Oh, that dreadful retching – followed by the up-chucking of anything from green bile to undigested dinners to things we’d rather not think about. How can you tell whether your dog vomiting is serious enough for a vet visit or something you can treat at home? And what makes dogs throw up, anyway?
Vomiting is usually associated with gastritis, which describes inflammation of the stomach lining.
Acute gastritis causes dogs to vomit once or off and on for one or two days. The cause is usually some kind of dietary indiscretion, which includes the ingestion of spoiled food, garbage, cat litter, bones, plants, grass, molds, fungi, toys, socks, underwear, and other questionable items.
Fortunately, most dogs with acute gastritis recover without veterinary treatment. However, continued vomiting can lead to dehydration, depression or lethargy, blood in the vomit or feces, abdominal pain, a loss of appetite, or other complications that require medical attention. A dog who vomits repeatedly or can’t keep even water down should be seen by a veterinarian.
Chronic gastritis describes intermittent vomiting lasting more than one to two weeks. Prescription and over-the-counter drugs, infections, foreign bodies, various canine illnesses, or a prolonged exposure to allergens can be underlying causes. Chronic vomiting interferes with the digestion and absorption of nutrients. Dogs with this problem can become finicky, have low energy, and develop a dull, dry, poor-quality coat. Chronic gastrointestinal problems are rarely self-correcting, so intermittent vomiting that persists for longer than a couple of weeks should be investigated by your vet to help correct a problem in its early stages.
Signs of a Dog About to Throw Up
When dogs feel nauseated and are about to throw up, they often drool, lick their lips, swallow excessively, and stand head down looking worried. Many dogs look for or turn to their owners when they’re about to vomit, which can signal alert caregivers to move their pets to a better location! In time you might be able to train your dog to throw up where it does the least damage. Chloe, my Labrador Retriever, occasionally vomits after eating grass, organ meats, or lamb shoulder bones, and she usually races out the dog door in time to reach the back lawn.
If you don’t already keep a health notebook for your dog, start now with basic information. If and when your dog vomits, write down what happened and when, what the dog ate, what came up, how long after eating the vomiting occurred, and what happened next. Include details like the amount of material vomited, the vomit’s consistency (food, liquid, foam, etc.), the vomit’s color, frequency of vomiting (note the date and time), and general observations about your dog’s appetite, attitude, appearance, and general health. Take photos if you can, gross as it may seem.
Should your pet develop chronic gastritis, this record will help your veterinarian make an accurate diagnosis. Should your dog be sensitive to a certain food or treat, your written and visual record will help you discover the connection.
When Dogs Vomit on an Empty Stomach
Some dogs vomit when their stomachs are empty for too long, perhaps because of irritation from the stomach acid that collects there. This is commonly called empty tummy syndrome, or more formally, bilious vomiting syndrome. Affected dogs usually vomit bile and foam in the early morning hours but are otherwise completely normal. Offering a small meal just before bedtime usually solves the problem.

If feeding more frequent meals doesn’t help, the cause could be a foreign body, which is the general term for something a dog swallows that can’t pass through the digestive system. Anything that stays in the stomach for too long causes irritation and can lead to vomiting, especially when the stomach is otherwise empty.
It’s a relief when a dog throws up something he shouldn’t have swallowed in the first place and the evidence explains what happened. But sometimes it’s a mystery, especially when X-rays and ultrasound exams don’t reveal everything in a dog’s stomach.
In 2002, Lori Curry of McGaheysville, Virginia, couldn’t figure out why Race, her one-year-old Shetland Sheepdog, threw up every morning at 3 a.m. “He was eating well, looked healthy, and had normal bowel function,” she recalls, “but the vomiting went on for more than a month.”
In addition to interrupting Curry’s sleep, the formerly well-housetrained Race began having accidents in the living room.
For help, Curry turned to a canine nutrition forum, and WDJ contributor Mary Straus replied with ideas about what the problem might be, including swallowing a foreign object.
After an inconclusive ultrasound test, Race was scheduled for an endoscopy, a visual exam of the esophagus and stomach.
“I brought Race in for the appointment,” says Curry, “and in the lobby while waiting to be seen, he threw up a very slimy, very old, thin nylon sock!”
Problem solved, Race went back to being housetrained and sleeping through the night.
In 2014, Quiz, a six-year-old Golden Retriever belonging to Clyde Surles of Nashotah, Wisconsin, was treated for hookworms. At about the same time, she had intermittent diarrhea and began vomiting bile on an empty stomach. Prescription drugs can upset a dog’s stomach but symptoms like these don’t usually last for weeks after a protocol ends.

“The bile vomiting recurred whenever her stomach was empty for eight hours or more,” says Surles. “Her appetite remained good and she ate immediately after vomiting. But she was definitely not feeling as well as she normally did, and her coat became dull and dry.”Despite stomach-settling medications, a prescription diet, X-rays, lab tests, and an ultrasound exam, Quiz kept throwing up and no one knew why.Mary Straus encouraged Surles to schedule an endoscopy, and that exam revealed an inedible plastic decoration from a cupcake Quiz had swallowed, wrapper and all, nearly three months earlier. It was removed during the endoscopy, and Quiz has been fine ever since. “I’ve never been so happy and relieved,” Surles says.
Dog Food Can Cause Dog Vomiting
Not every food agrees with every dog, and food sensitivities can lead to stomach upsets. Repeated exposure to problematic food leads to chronic inflammation of the stomach and intestinal tract. If you suspect that this might be your dog’s problem, try switching to a food with different ingredients, add digestive enzymes to your dog’s dinner, give probiotic supplements, and/or experiment with different brands or types of food.
Wheat and other grains along with soy and other legumes can contribute to canine indigestion. When comparing labels, look for foods that list animal proteins first. Grain-free and soy-free foods have become popular because many owners and veterinarians report improved digestion and other health benefits in dogs after making the switch.
Transitioning from dry to canned food or to a raw or cooked fresh-food diet or upgrading to improved ingredients may make a difference. Check WDJ‘s annual ratings of dry and canned foods for recommendations. Feeding a home-prepared diet makes it easy to avoid grains and other ingredients to which your dog may be sensitive. See “Easy Home-Prepared Dog Food” by Mary Straus (WDJ July 2012) for guidelines. If feeding a commercially prepared raw diet, see “The State of the Commercial Raw Diet Industry” by Karen Becker, Steve Brown, and Mary Straus (September 2015).
Dry food can trigger vomiting because it absorbs moisture in the stomach, expanding in size and causing regurgitation. Soaking dry food before feeding or mixing dry with canned food may help.
Rotation diets can help identify problem ingredients. In a rotation diet, you feed a different type or family of food every day for four or five days before repeating a food, such as chicken on Monday, beef on Tuesday, lamb on Wednesday, and salmon on Thursday. Monday is the only day for eggs because they come from chickens. Salmon oil can only be given on Thursday. Waiting four or five days before repeating a food is thought to give the body sufficient time to eliminate it so it no longer triggers symptoms.
Because it’s practically impossible to perform a good rotation diet test while feeding commercial pet food – there are too many overlapping ingredients – some dog lovers prepare their own simple menus for a month or so. This requires keeping careful track of ingredients and the dog’s reactions. Feeding a limited diet for up to a few weeks is safe for adult dogs, though not for growing puppies.
A dietary elimination trial takes a different approach by eliminating every food ingredient the dog has ever eaten, and replacing them with food ingredients the dog has never experienced. As explained in “Food Elimination Trial: A Valuable Tool (When Done Correctly)” in the April 2011 issue of WDJ, a valid food elimination trial consists of three phases: elimination, challenge, and provocation.
In the first (“elimination”) phase, the owner identifies and chooses a single protein source and single carbohydrate source that the dog has never eaten, such as pheasant and barley or rabbit and amaranth. The dog is fed these two ingredients and nothing else – no leftovers, bones, chews, treats, or supplements are allowed. If the dog goes for eight to 12 weeks without vomiting or showing other signs of digestive distress, those two ingredients are probably safe to feed on an ongoing basis. If, however, the dog shows distress, a new trial is begun, using a diet with another novel protein and another novel grain. (If, after these two trials, you still see no improvement, the problem is probably not linked to food allergies.)
Many people stop the experiment once their dogs improve on an elimination diet of the two novel ingredients. But to prove that there were ingredients in the dog’s former diet that were causing his symptoms, one should undertake a second (“challenge”) phase of the trial. Resume feeding the dog whatever food he used to be fed and watch to see whether the old diet again triggers vomiting or other symptoms within one week.
In the third (“provocation”) phase, you would go back to feeding the effective diet (consisting of the novel protein and novel carbohydrate that did not trigger the dog’s symptoms) – only now, once your dog’s condition has again stabilized, you’d add a single new ingredient. If the dog develops symptoms, remove that ingredient and try something else. Eventually you’ll have a variety of ingredients that agree with your dog, and you’ll know which foods trigger problems.
As noted in WDJ‘s 2011 article, “This is not a fun project. It takes commitment, extraordinary observation, and total control of your dog’s environment for weeks on end. However, identification of the ingredients to which your dog is allergic will enable you to simply prevent him from eating those ingredients, and stave off both the uncomfortable symptoms of allergy and the potentially hazardous treatments sometimes required to make him more comfortable.”
Whatever you feed, keep your dog’s food bowl and water bowl clean. Consider switching from plastic serving bowls to ceramic or stainless steel in case your dog is sensitive to the chemicals in plastic.
Some Dogs Eat Too Fast
One common reason for canine vomiting is eating too much or too fast. If your chow hound inhales his dinner, try the following strategies:
1. Feed your dog alone rather than with other pets, as the threat of competition can lead to stress and rapid eating.
2. Spread food over a cookie sheet, so it takes longer to find and swallow.
3. Feed multiple small meals during the day rather than one or two larger ones.
4. Place an unopened soup can, smooth stone, clean brick, or similar heavy object in your dog’s bowl along with food, which will slow your dog’s eating. Be sure the object is larger than anything your dog can swallow.
5. Try a “slow feeder” bowl with raised bumps or dividers that prevent a dog from eating quickly.
6. Feed treats in Kong toys, food puzzles, or other devices that prevent immediate swallowing.
7. Scatter your dog’s food outdoors on the lawn, indoors on an easy-to-clean kitchen floor, or on a “snuffle mat” – a fabric mat with long fibers that hide the kibble and force the dog to sniff out and lick up each piece of kibble individually.
8. If you feed raw meaty bones, try teaching your dog to chew (rather than swallow things whole) by holding one end while your dog tackles the other.
What to Do For Dog Vomiting
If your dog vomits after ingesting or being exposed to something dangerous, time is of the essence, so go at once to a veterinary clinic.
As mentioned, most cases of acute gastritis resolve on their own without medical intervention. Here are six nonmedical steps for treating acute gastritis in dogs who otherwise appear and act bright, alert, and normal.
1. Withhold food for 24 hours, which gives the digestive tract an opportunity to rest.
2. Provide small amounts of water every hour or so. If a small amount of water provokes vomiting, seek veterinary treatment.
3. After 24 vomit-free hours, feed small amounts of a low-fat food that is easy to digest. Some veterinarians recommend small amounts of a bland diet such as white rice and skinless, boneless chicken.
4. After that, resume feeding small meals totaling half of your dog’s regular daily diet, divided into four or six servings.
5. Over the next two to three days, gradually increase food amounts to normal levels.
6. Notify your veterinarian if vomiting resumes.
When to Call the Vet
In addition to notifying your veterinarian if your dog continues to vomit, be ready to call for help when:
– The vomiting is severe and comes on suddenly.
– Your dog has a fever or is lethargic or in pain.
– You know or suspect that your dog swallowed a foreign object.
– Your dog has bloody diarrhea.
– There is blood in the vomit or it has an unusual color or consistency (save a sample for your vet).
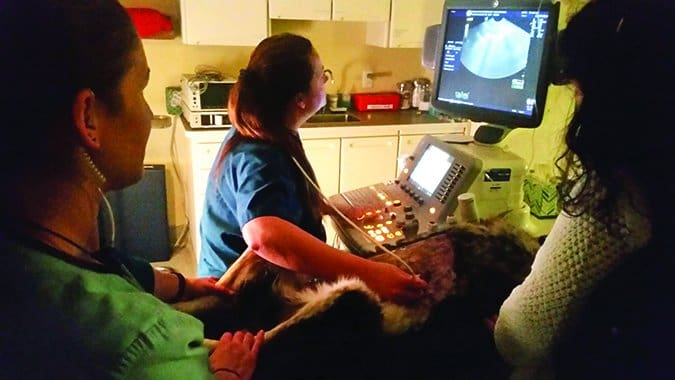
If medical care is needed, your veterinarian may take an X-ray or do an ultrasound in an effort to discover what your dog might have swallowed. Blood tests may be useful to help rule out other causes such as pancreatitis or acute kidney failure. Surgery may be required to remove an object that blocks the intestines or a large object in the stomach, such as Gorilla Glue, which swells to a large mass after ingestion.
If no cause is discovered, you may need to consult a specialist for an endoscopy, where a tube is inserted through your dog’s mouth and esophagus into the stomach. Small objects in the stomach can be removed with the endoscope. If no obvious cause is found during endoscopy, a biopsy of the stomach lining can be taken to provide additional information.
Your dog might be treated with gastrointestinal protectants such as sucralfate (Carafate), an anti-ulcer medication; with anti-emetic or anti-vomiting medications such as metoclopramide (Reglan or maxolon), H2 (histamine-2) receptor antagonists such as famotidine (Pepcid) or ranitidine (Zantac), which are used to reduce stomach acid; or proton pump inhibitors such as omeprazolie (Prilosec or Losec), which are used in cases of severe stomach ulceration.
Should You Make Your Dog Throw Up?
Veterinary exams, lab work, X-rays, ultrasound tests, endoscopies, and surgery are expensive, so we do what we can to avoid them. Still, dogs will be dogs. Let’s say you just saw your dog swallow a sock. What should you do?
Several online forums and blogs give detailed directions for making dogs vomit with emetic agents such as hydrogen peroxide or by using other methods. However, inducing vomiting is not always the best option. We recommend consulting your veterinarian or the ASPCA’s Animal Poison Control Center (888-426-4435) before taking such a step.
Note that some widely recommended methods are potentially harmful. Syrup of ipecac, which for decades was given to pets and people, is no longer considered the standard of medical care because of its toxic effect on the heart and circulatory system and because it tends to result in prolonged dog vomiting, lethargy, and diarrhea. Sticking your finger down a pet’s throat to stimulate a gag reflex (called digital vomiting induction) can result in injury to both you and your pet. Soaps, mustard powder, and table salt are not reliable, and their potential toxicity is a concern.
Instead, follow these instructions from the ASPCA’s Animal Poison Control Center. Read through them now so you understand the basic procedure, keep a copy with your dog’s health notebook, keep the necessary supplies on hand, and review the instructions again before calling for help.
1. Contact your local veterinarian or call the ASPCA’s Animal Poison Control Center at (888) 426-4435 or the Pet Poison Helpline at (855) 764-7661. Both hotlines are staffed 24 hours a day, seven days a week, and are available to pet owners at a small charge.
2. Be ready to describe your dog’s breed, age, approximate weight, any health problems the dog suffers from, what he may have eaten, and when he may have eaten it. If you are instructed to induce vomiting at home, proceed as described below. Otherwise follow the directions given by the veterinarian you have spoken with.
3. To induce your dog vomiting, assemble these supplies: a fresh, new, unopened pint or quart of 3-percent hydrogen peroxide, available at any drug store or supermarket; a large syringe (no needle) or turkey baster; a measuring teaspoon; latex or rubber gloves; paper towels; water; cleaning solution; and plastic bags.
4. If the dog has not eaten within the last two hours, offer a small meal. This makes it more likely that the dog will vomit, but is not essential if the dog is uninterested in food.
5. Measure 1 milliliter (ml) of 3-percent hydrogen peroxide per pound of dog weight, using either the syringe or teaspoon. One teaspoon is approximately 5 ml, so this is about one teaspoon per five pounds of body weight. There are three teaspoons in a tablespoon, so a 15-pound dog would need one tablespoon. The maximum amount of hydrogen peroxide to give at any one time is 45 ml, (about nine teaspoons, which is three tablespoons) even if a dog weighs over 45 pounds. Squirt the hydrogen peroxide into the back of the dog’s mouth using the syringe or turkey baster.
6. If vomiting has not occurred within 15 minutes or so, give one more dose of hydrogen peroxide measured as described above. If vomiting still does not occur, call back to your veterinarian or the pet poison control center hotline for instructions. It’s important that the hydrogen peroxide not remain in your dog’s stomach.
7. Once vomiting occurs, collect a sample in a leak-proof container. Bring this to your veterinarian’s office for identification, especially if you are unsure of exactly what your dog may have eaten.
8. Unless instructed otherwise by your veterinarian or the pet poison control center hotline, immediately take your dog to a veterinary clinic for evaluation.
Of course, if you are concerned, don’t wait for a veterinary receptionist to insist that you bring your dog in; they don’t know your dog like you do. A case in point is Lori Curry’s other Sheltie, Raz, who was famous for eating paper money, a utility glove that he passed whole, and a dryer sheet that made him sick until he vomited it up a week later. When he was 14, Raz grabbed and ate a raw corn cob from the back of a kitchen counter. Curry called an emergency clinic. “They recommended taking a wait-and-see approach,” she says.
As the veterinarian predicted, Raz passed most of the corn cob safely. But five days later, he suddenly declined, and despite thousands of dollars for surgery and round-the-clock emergency care, he almost died. “Corn cobs are dangerous, and when another time my dogs got into corn cobs, I insisted on inducing vomiting. I don’t take a wait-and-see approach for that problem anymore!” Curry says.
Canine Diseases That Can Cause Dog Vomiting
All kinds of illnesses trigger gastritis, so a dog vomiting is never a defining symptom by itself. Here are several conditions that cause vomiting in dogs.
Bloat
Also known as gastric dilation-volvulus or torsion, bloat is a serious condition affecting all types of dogs but especially large breeds with deep chests like Akitas, Great Danes, German Shepherd Dogs, and Doberman Pinschers. Dogs at greatest risk are those who rapidly eat a single large meal once daily – or dogs who break into food supplies and overeat. Gastric distention occurs as the stomach fills, and physical activity shortly after eating can cause the stomach to twist, which closes the esophagus and leaves the dog unable to expel gas or excess food by vomiting or belching. Symptoms include a distended abdomen, pain, drooling, and repeated, unproductive attempts to vomit.
Bloat is a medical emergency of the highest order; immediate veterinary attention is essential.
Parasites
Although roundworms tend to cause diarrhea rather than start a dog vomiting, if the infection is severe a puppy may vomit live worms. Other parasitic infestations can contribute to gastrointestinal symptoms.
Giardia, an intestinal parasite caused by a single-celled organism, affects an estimated 11 percent of all pets and up to 50 percent of puppies. It is easily transmitted through contaminated food, water, or soil, and through pet-to-pet contact. Giardia infections cause diarrhea and vomiting, although a dog may go without obvious symptoms for long periods. Coccidia, another single-celled organism that infects the small intestine, can produce vomiting, watery stools, bloody diarrhea, fever, depression, and life-threatening dehydration.
Multiple fecal parasite and giardia tests may be needed before these causes can be identified or ruled out because “false negative” results can occur for various reasons. Empirical treatment with fenbendazole (Panacur) for giardia and most intestinal worms, or diluted Ponazuril for coccidia, may be tried to see if symptoms improve.
Pancreatitis
Inflammation of the pancreas can cause diarrhea, vomiting, abdominal pain, and a loss of appetite. Because its symptoms are shared by so many other canine illnesses, pancreatitis can be difficult to diagnose, though there are now blood tests for canine pancreas-specific lipase that are more accurate for diagnosing both acute and chronic pancreatitis. In cases of chronic gastritis, your vet will look for underlying causes, including pancreatitis.
Inflammatory Bowel Disease (IBD)
This is another hard-to-diagnose digestive illness. In IBD, inflammatory cells take over the intestine, leading to scar tissue throughout the digestive system’s lining and chronic vomiting, diarrhea, and weight loss.
Liver Disease
This can trigger the dog vomiting bile, which tends to be thin, clear, yellow, or brown and sometimes frothy. The stool can become ribbon-like and have an orange tint. A bile acid test can confirm the diagnosis.
Addison’s Disease (Hypo-Adrenocorticism)
Caused by adrenal insufficiency, Addison’s can produce vomiting, diarrhea, fatigue, loss of appetite, and general weakness that tends to come and go over time. While Addison’s is a treatable condition, an Addisonian crisis in which the patient goes into shock can be fatal. See “Detecting Addison’s Disease in Your Dog” (WDJ October 2011) for information on Addison’s.
Peritonitis
This is an umbrella term for any inflammatory or infectious disease of the visceral lining (peritoneum) of the abdomen. It usually involves most of the abdominal organs (liver, stomach, intestines, spleen, kidney, reproductive organs, and bladder). Peritonitis results in the accumulation of fluid within the abdominal cavity. It can be associated with abdominal trauma, abdominal surgery, or pancreatitis. Its symptoms include vomiting, diarrhea, weakness, fever, loss of appetite, abdominal distention, and abdominal pain.
Pyometra
An infection of the uterus, pyometra is most common in intact females who have never been pregnant. Most are age six or older. The infection occurs after a heat cycle that does not result in pregnancy. Symptoms can include vomiting, lethargy, depression, fever, lack of appetite, excessive thirst, frequent urination, a distended abdomen (due to the enlarging uterus), vaginal discharge, excessive licking at the area, and weakness in the hind legs. Some spayed females may develop “stump pyometra” from a remnant of the uterus left behind.
Hemorrhagic Gastroenteritis
This condition is unusual in dogs, but it can be frightening, expensive, messy, and sometimes fatal. The cause of hemorrhagic gastroenteritis remains unknown, but its symptoms, which can affect any dog at any age, are dramatic – slimy vomit followed by blood in the vomit and bloody diarrhea. If your dog develops these symptoms, seek veterinary treatment at once. See “Hemorrhagic Gastroenteritis in Dogs” (WDJ July 2009) for details about identifying and treating hemorrhagic gastroenteritis.
Other Causes of Dog Vomiting
In addition to illnesses and diseases, there are a number of things that dogs can ingest or be exposed to that can cause acute or chronic gastritis.
Antibiotics, Anti-Inflammatories, Chemotherapy Drugs, and Other Medications
All of these can have numerous side effects, including vomiting. The same is true for vitamin D poisoning, which can occur from supplementing too much vitamin D3 (see “Vitamin D for Dogs,” WDJ July 2016) or from ingesting rodenticides (drugs that kill rats and mice) that contain vitamin D3.
Exposure to chemical irritants can start a dog vomiting, as can heavy metal poisoning and other chemical exposures. Never induce vomiting when a caustic substance was swallowed. Describe the symptoms to your veterinarian and provide a list of medications and supplements your dog has been taking. In cases of rodenticide poisoning or chemical exposure, contact your vet or the ASPCA’s Animal Poison Control Center at once.
Plants, Fungi, and Bacteria
Dogs are famous for eating grass and throwing up, and most are none the worse for wear. But an alarming number of plants are toxic to dogs. See the ASPCA’s list of nearly 500 toxic plants.
The most common plants that are problematic for dogs are the autumn crocus (Colchicum autumnale), azalea (Azalea nudiflora), cyclamen (Cylamen spp.), dumbcane (Dieffenbachia), hemlock (Conium maculatum, which is a poisonous plant and not related to the coniferous hemlock tree), English ivy (Hedera helix), mistletoe (Viscum album), oleander (Nerium oleander), thorn apple or jimsonweed (Datura stramonium), yew (Taxus spp.), and any mushroom or toadstool that you cannot identify as safe. Avoid planting any of these near where your dog will walk or play.
Pythiosis is an infectious disease caused by a fungus-like organism, Pythiuminsidiosum, that inhabits wetlands, ponds, and swamps. Dogs can develop pythiosis after swimming in or ingesting contaminated water, and their key symptom is vomiting. While most cases occur near the Gulf of Mexico, inland dogs have developed it, too. Young male retrievers are especially at risk if they retrieve and then chew on sticks from infected water.
Cyanobacteria (also known as blue-green algae) are microscopic bacteria found in freshwater lakes, streams, ponds, and brackish water that can cause vomiting in dogs. The bacteria colonize to form “blooms” that give water a blue-green or “pea soup” appearance. Algal concentrations are most abundant during hot summer weather. While most blue-green algae blooms are not toxic, it is impossible to determine the presence of toxins without testing. Therefore, all algae blooms should be considered potentially toxic and avoided because even small exposures, such a few mouthfuls of algae-contaminated water, can be fatal.
Settling Doggy Stomachs
It’s encouraging to know that most dogs who vomit have acute rather than chronic gastritis, that its cause is probably benign, and that most vomiting dogs recover on their own without medical treatment.
But sometimes your dog vomiting is a serious symptom, and it’s worth studying its possible causes so that if and when your dog throws up, you’ll have a better idea of how to respond in order to keep your best friend healthy.
CJ Puotinen is author of The Encyclopedia of Natural Pet Care and other books.







Been there.
Can’t give Freyja Grey pig ears. I don’t think she can digest them or is just allergic. She loves them but both times has vomited in the middle of the night, sometimes also with diarrhea. Hasn’t done it since I’ve stopped giving them to both dogs.
When Diana pawPrints was a puppy, twice she ate my parent’s dog Candy’s food when there were meds in it. Both times I had to do the peroxide bit (after calling the vet.) Second time I had to give her a second dose as she didn’t the first time, plus was bigger so needed more. She’s 92 pounds now so thankful this is no longer an issue.
Neither swallow inanimate objects or cat poop or dead things they may find (like field mice). They do chew on sticks but thankfully do not swallow the pieces. For both it is just chew up and spit out. A whole other issue. Thankfully with the small yard rodents it is dead and done as they are no longer “fun”.
Sorry this is about a cat, but I’m sure it will work the exact same way for a dog.
Casey, my female cat, was born in my closet in 2003 (she is 17). She chooses to be an indoor cat. Despite the fact that she eats a good quality kibble, she had gotten to the point where she would throw up the food pretty much every day.
A few weeks ago, while doing further research on the PEMF devices that I sell, I found a recent scientific paper that proved that a man was able to normalize the kidney function of an elderly cat, using only PEMF.
I immediately began treating her with a PEMF device. After receiving the first treatments the vomiting slowed. In the next 2 weeks she vomited only two times, so we went from once per day to once per week, in only 2 weeks of treatments. The following 2 weeks she has thrown up exactly zero times. She appears to be cured.
It dawned on me, that exactly as I talk to people every day about the benefits of PEMF for home bound, mostly indoors people who are chronically cut off from the natural electromagnatism outdoors, so was my cat an “indoor cutoff”.
Many of you have heard me talk about how our bodies run on electricity, but what we have not been told is where do we get it, since we don’t plug ourselves in at night like a cell phone. Where does our electricity come from to run our body?
It comes from two places: 1. It rains down out of the sky, call the Shumann waves or frequencies. 2. It bubbles up out of the dirt and the ground. People (and cats I now realize) who are indoors all the time, are always cut off from their source of electromagnatism, which every living being requires.
Being cut off, or restricted from the earths electromagnetic field is the beginning of disease. Without the electromagnatism to charge the battery in the cells, the cell stops going through its sodium-potassium pump function (eat, drink, relieve waste) and instead it begins to simply stew in its own juices (or go to sleep). When a group of cells “go to sleep” like this, it is what we call a diseased organ.
Of course, if you take this diseased organ to a doctor, they only have three options: cut, burn or poison. When all the organ really needed was a good jolt of delicious, life giving electromagnatism.
I finally realized that poor Casey was suffering from the exact condition that I talk to people about all day long, every day.
I feel like the painter whose own house is in desperate need, and the cobbler whose kids are barefoot.
I would feel horrible if it had been too late for Casey, but fortunately, with PEMF, it is never too late to improve the quality of your life, and the lives of those around you, as long as you are still alive.
According to the Journal of Science and Medicine, renal failure is a leading cause of suffering and death in domestic cats, with approximately 1 in 3 cats affected.
This is the article that launched my newfound household happiness:
Reversal of Renal Insufficiency in an Aging Cat: A 5-year Multi-Crossover Case Study
https://www.josam.org/josam/article/view/30
This report chronicles the return to normal and then reversion to renal insufficiency in a single cat, when PEMF was applied, then withheld, then applied again, over three cycles of application and non-application, over a 5-year period.
Casey now recognizes that it is the coil that make her feel so much better, so she sleeps directly on it all the time.
I’m so happy that my little kitty is healed.