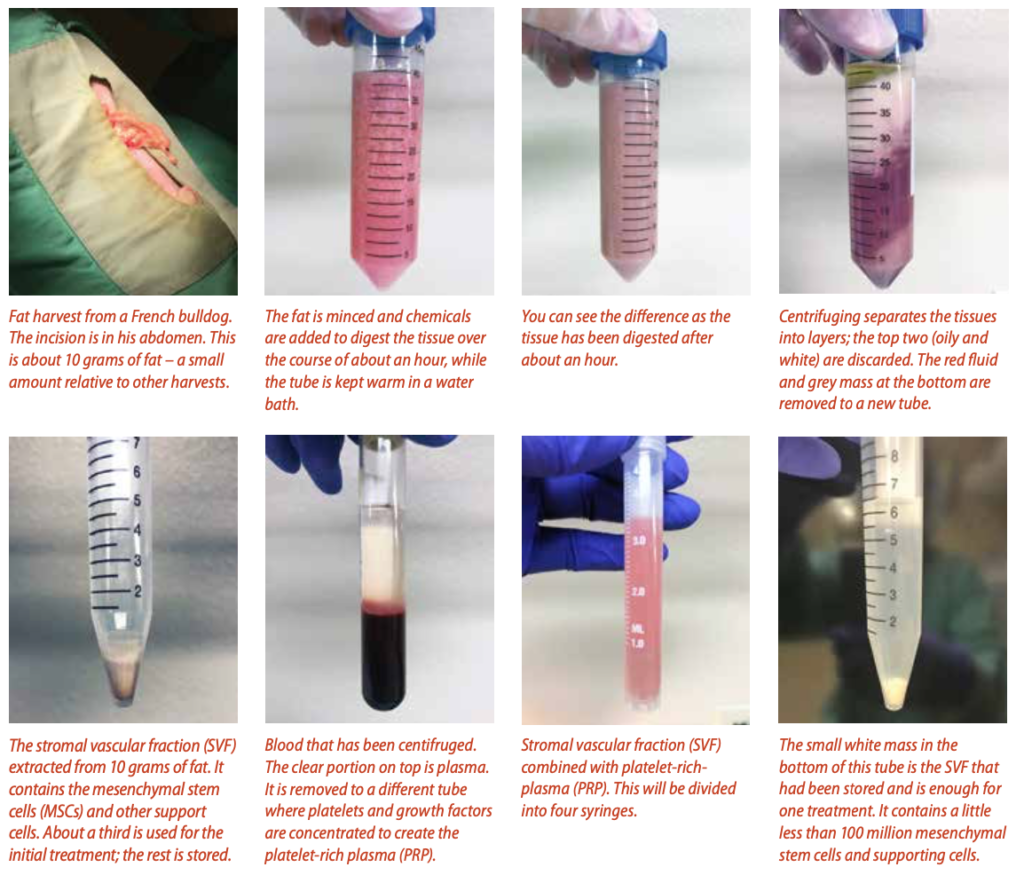
After removal, the fat is processed to extract the stem cells from the tissue (that’s my job!). The tissue goes through several mechanical and chemical digestion and separation steps. After a few hours the output is the stromal vascular fraction (SVF), which has concentrated mesenchymal SCs as well as other cells and components that support the action of the MSCs. Depending on the veterinarian, the SVF may be extracted on-site, in which case the dog is treated the same day (at the clinic where I work, we do the processing in-house). The majority of vets send the fat off to be processed and the SVF is returned for treatment on the second day following harvest at which time it is administered to the dog.
Usually, there are plenty of cells from the fat harvest for multiple treatments, depending on the condition being treated. The SVF needed for the initial treatment is slightly diluted in sterile saline and divided up to accommodate the number of injections to be made. Platelet-rich plasma (PRP, more on this below) is usually added to the SVF to further support the stem cell response. We usually save a small portion of SVF to be given intravenously. Extra fat containing cells for future treatments is sent off to be processed and the cells cryogenically frozen.
In most cases the dog is sedated for injection. If you’ve ever had an injection into a joint, you know that they are quite painful and that it is much easier on the dog to be sedated. If MSCs are administered only via IV, sedation is typically not necessary. Once the injections are complete, the sedation is reversed, and the dog can go home once he has fully recovered.
Future treatments are simpler, since the fat harvest and cell extraction has already been completed. In our office the dog comes to the office in the morning and has blood drawn for PRP. The blood is processed to obtain the PRP while thawed SVF goes through steps to wash and activate the MSCs. Once both components are prepared, they are administered as described above.
For joint injections, the first few days following treatment can be more painful than pre-treatment. The time for positive results to be evident varies from dog to dog. The average is a matter of weeks, but in some cases we’ve seen positive results in a few days, and there are times where it takes a month or two.
PLATELET-RICH PLASMA
Many vets accompany the MSCs with platelet-rich plasma. This substance helps amplify the signals from the injured or damaged area and directs the MSCs to that area. It helps to get the most out of the MSCs that are used. PRP also uses the dog’s own tissue – in this case, blood, which is drawn on the day of treatment. It is processed using a series of separation steps to concentrate platelets and a number of growth factors present in blood, and then the PRP is activated. It is combined with the SVF and administered with it in the injection.
In our office we sometimes use PRP outside of SC therapy to help promote healing. The most striking example of its efficacy I’ve seen was when two dogs had tibial plateau leveling osteotomy (TPLO) surgery for a ruptured ACL on the same day. Both had previous TPLO surgery on the other rear leg. PRP was administered to the surgical site once the procedure was complete. According to the owners and Dr. Hagler, both dogs had shorter recovery times compared to their previous surgeries and were using the surgical legs much sooner.
RISKS
Stem cell therapy is very safe. The MSCs used for therapy are autologous, meaning they come from the same dog who will receive them, so there is no risk of rejection. There are essentially no side effects from the treatment itself. The treatment process is rooted in the biology of the animal utilizing the natural healing properties of his or her own cells.
The most significant risk of the therapy has to do with the general anesthesia required in order to surgically remove some fat from the dog. There is always some risk in surgical procedures requiring anesthesia – more so for older or frail dogs. In addition, there is some risk of infection, since injections are often given into joints. To mitigate this risk, injections of MSCs are often accompanied by a small dose of antibiotic.

Rocco is a 10-year-old black Labrador Retriever. Thirteen months ago he had his first stem cell treatment to address a number of issues including arthritis in both hips and a neurological issue causing weakness in his rear end. The pain from his hips combined with the rear end weakness made it increasingly difficult for him to get around. Rocco’s owner, Vicki, says that he would squat to urinate and couldn’t get back up.
He also had masticatory myositis – an autoimmune condition that causes the muscles involved in chewing to become inflamed and very painful. Rocco was unable to open his mouth without terrible pain. To add to that he had neurological problems that affected his head and neck resulting in laryngeal paralysis. He had such a smorgasbord of neurological symptoms it was difficult to give him a definitive diagnosis.
Before he was hindered by his conditions Rocco was an active dog with a lot of pep. He loved his long walks at a local park. He let his family know he was ready for a walk by picking up his leash in his mouth. He caught treats that were tossed to him. And he would jump up onto the couch to hang out with his family. Vicki describes the heartbreak of seeing Rocco so impaired by pain that he wasn’t able to pick up his leash or jump up to the couch, and when they arrived at their favorite walking spot Rocco wouldn’t get out of the car. Because of the loss of musculature of his head, he looked very different, like his eyes were sunken in. She describes him looking like a skeleton. Rocco was on medications for pain and prednisone for the masticatory myositis but was getting little relief. Vicki was afraid this was the end of Rocco’s life.
She and Dr. Hagler decided to try stem cell therapy, and the results were amazing. Rocco received injections in both hips, intervertebral injections in his lumbar and sacral spine, and stem cells via IV for his head, jaw, and neck. The day after his treatment he was frisky and happy. He returned to his usual exuberance about his daily walks. And, his masticatory myositis and laryngeal paralysis resolved, and have not been apparent since.
While not necessarily one of the targets of his SC therapy, Rocco also had a long history of digestive issues. Despite years of trying to identify and treat the problem, nothing seemed to help. Rocco had diarrhea about every other week. He hasn’t had an episode of diarrhea since his SC treatment. Added to the success for the symptoms that were targeted this was an unexpected and wonderful surprise!
Rocco just came back in for a follow-up treatment, as Vicki had noticed some of the signs of his hip pain and rear end weakness returning. Again, he received injections in his hips and between vertebrae, and stem cells via IV. The next day Vicki described him as “super spunky” for the walk they had just been on. She describes Rocco’s experience being “like a miracle” and is so thankful to have her happy dog back, noting that Rocco’s improved health has been therapeutic for the whole family.
EXPECTATIONS
As I mentioned, SC therapy has been used most often in the treatment of arthritis, and with significant improvement in pain levels, range of motion, and functional mobility. Our practice has also used it in many cases of hip or elbow dysplasia, with excellent results in very young dogs with severe dysplasia.
One example is Tugboat, a chocolate Lab who was debilitated by elbow dysplasia when he was just four months old. His owner tried everything, including costly surgery, pain meds, therapy, etc.
Searching for other options she decided to try SC therapy. Following treatment, Tugboat is a different dog! He could hardly tolerate walking before, but now walks over an hour a day and plays at the beach. He comes in for repeat treatments every six months or so, when he starts showing signs of pain and decreased mobility, and soon returns to his normal activities.
MSCs are also used to treat damaged tendons and ligaments. SC therapy is helpful for partial tears, but not if the ligament is completely ruptured; there is simply not enough material to bridge a complete tear. At the clinic where I work, we have used SCs to treat degenerative myelopathy with good results. There have been a number of small scale (n=10 or less in most cases) studies that found SC therapy improved the condition of dogs with arthritis, dysplasia, intervertebral disc disease, perianal fistulas, inflammatory bowel disease, and keratoconjunctivitis sicca.3
Some dogs show improvement very early after treatment; others take longer, and the degree of improvement varies. However, says Dr. Hagler, “I’ve never seen a dog that didn’t have some improvement.”
Overall, the literature3 concurs that SC therapy is effective, though many studies or reports are anecdotal, based on practitioners’ data and experience; few clinical trials have yet been completed, though the companies whose technology is used to extract the SCs have studies in the works.
THE FUTURE OF STEM CELL THERAPY
The exciting possibilities for future directions of stem cell therapy mainly concern the source of cells used to treat patients. Currently the dog being treated must be the source of the cells used for treatment – otherwise the treatment would be legally considered a drug and must first gain approval from the U.S. Food and Drug Administration (FDA).
Having a stem cell “bank” would be a great help in the cases of dogs who lack enough fat to harvest or dogs who are too frail to undergo general anesthesia for surgical fat harvesting. Just as dogs can be universal recipients of blood, they can also safely receive stem cells that came from another dog. One study even found that MSCs can be extracted from human adipose tissue and transplanted into dogs.4 (Anyone have some fat you’d like to donate?)
Transplantation of MSCs from another animal would be a game changer. There are cases where the dog with banked cells doesn’t need them anymore, either because they’ve stopped doing therapy or because they are deceased. It would be ideal if the dog’s owner could make the banked cells available to other dogs. Currently this is not legal.
It’s possible to grow MSCs (but not supporting cells) in a lab to increase their numbers, reducing the need to harvest fat more than once; one company does that now.
You may be thinking that this sounds like something that may help your dog. Here are the next steps.
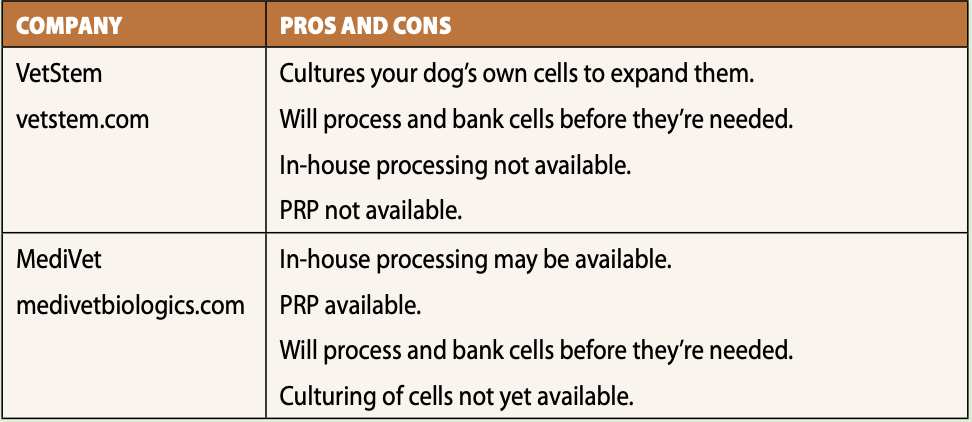
The first is to find a veterinarian who offers SC therapy. All veterinarians who provide this therapy work with one of two companies that provide the equipment, reagents, processing, and storage of cells: VetStem Biopharma and MediVet Biologics. The details of how services are offered depend to some degree on the company with which the vet’s office works.
VetStem has been doing SC therapy for animals for the longest time. VetStem currently cultures the animal’s MSCs, while MediVet does not, although they are working in that direction. VetStem does all the processing at their own facility.
MediVet provides training, equipment, and reagents to vet hospitals that choose to process cells in-house. Not all hospitals working with MediVet choose to do this, so in those cases, MediVet does the processing. The beauty of doing the processing onsite is that the fat harvest and initial therapy can be done in the same day. If you have to travel a distance to a vet for SC therapy, it certainly isn’t ideal to have to make multiple trips within a few days of each other for the initial therapy.
PRP can also be done onsite. VetStem does not incorporate PRP into their SC therapy.
Both companies store SCs for future use and can bank cells even before treatment is needed. If your dog is undergoing anesthesia for another procedure, like a spay or neuter, your veterinarian can harvest fat at that time and ship it to the company, so they can extract and freeze the cells for any future use your dog may need. If you have the foresight (and funds) to do this, it could eliminate the need to put your dog through fat-harvesting surgery later, when he may be less able to tolerate general anesthesia. When I am ready to have my dog neutered I will likely do this.
Depending on where you are located the choice of which company to utilize for the SC processing may be narrowed down for you simply by the vets who offer SC therapy in your area. Check with your veterinarian. You can also check the VetStem and MediVet websites; they can put in you in contact with one of their partner veterinarians near you.
CONSIDERATIONS BEFORE PROCEEDING
There are some cases where SC therapy is contraindicated. Because of the proliferative and immune-modulating effects of SCs, therapy should not be done for dogs who are known to have or suspected of having cancer. Neither should dogs who have an active infection receive therapy.
SC therapy may also not be an option for dogs who are lacking sufficient fat (until there is a stem cell bank for dogs!) or dogs who are too frail to withstand general anesthesia.
Stem cell therapy is not inexpensive; the cost for the initial treatment, including adipose harvest, is in the neighborhood of $2,500. Follow-up treatments can run $500 to $1,000. These numbers will vary from vet to vet. The good news is that many pet insurance plans now cover SC therapy. Even without insurance it is substantially less costly and less invasive than more drastic measures like joint replacement.
SC therapy is not a panacea and getting the greatest benefit requires basic but sometimes overlooked actions. It’s important to support the health of the whole dog: Keep his nails trimmed so they don’t interfere with walking. Feed a quality diet that supports overall health. Take precautions to prevent infection following surgery. Keep up with follow-up treatments in a timely manner to minimize the amount of pain or dysfunction the dog experiences. Supporting the dog’s overall health and providing him with quality care is imperative in getting the most out of treatment.
Joanne Osburn is the stem cell technician at Mt. Diablo Veterinary Medical Center in Lafayette, CA. After working for nine years as a biology tech at a government laboratory, she is delighted to be working in the veterinary field where she can help improve the lives of pets. She lives in the San Francisco Bay area with her husband Paul and super silly dog Guster.
1 Fortier LA, Travis AJ. “Stem cells in veterinary medicine.” Stem Cell Research & Therapy 2011; 2:9.
2 Markoski MM. “Advances in the use of stem cells in veterinary medicine: From basic research to clinical practice.” Scientifica 2016; 2016: 4516920.
3 Hoffman AM, Dow SW. “Concise review: Stem cell trials using companion animal disease models.” Stem Cells 2016; 34: 1709-1729.
4 Lee SH, Setyawan EMN, Choi YB, et al. “Clinical assessment after human adipose stem cell transplantation into dogs.” J Vet Sci 2018; 19(3): 452-461.






I am wondering what improvement you see in dogs with degenerative myelopathy? As an animal massage therapist, these are often my most heartbreaking cases, with rapid degeneration and minimal treatment options.
Thanks for all the information!!
How do you go about finding a veterinary practice that does stem cell and PRP work?
My 13 1/2 year old Llahsa mix has fatty lipomas in many places. Would SC therapy aid in reducing these? Non are carcinogenic.
Thanks so much
Can you give a ball park figure of the costs associated with a canine treatment plan (Labrador or Golden size) for arthritis in the lower back and hip joints
You are my breathing in, I have few blogs and infrequently
run out from post :).
Excellent article. I wonder why Roscoe needed injections in addition to IV. You should provide answers to comments.
EXCELLENT POINT ! I COULDN’T AGREE MORE, given the time this author spent putting a Lengthy article together for Us to read, and then doesn’t take the time to reply, seems rather unprofessional, imo.
My vet is wanting to use a bio stem patch to treat my dogs oronasal fistula. She is explained this is a new procedure using bio stems cells from the placenta of puppies (live puppies, no puppies are harmed). Its a patch of sorts, sewn over the fistula hole. She said this is a very new procedure. Has anyone heard of it? I cannot find any information on the internet about it.
I was talked into this treatment by an ambitious young Vet. I’m sorry to say it did not help my older German Shepherd. I felt badly for her. I adored her and thrn I put her through this.
Hi. What conditions were you attempting to treat? Did you end up seeing any improvement at all… I know the harvesting can/sounds a bit invasive but to me at least the attraction is the only downside is that it just doesn’t really help the situation, but might also perhaps be of benefit?
I have a puppy that has been diagnosed with osteonecrosis of her femoral head. I have read several articles about the use of stem cells to treat this condition. I am not seeing any veterinarians in the Saint Louis Mo. area that offers stem cell therapy. If anyone knows of any veterinarians in the area please post. I will check back